Podiatry CPT Codes 2026: Essential Billing Guide
Why Accurate Coding is the Lifeblood of Your Practice
Podiatry CPT codes are standardized numerical codes that describe medical procedures and services provided by podiatrists, essential for submitting claims to insurance companies and receiving proper reimbursement. Understanding and correctly applying these codes directly impacts your practice’s financial health.
Quick Reference: Essential Podiatry CPT Code Categories
| Service Type | Common CPT Codes | Example |
|---|---|---|
| Office Visits | 99202-99205, 99212-99215 | New or established patient E/M |
| Nail Care | 11720, 11721, 11730 | Debridement, avulsion |
| Skin Procedures | 11055-11057 | Callus removal |
| Injections | 20550, 20605 | Tendon sheath, joint |
| Surgery | 28285, 28292, 28297 | Hammertoe, bunion repair |
| Wound Care | 97597 | Debridement |
| Orthotics | L3020, L3030 | Custom foot orthotics |
The U.S. podiatry services market is projected to reach $5.1 billion by 2030, yet Medicare’s improper payment rate for podiatry care is 11.2%, translating to $216.9 million in projected improper payments. Insufficient documentation is the main culprit, accounting for 76.4% of these errors. Accurate coding isn’t just paperwork; it’s the difference between getting paid and watching revenue slip away.
Every day, podiatrists face a growing patient population driven by aging demographics, obesity rates, and the diabetes epidemic affecting over 38 million Americans. Between 15-34% of diabetic patients will develop a foot ulcer in their lifetime, and 15-20% of those ulcers may lead to amputation without proper treatment. Your clinical expertise saves limbs and lives—but coding errors can cripple your practice financially.
The challenge isn’t just knowing which code to use. It’s understanding when Medicare requires specific Q-modifiers for routine care, how to properly document medical necessity for nail debridement, and why missing a simple modifier -25 can cause your E/M service to be bundled and denied.
Practices with quarterly internal audits see 17% fewer denials compared to those auditing annually—a clear strategic advantage.
This guide walks you through the essential CPT and ICD-10 codes every podiatrist needs to know, the Medicare rules that trip up most practices, and the practical strategies that maximize your reimbursement while minimizing denials.
The Foundation: Understanding Podiatry Billing Codes and Guidelines
Podiatry medical billing relies on three core coding systems: CPT, ICD-10, and HCPCS. Each plays a distinct yet interconnected role in translating the care you provide into billable services.
CPT (Current Procedural Terminology) codes are what we’re primarily focusing on—these are the five-digit numerical codes that describe the actual services you perform, such as an office visit, a nail debridement, or a bunionectomy. They tell the payer what you did.
ICD-10 (International Classification of Diseases, 10th Revision, Clinical Modification) codes, on the other hand, are alphanumeric codes that describe the patient’s diagnosis or medical condition. They tell the payer why you did it. For example, a patient might present with plantar fasciitis (M72.2), and you perform an injection (a CPT code). Without the “why,” the “what” won’t get paid.
HCPCS (Healthcare Common Procedure Coding System) Level II codes are alphanumeric codes primarily used for products, supplies, and services not covered by CPT codes, such as durable medical equipment, orthotics, and some medications. These codes often start with a letter (e.g., L3020 for a custom foot orthotic).
These codes are the language you use to communicate with payers. Imprecise or non-compliant coding leads to denied claims and lost revenue. This is where the concept of medical necessity becomes paramount. Every service billed must be medically necessary, meaning it’s appropriate and consistent with the diagnosis and the patient’s symptoms.
Documentation is the bedrock of medical necessity. Your patient’s medical record, particularly your SOAP (Subjective, Objective, Assessment, Plan) notes, is the story that justifies every code you bill. Insufficient documentation is a colossal problem in podiatry, accounting for a staggering 76.4% of improper payments. If it’s not documented, it didn’t happen in the eyes of the payer. Accurate, thorough, and legible documentation is your first line of defense against denials.
Podiatry billing differs significantly from general medical billing. It has unique rules for routine foot care, modifiers, and systemic conditions that justify coverage. It requires a nuanced understanding of foot and ankle pathology and specific payer guidelines (especially Medicare). Services like custom orthotics or certain nail procedures have distinct coding and authorization requirements not found in general practice.
