From Foot to Fortune: Mastering Podiatry Practice Billing
Why Podiatry Practice Billing Demands Specialized Expertise
Podiatry practice billing is a highly complex field, demanding specialized knowledge of unique codes, modifiers, and payer policies that differ from other medical specialties. Mastering it is crucial for financial success.
Key challenges include:
- Specialized Coding: Using unique CPT codes (e.g., 11720-11721 for nail debridement) and specific ICD-10 codes for foot and ankle conditions.
- Medicare Q Modifiers: Applying Q7, Q8, and Q9 modifiers to justify routine foot care based on systemic conditions.
- Medical Necessity: Clearly documenting the link between systemic diseases (like diabetes) and the foot care provided.
- Routine vs. Medical Care: Distinguishing between covered medical treatments and non-covered routine services.
- Complex Modifiers: Correctly using modifiers like 25, 59, LT/RT, and toe-specific modifiers (TA-T9).
- Prior Authorizations: Managing pre-authorization for orthotics, procedures, and workers’ compensation cases.
The stakes are high. Inaccurate coding triggers denials, delayed payments, and audits. Medicare and private payers have strict rules for medically necessary foot care, and a single error can result in zero payment. Most podiatrists lack formal billing training, making in-house management time-consuming and risky.
Understanding these unique requirements is the first step to improving your practice’s financial health. Whether you face high denial rates or spend too much time on administrative tasks, mastering podiatry billing is essential for long-term success.
The Unique Landscape of Podiatry Billing
The world of podiatry practice billing is a complex ecosystem. Unlike general medicine, podiatry deals with a unique blend of routine care, acute injuries, chronic conditions, and surgical procedures affecting the feet and ankles. This specialized focus, so essential for overall health, brings distinct billing challenges that require a deep understanding to ensure financial stability.
What Makes Podiatry Practice Billing Unique?
Podiatry practice billing is set apart by its highly specialized services, from routine nail care to complex surgeries. A key differentiator is the need for specific modifiers and “class findings” to justify medical necessity, especially for services that might otherwise be deemed routine. For instance, nail debridement’s coverage hinges on whether a systemic condition like diabetes makes it medically necessary.
Serving a large Medicare population means navigating complex guidelines. The mix of medical and surgical services in one visit, plus pre-authorization needs for orthotics and unique protocols for workers’ compensation, adds layers of complexity. This requires precise coding and documentation to avoid denials.
Common Challenges and Their Financial Impact
Podiatry practices face a minefield of billing challenges that impact financial health. Claim denials are a primary issue, with common denial reasons in podiatry including lack of medical necessity, missing class findings, incorrect modifier use, and missing prior authorizations. A single error can lead to a rejected claim.
Other challenges include frequent coding updates, varied insurance policies, and difficult patient collections. These factors increase administrative burdens, delay payments, and reduce revenue. Higher denial rates mean less cash flow and more staff time spent chasing payments, increasing audit risks.
Medicare vs. Private Payer Policies
In podiatry practice billing, Medicare often sets the standard, but private payers have their own rules. Medicare has very specific guidelines for routine foot care, generally not covering services like nail trimming unless medically necessary due to a systemic condition (e.g., diabetes, vascular disease). This requires meticulous documentation and specific modifiers. You can find more details in our dedicated resource on Medicare Podiatry Billing Guidelines.
Private insurance policies vary significantly. A payer like Blue Cross Blue Shield may cover a wide range of treatments with accurate coding, but their prior authorization requirements or coverage criteria can differ from Medicare’s. Staying updated on each payer’s unique policies is a constant challenge.
Coding, Modifiers, and Documentation: The Core of Reimbursement
At the heart of successful podiatry practice billing is the trio of accurate coding, precise modifier application, and impeccable documentation. These elements are the bedrock of your claims and dictate whether you receive proper reimbursement or face denials.
Essential CPT and ICD-10 Codes
Mastering CPT and ICD-10 codes is non-negotiable. CPT codes describe the services you provide, while ICD-10 codes explain the diagnosis.
