Foot and ankle billing 2026: Master Profit
Understanding the Foot and Ankle Billing Process
Foot and ankle billing is the specialized process of submitting and managing insurance claims for podiatric and orthopedic foot care services. It requires precise medical coding, thorough documentation, and strict adherence to payer-specific guidelines to ensure proper reimbursement.
Key Components of Foot and Ankle Billing:
- CPT/HCPCS Codes – Procedure codes like 11055-11057 (callus removal), 11719 (nail trimming), and G0127 (dystrophic nails)
- ICD-10-CM Codes – Diagnosis codes that establish medical necessity for services
- Modifiers – Special indicators like Q7, Q8, Q9 for systemic conditions, and -25 for separate E/M services
- Medicare Guidelines – Coverage rules for routine foot care based on systemic diseases like diabetes or peripheral vascular disease
- Documentation Requirements – Proof of medical necessity, active care dates, and provider NPIs
If you’re a podiatrist struggling with claim denials, delayed payments, or confusing Medicare rules, you’re not alone. The research shows that foot and ankle billing is among the most complex areas of medical billing—with strict 60-day frequency limits for routine care, mandatory referrals for certain insurance plans like United Healthcare HMO, and specific documentation requirements that can make or break your reimbursement.
The average foot or ankle surgery ranges from $5,000 to $20,000 depending on complexity and location. But getting paid for these procedures—or even routine nail trimming—requires navigating a maze of coding rules, modifier requirements, and payer policies.
Routine foot care is generally excluded from Medicare coverage unless specific systemic conditions are present. Services performed for patients with diabetes, peripheral neuropathy, or vascular disease require precise ICD-10 coding and Q modifiers to prove medical necessity. Miss one detail, and your claim gets denied.
Advanced diagnostics add another layer of complexity. Gait analysis and motion labs use CPT codes 96001, 96002, and 96004—but coverage varies widely by insurance, and patients often need to verify benefits beforehand.
This guide breaks down everything you need to know about foot and ankle billing: from essential CPT codes and Medicare compliance to preventing denials and understanding patient responsibilities. Whether you’re billing for in-office procedures or complex surgical interventions, we’ll help you optimize your revenue cycle and reduce administrative burden.
