Podiatry Practice Billing: Top 3 2026 Secrets
Why Podiatry Practice Billing Demands Specialized Expertise
Podiatry practice billing is one of the most complex specialties in medical billing, requiring precise knowledge of unique codes, modifiers, and payer-specific rules that can make or break your practice’s financial health.
Key Elements of Successful Podiatry Billing:
- Accurate Documentation – Clear SOAP notes demonstrating medical necessity, especially for routine foot care linked to systemic conditions like diabetes
- Specialized Coding – Correct use of CPT codes (11720-11721 for nail debridement, 28285 for hammertoe correction) with appropriate modifiers (Q7-Q9, RT/LT, TA-T9)
- Payer Policy Knowledge – Understanding Medicare’s routine foot care restrictions vs. commercial insurance requirements
- Clean Claims Process – Insurance verification, claim scrubbing, and timely submission to minimize denials
- Effective Denial Management – Quick appeal turnaround and systematic follow-up to reduce days in accounts receivable
Podiatry practices face unique revenue cycle challenges, mixing medical and surgical services where the line between “routine” and “medically necessary” care determines payment. With little billing training, physicians can easily see claims denied for a single missing modifier. While benchmark billing costs are 6-8% of gross income, the complexities of podiatry often push this figure higher.
The stakes are high. Denials cause delayed payments and administrative burdens. Medicare restricts routine foot care reimbursement without documented systemic conditions and Q-modifiers. Commercial payers and workers’ comp cases add further complexity with unique bundling edits and prior authorization rules.
This guide will walk you through the essential elements of podiatry practice billing—from understanding how systemic conditions impact coverage to mastering the critical codes and modifiers, building an efficient workflow, and deciding whether to keep billing in-house or partner with specialists who live and breathe podiatry billing every day.
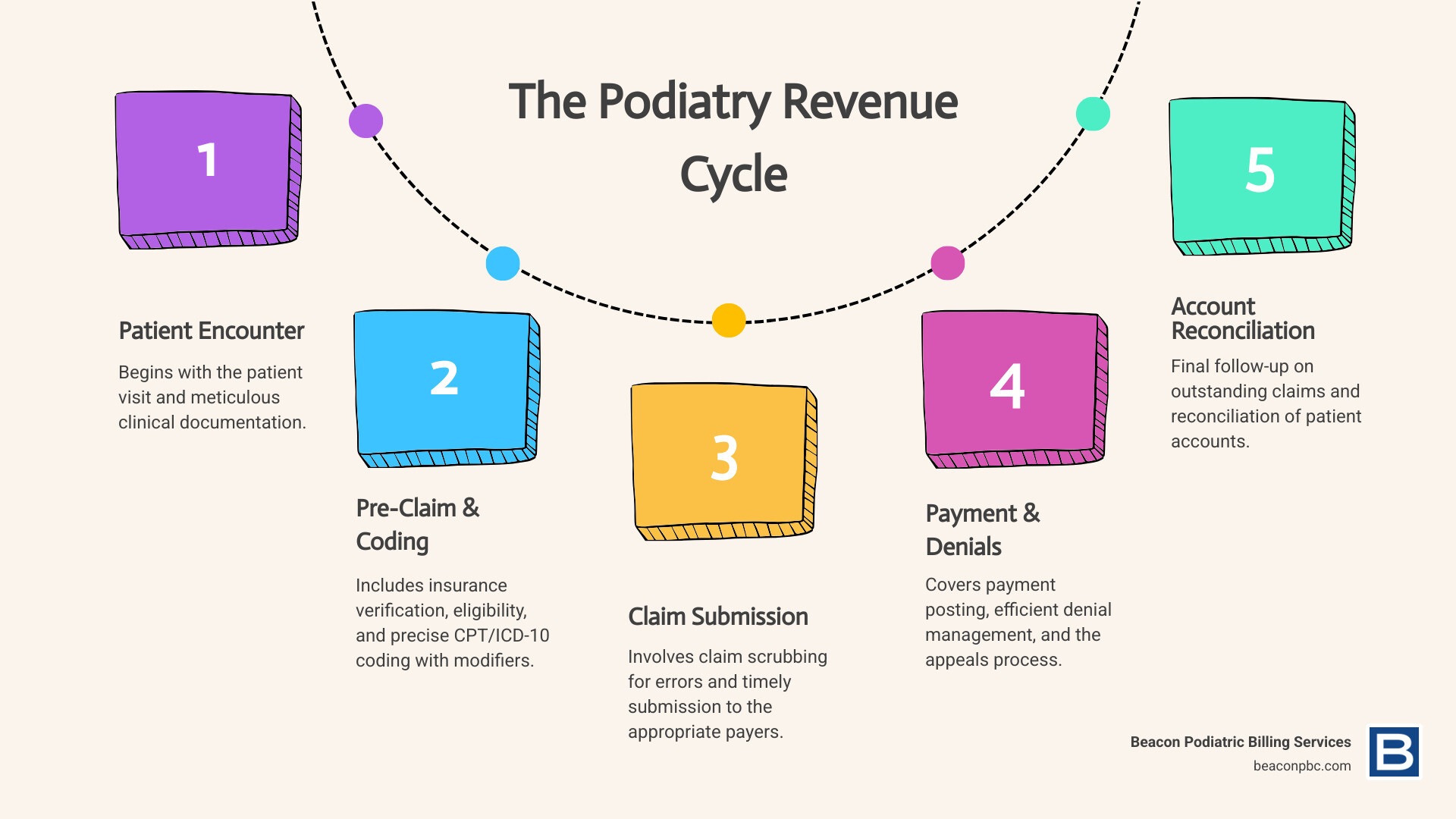
The Unique Challenges of Podiatry Billing
Podiatry billing is intricate, unlike general medical billing. It often involves a gray area between routine care and medically necessary intervention, a distinction that directly impacts reimbursement.
The podiatry billing process encounters certain challenges that affect financial stability, including complex coding, varied insurance coverage, documentation issues, and the threat of denials. Practices also must steer a constantly changing regulatory environment and the demands of integrating efficient technology.

A primary hurdle is “routine foot care.” Payers, especially Medicare, often view services like nail trimming as non-covered unless a systemic condition justifies medical necessity. Without this justification or required prior authorizations for orthotics, claims are frequently denied, causing lost revenue and administrative headaches.