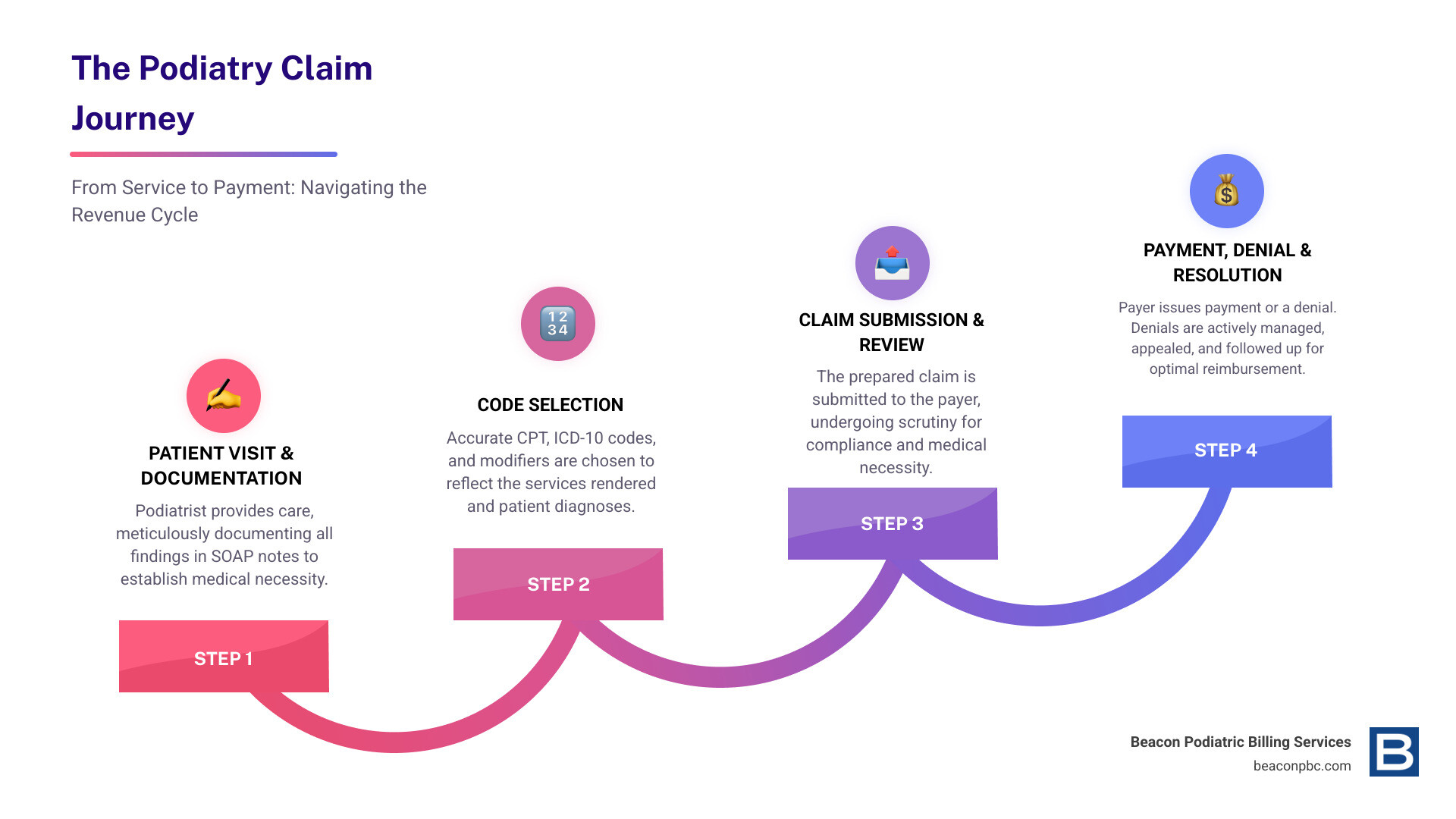
The journey of a claim, from patient visit to payment, involves several critical steps: insurance verification, meticulous code selection, claim submission, and denial management. It’s a cycle that demands precision at every turn.