Common Podiatry CPT Codes:
- Office Visits (E/M): 99203-99205 (New), 99213-99215 (Established)
- Routine Foot Care: 11720-11721 (Nail Debridement), 11055-11057 (Callus Removal)
- Procedures: 11730-11750 (Nail Avulsion), 20550 (Plantar Fascia Injection), 28285 (Hammertoe Correction)
- Orthotics (HCPCS): L3020-L3040 (Custom Fittings)
For ICD-10 codes, specificity is key (e.g., M77.31 for right-foot plantar fasciitis). Every procedure must be linked to a qualifying diagnosis. For practical examples, you can refer to guides like the Podiatry Services Billing Examples: CMS-1500.
The Critical Role of Modifiers
Modifiers add crucial context to your services. Without them, even correctly coded claims can be rejected.
- Q Modifiers (Q7, Q8, Q9): Unique to Medicare, these justify routine foot care by indicating systemic conditions.
- Modifier 25: Appended to an E/M code when a significant, separate E/M service is performed on the same day as a minor procedure.
- Modifier 59: Used to unbundle procedures performed on different anatomical sites on the same day.
- Laterality (LT, RT) & Toe (TA-T9) Modifiers: Provide essential anatomical specificity.
- Modifier 50: Indicates a bilateral procedure.
Proper modifier use is critical for telling the full story of the patient’s care and ensuring accurate reimbursement.
How Systemic Conditions and Documentation Drive Coverage
Medical necessity is proven at the intersection of systemic conditions and thorough documentation. Many patients have underlying health issues like diabetes, peripheral neuropathy, or vascular disease that directly impact their foot health and service coverage.
Medicare, for example, only covers routine foot care if a systemic condition makes the patient high-risk. Meticulous clinical documentation is your superpower here. SOAP notes must clearly link the foot condition to the systemic disease by detailing patient history, physical exam findings (including Class A, B, C findings), and a clear assessment of medical necessity. Without this explicit link, claims will likely be denied. As a podiatrist treats a wide range of issues, your documentation must reflect the medical necessity of every intervention.
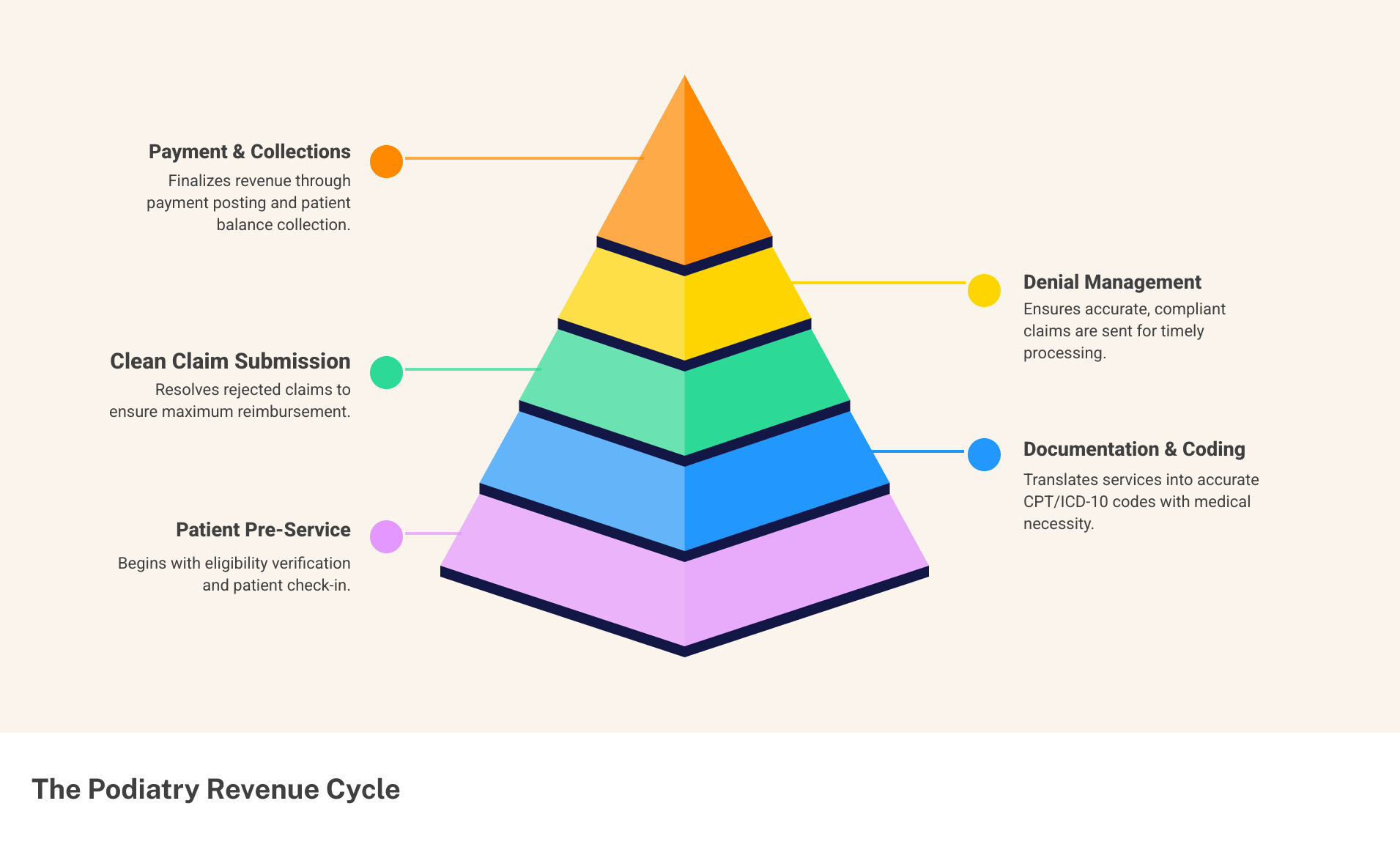
The Comprehensive Podiatry Practice Billing Workflow
A comprehensive workflow is essential for effective podiatry practice billing. It’s a systematic approach from patient scheduling to final payment, designed to maximize reimbursement and minimize administrative headaches. A structured process prevents lost revenue and ensures every step is executed with precision.