The Impact of Systemic Conditions on Coverage
Systemic conditions like diabetes, peripheral vascular disease (PVD), and peripheral neuropathy profoundly impact coverage for podiatry practice billing. Medicare, for example, won’t cover routine foot care unless a patient has a qualifying systemic condition that puts them at high risk.
To justify coverage for these patients, accurate documentation of “class findings” is critical. These findings categorize the condition’s severity and the risks involved. For example:
- Class A: Indicates a non-traumatic amputation or significant findings, such as severe claudication or gangrene.
- Class B: Involves conditions like swelling, poor circulation, or temperature abnormalities.
- Class C: May include onychomycosis, fungal infections, or thickened nails.
Without clear documentation linking the systemic condition to the service’s medical necessity (e.g., preventing ulcers or amputations), claims will be denied. You need to demonstrate that the service prevents further complications, which is a key aspect of medical necessity. For a deeper dive into these guidelines, you can find more info about Medicare Podiatry Billing Guidelines on the Guide Podiatric Billing Services website.
Navigating Medicare vs. Commercial Payer Policies
Navigating policy differences between Medicare and commercial payers is another major challenge in podiatry practice billing. While Medicare has stringent rules, commercial insurers have their own unique and complex requirements.
- Medicare Guidelines: Medicare requires a qualifying systemic condition, specific class findings, and correct Q-modifiers for routine foot care. It also imposes frequency limits (e.g., every 60 days) and requires the patient to have seen their managing physician within the last six months.
- Commercial Insurance Rules: Commercial payers vary widely. Some are less restrictive than Medicare, while others demand more detail. Prior authorizations are more common for custom orthotics, injections, or surgery. Many denials stem from common denial reasons in podiatry such as missing authorizations or incorrect modifier use. Each payer may have different bundling edits, complicating billing for multiple procedures.
Understanding and carefully tracking these variations is crucial for maximizing reimbursement and minimizing denials across all your patient demographics in New Jersey, Nevada, Nebraska, North Carolina, and Kentucky.
Mastering Podiatry Codes & Modifiers for Maximum Reimbursement
In podiatry practice billing, correct codes and modifiers are essential for communicating medical necessity to payers. Podiatric coding is a constantly changing field, so staying current on CPT, ICD-10, and HCPCS changes is vital for accurate reimbursement. You can always check more info about Billing & Coding Updates on the Guide Podiatric Billing Services site for the latest changes.