The Typical Podiatry Billing Workflow
Let’s walk through a typical day in the life of a podiatry claim, highlighting the crucial steps that ensure smooth sailing through the revenue cycle:
-
Step 1: Patient Eligibility Verification: Before the patient’s visit, verify their insurance coverage and eligibility. Confirm benefits, copays, deductibles, and any prior authorization requirements for planned services. This proactive step prevents payment issues for both the patient and your practice.
-
Step 2: Clinical Documentation: Your SOAP notes must be comprehensive, detailed, and clearly support the medical necessity of every service. Include relevant comorbidities, physical findings, and a clear treatment plan. If it’s not documented, it’s not reimbursable.
-
Step 3: Code Selection: Here’s where the CPT, ICD-10, and HCPCS codes come into play. We carefully select the most accurate codes that reflect the services rendered and the patient’s diagnosis. This includes choosing the correct level of E/M service, identifying specific procedure codes (like podiatry CPT codes 11720 for nail debridement or 28285 for hammertoe repair), and linking them to the most specific ICD-10 diagnosis codes, paying close attention to laterality (left vs. right).
-
Step 4: Claim Scrubbing & Submission: Before submission, claims undergo a rigorous “scrubbing” process to check for errors, inconsistencies, and compliance with payer-specific rules and NCCI (National Correct Coding Initiative) edits. Claims are then submitted electronically via a clearinghouse or direct payer portal.
-
Step 5: Payment Posting: Once payers process the claims, we receive an Explanation of Benefits (EOB) or Electronic Remittance Advice (ERA) detailing the payment, any adjustments, or denials. We carefully post these payments to the patient accounts, ensuring accurate financial records.
-
Step 6: Denial Management & Follow-up: Denials require active management. Identify the reasons, correct errors, and appeal when appropriate. A robust denial management strategy is crucial, as even a small percentage of unaddressed denials significantly impacts your bottom line. Proactive management, such as regular audits, is key to reducing denial rates.
Cracking the Codes: A Guide to Common Podiatry CPT Codes
Let’s explore the most frequently used podiatry CPT codes. This section highlights common codes across various services. For a complete list and current guidelines, always consult the official American Podiatric Medical Association (APMA) CPT Coding Guide.
Evaluation and Management (E/M) Services
These codes are for the bread and butter of your practice—the patient visits where you evaluate, diagnose, and manage conditions. E/M codes are selected based on either the total time spent with the patient (on the date of the encounter) or the complexity of Medical Decision Making (MDM).
- New Patient Codes:
- 99202: Straightforward MDM, 15-29 minutes
- 99203: Low MDM, 30-44 minutes
- 99204: Moderate MDM, 45-59 minutes
- 99205: High MDM, 60-74 minutes
- Established Patient Codes:
- 99212: Straightforward MDM, 10-19 minutes
- 99213: Low MDM, 20-29 minutes
- 99214: Moderate MDM, 30-39 minutes
- 99215: High MDM, 40-54 minutes
In podiatry, where we often manage complex conditions like diabetic foot ulcers or surgical referrals, the MDM often drives higher-level codes. Just be sure your documentation clearly supports the chosen level.
Key podiatry CPT codes for Routine Foot Care and Nail Procedures
Routine foot care is where many podiatry practices encounter billing complexities, especially with Medicare. Accurate coding and robust documentation of medical necessity are paramount.
- Nail Debridement: These codes are for the trimming, cutting, or debridement of nails.
- 11720: Debridement of 1-5 nails.
- 11721: Debridement of 6 or more nails.
- Crucial Insight: These are frequently scrutinized by payers. Medical necessity, often linked to systemic conditions (like diabetes or peripheral vascular disease) or painful mycotic nails, must be explicitly documented.
- Callus Removal:
- 11055: Paring or cutting of a single hyperkeratotic lesion (e.g., callus or corn).
- 11056: Paring or cutting of 2-4 hyperkeratotic lesions.
- 11057: Paring or cutting of more than 4 hyperkeratotic lesions.
- Best Practice: Always link these to a qualifying diagnosis, especially for Medicare patients, to justify the service.