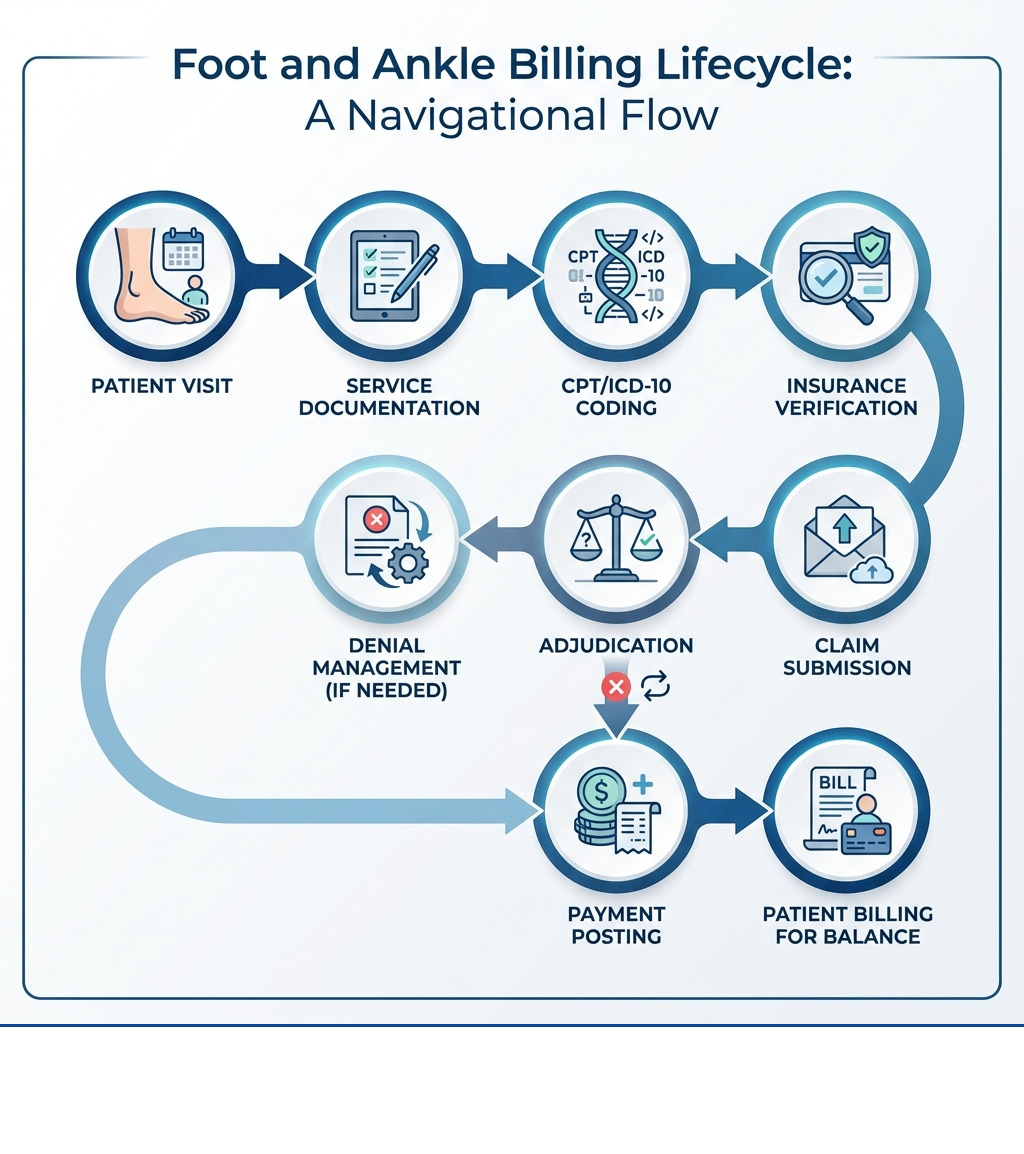
Essential Codes and the Role of CPT in Foot and Ankle Billing
At the heart of accurate foot and ankle billing lies the mastery of medical coding. This intricate language ensures that the services you provide are properly communicated to insurance payers for reimbursement. We rely on two primary coding systems: CPT (Current Procedural Terminology) codes for the procedures and services rendered, and ICD-10-CM (International Classification of Diseases, 10th Revision, Clinical Modification) codes for the diagnoses that establish medical necessity.
CPT codes are like the verbs of medical billing, describing what you did, from routine office visits to complex surgical repairs. ICD-10-CM codes are the nouns, explaining why you did it, detailing the patient’s condition. Together, they paint a complete picture for the payer. Without precise and compliant coding, even the most expertly performed procedure can result in a denied claim. Our goal is to ensure your practice’s financial health, and that starts with getting these codes right every time. For a deeper dive into these codes, check out our resources on Footing the Bill: A Podiatrist’s Handbook to CPT and ICD-10 Codes and The Foot-Friendly Guide to Podiatry Billing and Coding.
Essential CPT Codes for Foot and Ankle Billing
When it comes to foot and ankle billing, certain CPT codes are staples in every podiatry practice. These codes cover the most common services, from routine care to initial evaluations:
-
Debridement (11055-11057): These codes are used for the removal of benign hyperkeratotic lesions, commonly known as corns and calluses. The specific code you use depends on the number of lesions treated:
- 11055: Paring or cutting of benign hyperkeratotic lesion (e.g., corn or callus); single lesion
- 11056: Paring or cutting of benign hyperkeratotic lesion (e.g., corn or callus); two to four lesions
- 11057: Paring or cutting of benign hyperkeratotic lesion (e.g., corn or callus); more than four lesions
These codes replaced earlier ones for callus removal. If you debride one lesion on the right foot and two on the left, you would use code 11056 as it covers two to four lesions across all sites.
-
Nail Trimming (11719): This code is used for the trimming of non-dystrophic nails. This typically refers to nails that are normal in appearance but may require trimming for various reasons.