From Patient Encounter to Clean Claim Submission
The journey to a clean claim starts before the patient arrives. A meticulous workflow increases first-pass resolution and accelerates payments.
- Patient Eligibility Verification: Verify eligibility when the appointment is scheduled and again before the visit to prevent surprises.
- Accurate Clinical Documentation: Support every service with comprehensive SOAP notes that detail medical necessity, comorbidities, and laterality.
- Code & Modifier Selection: Choose the correct CPT, HCPCS, and ICD-10 codes, and append appropriate modifiers (Q-modifiers, 25, 59, etc.) to provide context.
- Claim Scrubbing: Before submission, use claim scrubbing tools to perform a pre-submission audit, which can catch up to 80% of common errors.
- Timely Claim Submission: Submit scrubbed claims electronically, adhering to payer filing deadlines to avoid automatic denials.
Best Practices for Managing Denials in Podiatry Practice Billing
Denials are inevitable, but how you manage them is key. A robust denial management strategy is crucial for a healthy revenue cycle.
- Act Quickly: Address denials daily. The faster you act, the higher the chance of a successful appeal.
- Identify Root Causes: Log each denial to understand the reason—be it a coding error, documentation issue, or eligibility problem—to prevent future occurrences.
- Appeal Effectively: Initiate appeals promptly within the payer’s timeframe (often 30-90 days), supported by strong documentation.
- Track Trends: Analyze denial data to identify patterns with specific codes or payers, informing process improvements.
Measuring Success: Key Performance Indicators (KPIs)
To know if your podiatry practice billing efforts are working, you must measure them. Tracking Key Performance Indicators (KPIs) gauges your practice’s financial health and allows for data-driven decisions.
Essential KPIs include:
- Clean Claims Rate: The percentage of claims paid on the first submission.
- Days in Accounts Receivable (A/R): The average time to collect payments.
- Collection Ratio: The percentage of collectible revenue that is actually collected.
- Denial Rate: The percentage of claims denied by payers.
- A/R Aging Report: A breakdown of outstanding claims by age (e.g., 0-30, 31-60, 90+ days).