- Nail Avulsion: This is for the removal of a nail plate.
- 11730: Avulsion of nail plate, partial or complete, simple; single.
- 11732: Each additional nail plate (List separately in addition to code for primary procedure).
- Documentation Tip: Always specify the toe and side (e.g., left great toe) using appropriate modifiers.
- Nail Biopsy:
- 11755: Biopsy of nail unit (e.g., plate, bed, matrix, hyponychium).
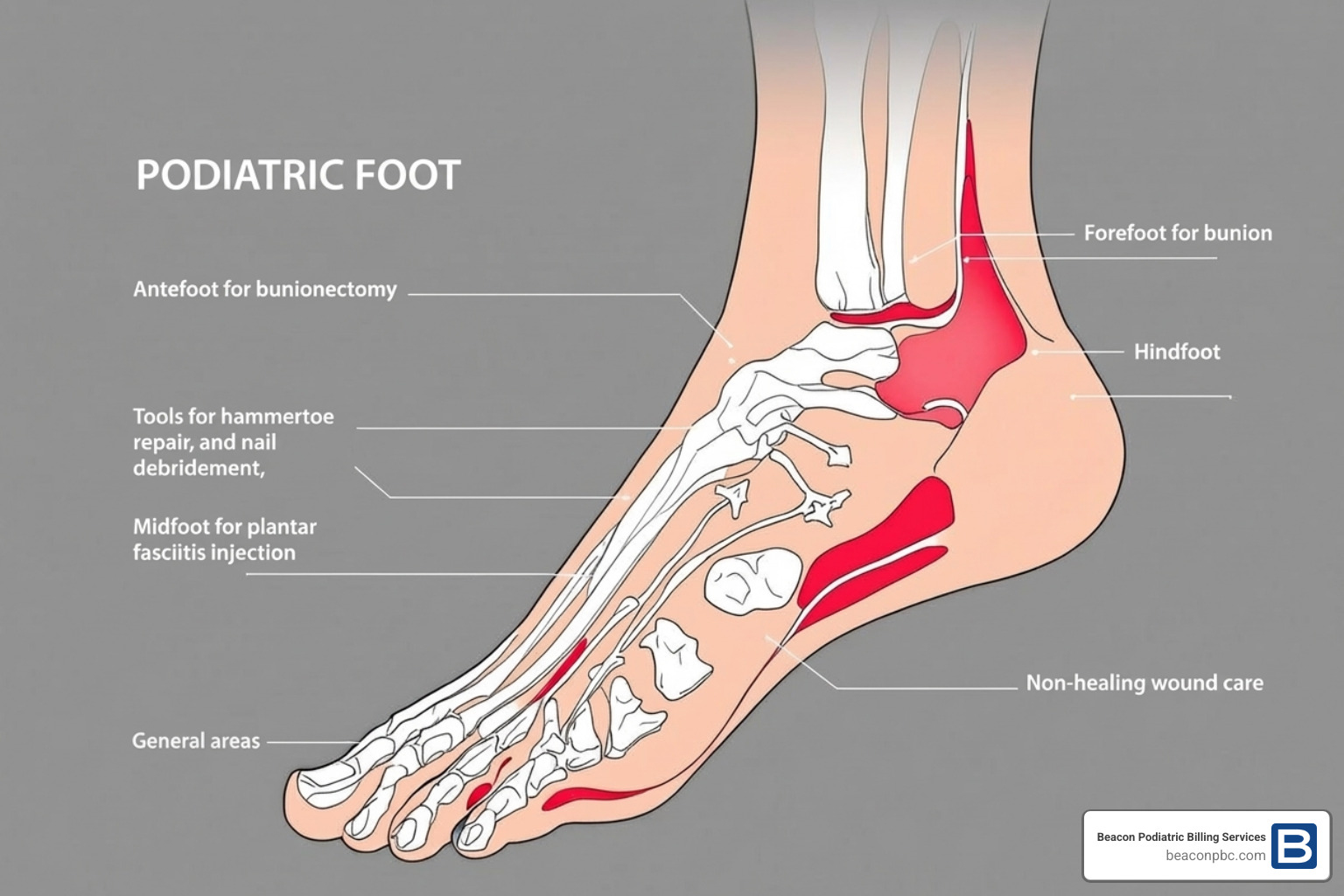
Essential podiatry CPT codes for Surgical, Injection, and Wound Care Procedures
Podiatrists perform a wide range of procedures, from minor in-office interventions to complex surgeries. Here are some key codes:
- Bunionectomy (Hallux Valgus Correction):
- 28292: Correction, hallux valgus (bunion), with sesamoidectomy, when performed; with proximal metatarsal osteotomy, any method.