Essential CPT and ICD-10 Codes
Accurate coding involves selecting the right Current Procedural Terminology (CPT) codes for procedures and International Classification of Diseases, Tenth Revision (ICD-10) codes for diagnoses. Here’s a look at some commonly used codes in podiatry:
Common CPT Codes in Podiatry:
- Evaluation and Management (E/M) Services:
- New Patient Visits: 99202–99205 (by complexity)
- Established Patient Visits: 99212–99215 (by complexity)
- Nail Care Procedures:
- 11720: Debridement; one to five nails
- 11721: Debridement; six or more nails
- 11730: Avulsion of nail plate, partial or complete, simple; single
- Skin Procedures:
- 11055: Paring of corn/callus; single lesion
- 11056: Paring of corn/callus; two to four lesions
- 11057: Paring of corn/callus; more than four lesions
- Injections:
- 20550: Injection; tendon sheath, ligament (e.g., plantar fascia)
- 20610: Arthrocentesis, aspiration and/or injection; major joint or bursa (e.g., ankle, knee)
- 64450: Injection, anesthetic agent; plantar digital nerve
- Surgical Procedures:
- 28285: Correction, hammertoe (e.g., interphalangeal fusion, partial or total phalangectomy)
- 28296: Correction, hallux valgus (bunion); w/ distal metatarsal osteotomy
- Orthotics and Prosthetics:
- L3020: Foot insert, molded to patient model, “sport”
- Wound Care:
- 11042-11047: Debridement codes for various depths and sizes of wounds.
- 97597-97598: Debridement (e.g., waterjet, sharp selective)
Common ICD-10 Codes in Podiatry:
- E11.621: Type 2 diabetes mellitus with foot ulcer
- L84: Corns and callosities
- M79.671: Pain in the left foot (laterality is crucial!)
- M77.31: Plantar fasciitis, right foot
- L60.0: Ingrowing nail
Linking each procedure to a qualifying diagnosis is vital. Billing CPT 11721 for nail debridement without an ICD-10 code for a systemic condition like diabetes (E11.621) will likely be denied.
Critical Modifiers and When to Use Them
Modifiers provide essential context to CPT codes, and correct usage is key to preventing denials in podiatry practice billing.
- Q Modifiers (Q7, Q8, Q9): Critical for routine foot care under Medicare.
- Q7: Used for one Class A finding (e.g., a non-traumatic amputation).
- Q8: Used for two Class B findings (e.g., absent pulses, edema). Used with CPT 11721 for systemic conditions.
- Q9: Used for one Class B finding and two Class C findings (e.g., onychomycosis, thickened nails).
- Laterality Modifiers (RT, LT): Indicate which side of the body a procedure was performed on (Right, Left). Always use these for unilateral procedures.
- Toe Modifiers (TA-T9): Specify which toe a procedure was performed on (e.g., TA for left foot, first digit). Note: Not used for CPT codes 97598, 11720, and 11721.
- Modifier 59 (Distinct Procedural Service): Indicates a procedure was distinct from other services on the same day. Example: Used when removing a callus (11055) and a wart (17110) in different locations during the same visit.
- Modifier 25 (Significant, Separately Identifiable Evaluation and Management Service): Applied to an E/M service when a significant, separately identifiable E/M service is performed on the same day as a procedure.
Incorrect modifier use is a top reason for denials. Mastering their context is as important as knowing the codes themselves. For a comprehensive resource on this, check out Podiatry Billing Made Easy: Your Ultimate Cheat Sheet for CPT Modifiers and Diagnosis Codes.
Building a Bulletproof Podiatry Practice Billing Workflow
An effective podiatry practice billing workflow is the backbone of a financially healthy practice. This continuous cycle, from registration to final payment, minimizes errors, speeds up reimbursement, and lets your team focus on patient care. For more insights into optimizing your operations, explore more info about Practice Management & Growth.
From Patient Check-In to Clean Claim Submission
Every step in the patient journey presents an opportunity to ensure a clean claim.
- Patient Registration & Eligibility Verification: Collect complete demographic and insurance data. Verify insurance for every visit, as policies change. Use automated systems to check eligibility at scheduling and before the appointment to identify issues proactively.
- Accurate Clinical Documentation (SOAP Notes): The medical record must clearly demonstrate medical necessity. Detail the chief complaint, exam findings (including class findings), diagnosis, and treatment plan. For routine nail care, document the systemic condition (e.g., diabetes) and associated findings (e.g., neuropathy) that justify the service.
- Code Selection & Modifier Application: Based on documentation, select the correct CPT and ICD-10 codes. Apply all necessary modifiers (Q, RT/LT, T, 25, 59) to give the payer the full context.