-
Dystrophic Nails (G0127): For the trimming of dystrophic nails (nails that are thickened, discolored, or otherwise abnormal), Medicare often requires the use of HCPCS code G0127. This code specifically addresses the medical necessity of trimming such nails, especially in patients with systemic conditions that put them at higher risk.
-
Evaluation and Management (E/M) Codes: These codes (e.g., 99202-99215 for office visits) cover the cognitive work involved in assessing a patient’s condition, making a diagnosis, and developing a treatment plan. They are crucial for every patient encounter.
-
Modifier -25: This little modifier plays a big role. When you perform a procedure (like debridement or nail care) on the same day as a significant, separately identifiable E/M service, you’ll append modifier -25 to the E/M code. This tells the payer that the E/M service was distinct from the procedure and should be reimbursed separately. It’s a key tool in ensuring you’re compensated for both the hands-on care and the diagnostic/decision-making process.
Navigating Foot and Ankle Billing for Surgical vs. In-Office Care
The billing landscape shifts significantly when comparing in-office procedures to surgical interventions in foot and ankle billing. While both require meticulous coding and documentation, the complexities multiply with surgery.
In-office procedures, such as minor lesion removals, injections, or routine foot care, are typically straightforward. You’ll bill for the professional service, any materials used, and potentially a separate E/M if applicable. The overhead is lower, and the billing process is relatively contained within your practice’s system.
Surgical interventions, on the other hand, introduce a cast of new characters to the billing stage:
- Facility Fees: When a surgery takes place in an outpatient surgical center or hospital, the facility bills for the use of its operating rooms, equipment, and nursing staff. This is separate from the surgeon’s fee.
- Anesthesia: Anesthesia services are typically billed by a separate provider or group.
- Pathology/Radiology: If specimens are sent to pathology or imaging is performed, these are also billed separately.
- Global Periods: Many surgical procedures come with a “global period”—a timeframe (e.g., 10, 30, or 90 days) during which all routine pre-operative and post-operative care related to the surgery is considered bundled into the surgical fee. This means you generally cannot bill separately for follow-up visits during this period. Understanding these global periods is critical to avoid duplicate billing and denials.
Accurate coding for surgical procedures involves not only the primary surgical code but also appropriate modifiers for bilateral procedures, assistant surgeons, or multiple procedures performed during the same session. The stakes are higher, and the financial impact of errors can be substantial. For strategies on maximizing revenue from various procedures, including surgical ones, consider exploring our insights on High-Profit Procedures: Smart Strategies & Your Guide to Podiatry Revenue Growth.
Medicare Guidelines and Routine Foot Care Compliance
Medicare’s rules for foot and ankle billing, particularly concerning routine foot care, are notoriously stringent. Generally, services like shaving, paring, cutting of corns or calluses, and trimming of non-dystrophic nails are considered “routine” and are excluded from Medicare coverage. This is because Medicare views these services as something a beneficiary or caregiver could perform.
However, there’s a crucial exception: if the routine foot care is medically necessary due to the presence of specific systemic conditions that pose a threat to the patient’s health, Medicare may cover it. These conditions include:
- Diabetes Mellitus Complications: Especially when accompanied by neuropathy (nerve damage) or poor circulation.
- Peripheral Vascular Disease (PVD): Conditions affecting blood flow to the lower extremities.
- Other Neurological Disorders: Such as multiple sclerosis or hereditary neuropathies, which can impair sensation or motor function in the feet.
The key is to demonstrate medical necessity through thorough documentation. You need to show that if a non-professional were to perform these services, there would be an increased danger of infection or injury due to the patient’s underlying condition. Medicare Administrative Contractors (MACs) publish detailed articles, such as Billing and Coding: Routine Foot Care (A56680), that outline these requirements. Understanding these guidelines is essential for compliance and reimbursement. For more comprehensive guidance, our Medicare Podiatry Billing Guidelines provide an in-depth look.