- 28297: Correction, hallux valgus (bunion), with sesamoidectomy, when performed; with distal metatarsal osteotomy, any method.
- Surgical Insight: Operative notes must be incredibly detailed, describing the specific surgical approach, any implants used, and pre- and post-operative diagnoses.
- Hammertoe Repair:
- 28285: Correction, hammertoe (e.g., interphalangeal fusion, partial or total phalangectomy).
- Documentation Tip: Clearly state which toe(s) are being corrected.
- Injections:
- 20550: Injection(s); tendon sheath, or ligament, aponeurosis (e.g., plantar “fascia”). Common for plantar fasciitis.
- 20605: Arthrocentesis, aspiration and/or injection; intermediate joint or bursa (e.g., ankle, elbow, wrist, or temporomandibular joint). For smaller joints in the foot, such as the metatarsophalangeal joint.
- Coding Alert: Payers often bundle injections with office visits. If you perform a significant, separately identifiable E/M service on the same day as an injection, use modifier -25 on the E/M code to ensure both are reimbursed.
- Wound Debridement:
- 97597: Debridement (e.g., high pressure waterjet with/without suction, sharp selective debridement with scissors, scalpel and forceps) open wound, (e.g., full thickness skin, subcutaneous tissue, muscle, or bone), including topical application(s), wound assessment, use of a whirlpool, when performed and instruction(s) for ongoing care, per session, total wound(s) surface area; first 20 sq cm or less.
- Important Note: This code is for active wound care management. Other debridement codes exist (e.g., 11042-11047) for deeper debridement of skin, subcutaneous tissue, muscle, and bone.
Navigating Payer Nuances: Medicare, Modifiers, and Systemic Conditions
Medicare, a primary payer for many podiatry patients, has a labyrinth of specific rules for routine foot care. Understanding these nuances, plus the role of modifiers and “Class Findings,” is key to proper reimbursement. For more in-depth information, we always refer our clients to Medicare Podiatry Billing Guidelines.
Medicare generally considers “routine foot care” (like cutting corns/calluses and trimming nails) to be non-covered. Why? Because historically, these were seen as hygiene services. However, there are significant exceptions! Services become medically necessary and thus covered when they are:
- An integral part of another covered service (e.g., treating an ulcer).
- For the treatment of warts.
- When a systemic condition (like diabetes, peripheral vascular disease, or certain neuropathies) results in severe circulatory discomfort or reduced sensation, posing a hazard if performed by a non-professional.
This is where systemic conditions like diabetes, arthritis, and peripheral vascular disease (PVD) become critical. These conditions often lead to foot complications that necessitate professional podiatric care to prevent more severe outcomes like ulcers or amputations. For patients with these underlying diseases, routine foot care can be covered if properly documented. Diabetes alone affects over 38 million Americans, and the associated foot complications underscore the medical necessity of your services.
The Crucial Role of Modifiers in Podiatry Billing
Modifiers are two-character codes added to CPT or HCPCS codes to provide additional information about a service, clarifying the circumstances under which it was performed.
- Modifier -25 (Significant, Separately Identifiable E/M Service): This is perhaps one of the most frequently used—and often misused—modifiers in podiatry. We use it when a significant, separately identifiable E/M service (like a new patient exam) is performed on the same day as a minor procedure (like an injection or nail avulsion). Without -25 on the E/M code, the payer might bundle the E/M service into the procedure, resulting in no reimbursement for your evaluation time.
- Modifier -59 (Distinct Procedural Service): When two or more procedures that would normally be bundled are performed on the same day, but are distinct and separate (e.g., at different anatomical sites, or for different diagnoses), modifier -59 is your best friend. For example, if you remove a callus (11055) from the right foot and a wart (17110) from the left foot during the same visit, -59 would be appended to one of the procedure codes to indicate they are distinct.