- Claim Scrubbing & Submission: Use billing software with claim scrubbing tools to catch common errors like missing modifiers or incorrect code linkages before submission. This pre-submission audit prevents many initial denials. Submit claims electronically via a clearinghouse.
Integrating technology like EHRs and billing software is paramount to streamline documentation and improve coding accuracy.
Effective Denial Management and A/R Follow-Up
Even with the best workflow, denials happen. How you manage them is key to the financial health of your podiatry practice billing.
- Denial Reason Analysis: When a claim is denied, understand why. Log the denial, identify the reason code, and track patterns. Common reasons include lack of medical necessity, incorrect modifiers, or missing prior authorization.
- Prompt Action & Appeal Process: Act immediately on denials, as payers have strict appeal deadlines. Correct errors, gather supporting documents, and resubmit or file a formal appeal.
- Timely Follow-Up: Establish a systematic process to follow up on all submitted claims and appeals. Use Electronic Remittance Advice (ERA) to monitor claim status.
- Reducing Days in A/R: The goal is to reduce the time money is tied up in accounts receivable. A high clean claims rate and efficient denial management directly improve cash flow. For further strategies, see more info about Financial Health & KPIs.
A proactive approach to denial management, coupled with continuous staff training and process refinement, transforms denials from revenue black holes into learning opportunities that strengthen your entire billing operation.
The Financial Stakes: In-House vs. Outsourced Podiatry Practice Billing
Every podiatry practice must decide whether to manage billing in-house or outsource to a specialist. This choice significantly impacts staffing costs, revenue, and compliance, as inaccurate podiatry practice billing leads to denials, audit risks, and lost revenue.
| Feature | In-House Podiatry Billing | Outsourced Podiatry Billing |
|---|---|---|
| Cost | High fixed costs (salary, benefits, training, software, office space); Variable costs (postage, clearinghouse fees); Potential for hidden costs (denial rework, lost revenue from errors); Benchmark 6-8% of gross income, often higher due to complexity. | Typically a percentage of collections (e.g., 5-10%); Predictable variable cost; No employee overhead (benefits, training); Access to advanced software without direct purchase; Cost-efficiency often higher due to economies of scale and expertise. |
| Expertise | Requires continuous training for staff on evolving codes and payer rules; Risk of single point of failure if one employee handles all billing; Expertise may be broad rather than deep in podiatry. | Access to dedicated, podiatry-specific billing experts; Up-to-date knowledge of all codes, modifiers, and payer policies; Team of billers ensures continuity and redundancy. |
| Efficiency | Can be efficient with highly trained staff and robust systems; Prone to slowdowns due to staff illness, turnover, or lack of specialized tools; Time spent on billing takes away from patient care. | Streamlined processes; Faster claims submission and follow-up due to specialized workflows and technology; Reduced administrative burden on practice staff, allowing more focus on patient care. |
| Compliance | Requires meticulous internal auditing and adherence to constantly changing regulations (HIPAA, CMS, payer-specific); High risk of non-compliance if staff are not regularly trained or updated. | Specialized services are inherently focused on compliance and stay current with all regulations; Reduces practice’s compliance burden; Built-in checks and balances to minimize audit risk. |
| Control | Direct control over all billing processes and staff; Immediate access to billing data and reports. | Less direct day-to-day control, but reliable services offer transparent reporting and communication; Regular reporting keeps you informed; Frees up practice management to focus on higher-level strategic decisions. |
| Risk | High risk of embezzlement, staff turnover, burnout, and costly errors leading to denials and audits. | Reduces risks associated with in-house staffing (embezzlement, turnover); Transfers billing-related compliance and operational risks to the billing service; Improves security of patient data and financial information. |
The True Cost of In-House Billing
Many practices underestimate the true cost of managing podiatry practice billing internally, which extends beyond salary:
- Biller Salary & Benefits: An experienced podiatry biller requires a competitive salary plus benefits (health insurance, retirement, PTO), which can add 30% to the base cost.
- Training Costs: Staff require continuous training on changing codes and payer policies, incurring costs for courses and time away from the office.
- Software Expenses: Costs include billing software, EHR systems, clearinghouse fees, and necessary updates.
- Staff Turnover Risk: The departure of a key billing employee can disrupt your revenue cycle, as training a replacement is time-consuming and costly.
- Embezzlement Risk: Concentrating billing and collections duties in one person creates a vulnerability that requires robust internal controls to mitigate.
- Lost Revenue: This is the biggest hidden cost. Inaccurate coding, missed appeals, and poor follow-up directly reduce income. A low clean claims rate is a sign your in-house billing is underperforming.