The Significance of Q Modifiers
When billing Medicare for routine foot care that falls under the “medically necessary” exception, Q modifiers are your best friends. These modifiers (Q7, Q8, and Q9) are essential to indicate the “class findings” that justify coverage due to the patient’s systemic condition and its peripheral complications. Without them, your claim for routine foot care will likely be denied.
Here’s a simplified breakdown of what each Q modifier generally signifies, based on Medicare guidelines:
- Modifier Q7: Indicates that one of the “Class A” findings is present, representing a severe systemic condition with peripheral involvement. These might include a history of previous ulceration, infection, or gangrene of the foot, or a non-traumatic amputation.
- Modifier Q8: Indicates that two of the “Class B” findings are present, showing a systemic condition with moderate peripheral involvement. Examples include intermittent claudication, dependent rubor (redness), or trophic changes (e.g., hair loss, skin atrophy).
- Modifier Q9: Indicates that all three “Class C” findings are present, demonstrating a systemic condition with severe peripheral involvement. This typically requires documentation of absent pedal pulses and dependent rubor.
The specific clinical findings that qualify for each class are detailed in Medicare’s billing and coding articles. It’s crucial for your documentation to clearly support the presence of these findings. These modifiers tell Medicare, “Hey, this isn’t just a cosmetic nail trim; this patient has serious underlying conditions that make this care medically essential to prevent worse outcomes.” Navigating these complexities can be tricky, but we aim to make it clearer. To learn more about what Medicare covers, check out Demystifying Medicare Podiatry: What’s Covered, When, and How to Calculate Costs.
Active Care Requirements
Beyond the presence of systemic conditions and the correct Q modifiers, Medicare imposes another critical requirement for certain routine foot care services: the active care requirement. This rule states that for specific asterisked ICD-10-CM diagnosis codes (which are detailed in Medicare’s various billing and coding articles), the patient must be under the “active care” of a Doctor of Medicine (MD) or Doctor of Osteopathy (DO) for the complicating disease process.
What does “active care” mean in this context? It means that the patient must have been seen by an MD or DO for treatment and/or evaluation of the underlying systemic condition (e.g., diabetes, peripheral vascular disease) within the six-month period prior to the date of the foot care service.
To comply with this, your practice needs to:
- Document Thoroughly: Ensure your medical records clearly show the patient’s systemic condition and the medical necessity for the foot care.
- Report the Date Last Seen (DPLS): On the claim form (e.g., CMS-1500, Line 19), you must report the approximate date the patient was last seen by their managing MD or DO for the complicating condition.
- Include the MD/DO’s NPI: The National Provider Identifier (NPI) of the treating physician must also be included on the claim.
Failing to meet these active care requirements or properly document them is a common reason for Medicare denials for routine foot care. It emphasizes the importance of good communication and coordination with your patients’ primary care physicians or specialists. Keeping your practice audit-proof means staying on top of these details. For more insights on compliance, see our guide on how to Audit-Proof Your Practice: A Guide to Podiatry Billing Compliance.
Advanced Diagnostics: Billing for Gait Analysis and Motion Labs
Beyond traditional office visits and procedures, modern podiatry and orthopedic foot care often incorporate advanced diagnostic tools like gait analysis and motion labs. These sophisticated technologies provide in-depth insights into a patient’s movement patterns, helping to diagnose complex conditions and tailor treatment plans.
A gait analysis lab typically uses a combination of cutting-edge equipment:
- 3D Motion Capture: Similar to technology used in video games, multiple cameras track reflective markers placed on the body to create a precise 3D model of how a patient walks or moves.
- Force Platforms: Integrated into the floor, these measure the ground reaction forces, revealing how much force is being exerted and absorbed by the foot and ankle during movement.
- Plantar Pressure Mats: These specialized mats capture detailed information about pressure distribution across the sole of the foot, identifying high-pressure areas that could lead to pain or injury.
- Surface Electromyography (EMG): Electrodes placed on the skin measure muscle activation patterns and timing, showing how muscles are working (or not working) during movement.