- Q Modifiers (Q7, Q8, Q9): These are specific to Medicare and are used for routine foot care to indicate the presence of qualifying systemic conditions that justify coverage.
- Q7: One Class A finding (e.g., nontraumatic amputation of the foot).
- Q8: Two Class B findings (e.g., absent posterior tibial pulse, advanced trophic changes).
- Q9: One Class B and two Class C findings (e.g., claudication, temperature changes).
- These modifiers are absolutely essential for getting routine foot care claims paid by Medicare when medical necessity is established.
- Laterality Modifiers (LT, RT): These indicate whether a procedure was performed on the left (LT) or right (RT) side of the body. For bilateral procedures, some payers prefer using modifier -50, while others may require LT and RT on separate lines. Always check payer-specific guidelines.
- Toe Modifiers (TA-T9): These are used to specify which toe a procedure was performed on (e.g., TA for left foot, great toe; T1 for left foot, second toe; up to T9 for right foot, fifth toe). These are particularly useful for procedures like hammertoe repair or nail avulsions.
“Class Findings” and Systemic Conditions: Justifying Medical Necessity
The concept of “Class Findings” is Medicare’s way of standardizing the documentation of the severity and necessity of podiatric care, especially for routine foot care. These findings help establish a “presumption of coverage” for patients with severe peripheral involvement due to systemic conditions.
- Class A Findings: These indicate non-traumatic amputation of the foot, which immediately establishes medical necessity for routine foot care.
- Class B Findings: Requires three of the following: absent posterior tibial pulse, absent dorsalis pedis pulse, advanced trophic changes (e.g., hair loss, thinning of skin, brittle nails), edema, or paresthesia.
- Class C Findings: Requires two of the following: claudication, temperature changes, edema, paresthesia, or burning.
To justify coverage, a patient would typically need one Class A finding, or two Class B findings, or one Class B and two Class C findings. This detailed level of clinical documentation is paramount. Furthermore, for these systemic conditions, the patient must be under the active care of a Doctor of Medicine or Osteopathy who has documented the condition within a certain timeframe (often six months).
The Centers for Medicare & Medicaid Services (CMS) provides extensive guidance, such as the CMS article on “Billing and Coding: Foot Care”. This resource details ICD-10-CM code groups that support medical necessity. Linking the diagnosis (ICD-10) to the procedure (CPT) is the backbone of proper reimbursement; without it, claims may be denied.
Preventing Denials and Maximizing Reimbursement
Denials are a major threat to a healthy revenue cycle, representing lost time and revenue. In podiatry, where the improper payment rate is 11.2% (projected to be $216.9 million!), preventing denials is not just a best practice—it’s a survival strategy.
What are the most common reasons claims get rejected or denied in podiatry billing? Our research shows that insufficient documentation leads the pack, accounting for a whopping 76.4% of improper payments. This means the story you’re telling the payer isn’t complete or clear enough to justify the service. Other culprits include:
- Incorrect coding: Using the wrong podiatry CPT codes, ICD-10 codes, or HCPCS codes. This also includes issues like mutually exclusive code pairings (where two codes can’t be billed together) or missing laterality.
- No documentation: This is even worse than insufficient documentation; it means there’s no record at all to support the service.
- Medical necessity issues: The payer doesn’t agree that the service was necessary for the diagnosis provided. This often ties back to documentation.
- Prior authorization failures: Performing a service that required pre-approval from the insurance company, but not obtaining it beforehand. Many podiatric services, especially custom orthotics or complex surgeries, require this.
So, how can we turn the tide and maximize reimbursement? Here are our best practices:
- Impeccable Documentation: Every service, every diagnosis, every patient interaction must be clearly and thoroughly documented. This includes detailed SOAP notes, supporting medical necessity, and justifying the level of service.
- Accurate and Up-to-Date Coding Knowledge: The world of coding is constantly evolving. We encourage continuous education and staying current with the latest coding updates for the podiatry specialty.
- Proactive Insurance Verification and Authorization: Verify eligibility, benefits, and obtain all necessary prior authorizations before the patient’s visit. This catches potential issues early.