Regularly monitoring these KPIs provides invaluable insights. You can learn more about Financial Health KPIs and how to Live and Die by KPIs: The Podiatrist’s Guide to Practice Growth and Profitability.
Optimizing Your RCM: Technology and Outsourcing
In today’s healthcare environment, optimizing your revenue cycle management (RCM) is about more than just codes; it’s about embracing efficiency through technology and external expertise. For podiatry practice billing, this means streamlining operations to free up valuable time for patient care.
Leveraging Technology to Streamline Operations
Modern software is an indispensable ally for efficient podiatry practice billing, automating tasks and improving accuracy.
Key tools include:
- Automated Eligibility Checks: Verify patient insurance automatically before the visit to reduce eligibility-related denials.
- AI-Suggested Codes: Use AI to analyze notes and suggest accurate billing codes, minimizing errors.
- Claim Scrubbing Tools: Identify and flag common errors before submission to improve first-pass resolution rates.
- Patient Portals & Online Payments: Empower patients to check in, view balances, and pay online, improving collections and satisfaction.
- Cloud-Based Software: Ensure your team always has access to the latest CPT and ICD-10 code sets for compliance.
- Electronic Remittance Advice (ERA): Track claims online and access EOBs for faster payment posting.
Embracing these technologies makes billing more efficient and profitable. For practices considering a switch, navigating your transition to a new EHR is a critical step.
When to Consider Outsourcing Your Podiatry Practice Billing
Many practices find outsourcing their podiatry practice billing to be a game-changer. The decision often comes down to time, cost, and a need for specialized expertise.
Consider outsourcing if you experience:
- Time Constraints: You want to focus more on patient care and less on administrative tasks.
- High Denial Rates: Your in-house team is struggling to keep up with complex podiatry rules.
- Staffing Issues: Recruiting and retaining skilled billing staff is challenging and costly.
- A Need for Deeper Expertise: You want to leverage a team with specialized knowledge to maximize collections.
- Cost-Inefficiency: The total cost of in-house billing (salaries, errors, lost revenue) is too high.
Outsourcing frees you to focus on patients while experts handle the complexities of billing. A partnership with a specialized service can save time, reduce stress, and improve your practice’s financial health.
Frequently Asked Questions about Podiatry Billing
How often can routine foot care codes like 11721 be billed to Medicare?
Medicare may cover code 11721 (debridement of 6+ nails) roughly every 60 days, but only if it is medically necessary. The patient must have a qualifying systemic condition (e.g., diabetes, vascular disease) that puts them at high risk. This must be clearly documented with specific “class findings” and justified with the appropriate Q modifier (e.g., Q8). Without this, the service is considered routine and will not be covered.
What is the difference between modifier 59 and modifier 25?
These modifiers distinguish separate services performed on the same day:
-
Modifier 25: Appended to an E/M service code (e.g., 99213-25), it indicates a significant, separately identifiable E/M service was performed on the same day as a minor procedure (e.g., evaluating new heel pain during a visit for an ingrown nail removal).
-
Modifier 59: Appended to a procedure code, it indicates two procedures that are normally bundled were performed at different anatomical sites or in separate encounters on the same day (e.g., callus removal on the right foot and wart removal on the left).
Correctly using these modifiers is vital for accurate reimbursement.
Why is credentialing important for podiatry billing?
Credentialing is critical for podiatry practice billing because it verifies a provider’s qualifications with insurance payers, allowing them to become “in-network.” Without proper credentialing, claims will be rejected or paid at much lower out-of-network rates. This process is mandatory for receiving payments from insurers and retaining patients who rely on their coverage. The CAQH ProView system helps streamline this process by creating a centralized database for providers, but it can still take 90-120 days and must be managed proactively.
Conclusion
Mastering podiatry practice billing is about building a robust system for financial health. By focusing on meticulous documentation, accurate coding, and proactive denial management, you can improve your clean claims rate, reduce A/R days, and boost collections. This approach minimizes administrative burdens and allows you to focus on providing exceptional patient care.
The value of specialized expertise cannot be overstated. Our 100% US-based team specializes exclusively in podiatry, offering custom solutions to maximize your collections and streamline operations.
Take the next step towards financial health for your practice with our specialized billing services.