How to Choose a Specialized Podiatry Practice Billing Partner
When outsourcing podiatry practice billing, choosing the right partner is critical. Look for deep podiatry expertise, not just the lowest price. Ask these key questions:
- Podiatry Expertise: Do they specialize in podiatry? Is their staff trained on podiatry-specific codes (Q-codes, T-modifiers) and routine foot care policies?
- Reporting Capabilities: What key performance reports do they provide (e.g., clean claim rate, days in A/R)? Is reporting transparent and easy to understand?
- Fee Structure: What is their fee model (e.g., percentage of collections)? Are there hidden costs or start-up charges?
- US-Based Team: Is their team 100% US-based to ensure clear communication and regulatory understanding?
- Credentialing Services: Do they handle the complex and time-consuming provider credentialing process?
- Workflow & Turnaround: What is their claim submission turnaround time and process for information transfer?
- Denial Management: What is their process and success rate for appealing denials?
- Data Security: How do they ensure HIPAA compliance and data security?
- Money Handling: Do they ensure all payments go directly to your practice’s bank account, not to the billing service?
- Client Support: Will you have a dedicated point of contact and what is their response time?
- Contract Terms: What is the contract length? An initial one-year term is advisable.
By asking these detailed questions, you can make an informed decision that truly benefits your podiatry practice billing. For more resources, check out more info about our Articles.
Frequently Asked Questions about Podiatry Billing
What are the most common reasons for podiatry claim denials?
The most common reasons for podiatry practice billing claim denials include:
- Lack of Medical Necessity: Documentation fails to prove a service was necessary, especially for routine foot care linked to systemic conditions.
- Incorrect Modifier Usage: Forgetting or misusing crucial modifiers like Q-codes, laterality (RT/LT), Modifier 59, or Modifier 25.
- Missing Prior Authorization: Failing to get pre-approval for surgeries, custom orthotics, or certain other procedures.
- Routine Care Exclusions: Billing for routine foot care for patients without a qualifying systemic condition documented per payer rules.
- Inadequate Documentation of Class Findings: Failing to clearly document the specific Class A, B, or C findings that justify care for a patient with a systemic condition.
How much do podiatry billing companies charge?
Podiatry billing service fees typically range from 5% to 10% of monthly collections, though some rates can be as low as 3% to 6%. This percentage-based model aligns the billing service’s success with yours. The exact fee depends on:
- Practice Size and Volume: Larger practices may secure lower rates.
- Services Included: The fee may or may not include services like credentialing or practice management consulting.
- Complexity: High-volume surgical or workers’ comp practices may see higher rates due to increased complexity.
- Geography: Regional operating costs can sometimes influence pricing.
When evaluating price, consider the total cost versus the potential increase in collections and reduced administrative burden.
Does Medicare cover routine foot care?
The answer is generally no, unless specific conditions are met.
Medicare considers routine foot care (e.g., nail trimming, callus removal) non-covered. However, Medicare will cover these services if a patient has a qualifying systemic condition that puts them at high risk. Common qualifying conditions include:
- Diabetes Mellitus (DM)
- Peripheral Vascular Disease (PVD)
- Peripheral Neuropathy
To ensure coverage, you must carefully document two critical elements:
- A Qualifying Systemic Condition: The patient must have a qualifying diagnosis.
- Class Findings: The podiatrist must document specific Class A, B, or C findings that prove the medical necessity of the care to prevent complications.
Additionally, the claim must include the correct Q-modifier (Q7, Q8, Q9) to indicate the findings. Without it, the claim will be denied. The patient’s managing physician must also have seen them within the last six months.
So, while Medicare generally doesn’t cover “routine” foot care, it does cover medically necessary foot care for at-risk patients, provided all documentation and coding requirements are met.
Conclusion
Navigating podiatry practice billing is complex. It requires specialized knowledge of routine foot care rules, systemic conditions, and an ever-changing landscape of codes and modifiers. An effective workflow with accurate documentation and proactive denial management is essential for your practice’s financial health.
The choice between in-house and outsourced billing is pivotal. While in-house offers control, it carries hidden costs and risks. Outsourcing to a specialized, 100% US-based partner with deep podiatry expertise can streamline finances, reduce administrative burdens, and maximize collections. This allows your team to focus on patient care in New Jersey, Nevada, Nebraska, North Carolina, and Kentucky.
By partnering with a dedicated expert like Guide Podiatric Billing Services, you can steer these complexities, maximize your revenue, and ensure your practice’s financial health. Learn more about our specialized podiatry billing services.