- Rigorous Claim Scrubbing: Implement a robust internal process (or partner with experts like us!) to review claims for errors before submission. This pre-submission audit can catch a significant percentage of common errors.
- Effective Denial Management: Log each denial, understand the reason, correct the error, and resubmit or appeal promptly. A well-structured denial management process is critical for recovering lost revenue.
- Regular Internal Audits: This is a game-changer. An MGMA report showed that practices conducting quarterly internal audits saw 17% fewer denials compared to those auditing annually. Regular audits identify error patterns, create training opportunities, and ensure compliance. Staying current with Billing & Coding Updates is also crucial.
Frequently Asked Questions about Podiatry Coding
We encounter many questions about podiatry CPT codes and billing in our daily work. Here are some of the most common ones:
What are the most common ICD-10 codes used in podiatry?
While the list is extensive, some of the most frequently seen ICD-10 codes in podiatry include:
- Plantar Fasciitis (M72.2): A classic foot complaint causing heel pain.
- Ingrown Nail (L60.0): Onychocryptosis, often requiring nail avulsion.
- Diabetic Foot Ulcer (E11.621 for Type 2 diabetes with foot ulcer, left foot): Given the prevalence of diabetes, these are unfortunately common and require meticulous coding. Note the laterality and specificity.
- Corns and Callosities (L84): Hyperkeratotic lesions often treated with paring or trimming.
- Foot Pain (M79.67-): Often used as a symptom code, requiring further specificity (e.g., M79.671 for pain in left foot, M79.672 for pain in right foot).
Specificity is key with ICD-10 codes. Always choose the most detailed code available that accurately reflects the patient’s diagnosis, including laterality and severity where applicable.
What is the difference between CPT codes 11720 and 11721?
These two podiatry CPT codes are specifically for nail debridement, and the distinction is simple but critical:
- 11720: Debridement of 1-5 nails. This code is used when you debride up to five nails during a single encounter.
- 11721: Debridement of 6 or more nails. This code is used when you debride six or more nails in one session.
The medical necessity for performing debridement, especially for mycotic (fungal) nails, must be well-documented. For instance, if the mycotic nails are causing pain or limiting ambulation, or if the patient has underlying systemic conditions that make professional debridement necessary (e.g., diabetes), this should be clearly stated in the patient’s record.
How do podiatry billing codes differ globally?
The podiatry CPT codes discussed here are specific to the United States. CPT is the proprietary system from the American Medical Association (AMA) used for reporting medical services in the U.S.
Globally, coding systems vary significantly. While the World Health Organization (WHO) is developing the International Categorization of Health Interventions (ICHI) to standardize classifications, regional differences persist. Practicing in Canada or the UK, for example, would involve entirely different coding systems. Our focus remains on the U.S. healthcare landscape, which is relevant for practices in states like New Jersey, Nevada, Nebraska, North Carolina, and Kentucky.
Conclusion: Take Control of Your Podiatry Revenue Cycle
We’ve covered a lot of ground, from the foundational understanding of podiatry CPT codes and their workflow to the intricate dance with Medicare rules, the power of modifiers, and the crucial role of documentation in preventing denials. The message is clear: accurate and compliant coding is not merely an administrative task; it is the financial backbone of your podiatry practice.
The U.S. podiatry market is growing due to an aging population and the prevalence of diabetes, meaning more patients need your care. This growth is only sustainable with a healthy, efficient revenue cycle. Given the high improper payment rates and evolving coding guidelines, specialized expertise in podiatry billing is a necessity, not a luxury.
A proactive revenue cycle management (RCM) strategy, built on meticulous documentation, accurate code selection, diligent denial management, and regular audits, is your best defense against lost revenue. It ensures that every service you provide is translated into timely and accurate reimbursement.
If the complexities of podiatry billing and coding are causing headaches, you don’t have to steer them alone. We specialize in providing custom, 100% US-based billing and RCM services exclusively for podiatry practices. Our dedicated team understands the unique challenges you face and is committed to maximizing your collections and streamlining your operations.
Ready to take control of your practice’s financial health? Explore our specialized Billing Services to see how we can help your practice thrive.