These tools are invaluable for analyzing tendon injuries, assessing the need for total ankle replacement, diagnosing movement disorders, and even optimizing athletic performance. However, while clinically powerful, billing for these services can be complex. The cost of a full gait analysis can vary significantly, and coverage by insurance providers is not always guaranteed. Patients are often advised to check with their insurance provider regarding coverage for these specific services. For example, some facilities that provide such advanced diagnostics can be found through searches like UCHealth Foot and Ankle Center – Central Park.
Coding for Motion Analysis
Billing for advanced diagnostics like gait analysis and motion labs requires specific CPT codes that reflect the complexity and technology involved. These services are often billed as a series of codes, depending on the components performed:
- CPT 96001: This code is used for “3D computer-based motion capture analysis of gait and/or locomotion, including plantar pressure measurements, dynamic surface electromyography, and/or kinematic analysis; initial 60 minutes.” This code typically covers the comprehensive data collection and initial analysis.
- CPT 96002: For additional time spent on the motion analysis, this code is used: “3D computer-based motion capture analysis of gait and/or locomotion, including plantar pressure measurements, dynamic surface electromyography, and/or kinematic analysis; each additional 30 minutes.”
- CPT 96004: This crucial code covers the “Review and interpretation of comprehensive computer-based motion analysis, with written report.” This reflects the physician’s expertise in analyzing the collected data and translating it into actionable clinical recommendations. It often involves a multidisciplinary team review, which can include physical therapists, biomedical engineers, and orthotists.
While these codes exist, coverage for motion analysis can vary widely among insurance plans. Patients are encouraged to contact their insurance provider directly to confirm coverage details. These services can be instrumental in athletic performance analysis, helping athletes identify biomechanical inefficiencies and reduce injury risk. Ensuring proper documentation to support the medical necessity of these high-tech analyses is paramount for successful reimbursement. For general billing inquiries, including how patients can pay their bills, our Pay Your Foot and Ankle Bill: Quick and Easy Steps page can be a helpful resource.
Optimizing Foot and Ankle Billing Processes to Prevent Denials
Preventing claim denials is a cornerstone of a healthy revenue cycle in foot and ankle billing. Denials lead to delayed payments, increased administrative work, and ultimately, lost revenue. Optimizing your billing processes involves a multi-faceted approach, focusing on accuracy and proactive measures.
Here are key strategies we recommend to minimize denials and streamline your billing:
- Accurate Coding: This is non-negotiable. Ensure that CPT, HCPCS, and ICD-10-CM codes precisely reflect the services rendered and the patient’s diagnosis. This includes using appropriate modifiers like -25, Q7, Q8, Q9, and anatomical modifiers (LT, RT, TA-T9).
- Thorough Documentation: “If it wasn’t documented, it wasn’t done.” Your clinical notes must clearly support the medical necessity of every service. For routine foot care, this means documenting systemic conditions, class findings, and active care requirements. For E/M services, ensure the documentation justifies the level of service billed.
- Claim Scrubbing: Implement a robust pre-submission review process. Claim scrubbing software or expert billers can identify common coding errors, missing information, or payer-specific edits before claims are sent out, catching potential denials before they happen.
- Insurance Verification: Always verify patient eligibility and benefits before services are rendered. This helps identify deductibles, co-pays, co-insurance, and any specific coverage limitations for foot and ankle care.
- Prior Authorization and Referral Management: Many insurance plans, especially HMOs and PPO-POS plans like United Healthcare, require prior authorization for certain procedures or an authorized referral from a Primary Care Provider (PCP). Obtaining these approvals upfront is crucial.
- Timely Filing: Be aware of payer-specific timely filing limits. Submitting claims promptly prevents denials due to expired deadlines.
By implementing these strategies, your practice can significantly reduce the incidence of denials, improve cash flow, and free up staff to focus on patient care. Mastering these processes is key to financial success. For more on streamlining your practice’s finances, explore The Art of the Bill: Streamlining Your Podiatry Practice Finances and avoid common Podiatry Billing Pitfalls: Your Guide to Staying Compliant and Audit-Free.
| Common Denial Reasons | Solutions community of Foot and Ankle Clinic and Podiatry billing.
