Medicare Podiatry Billing Guidelines: Expert 2026
Why Medicare Podiatry Billing Guidelines Matter for Your Practice
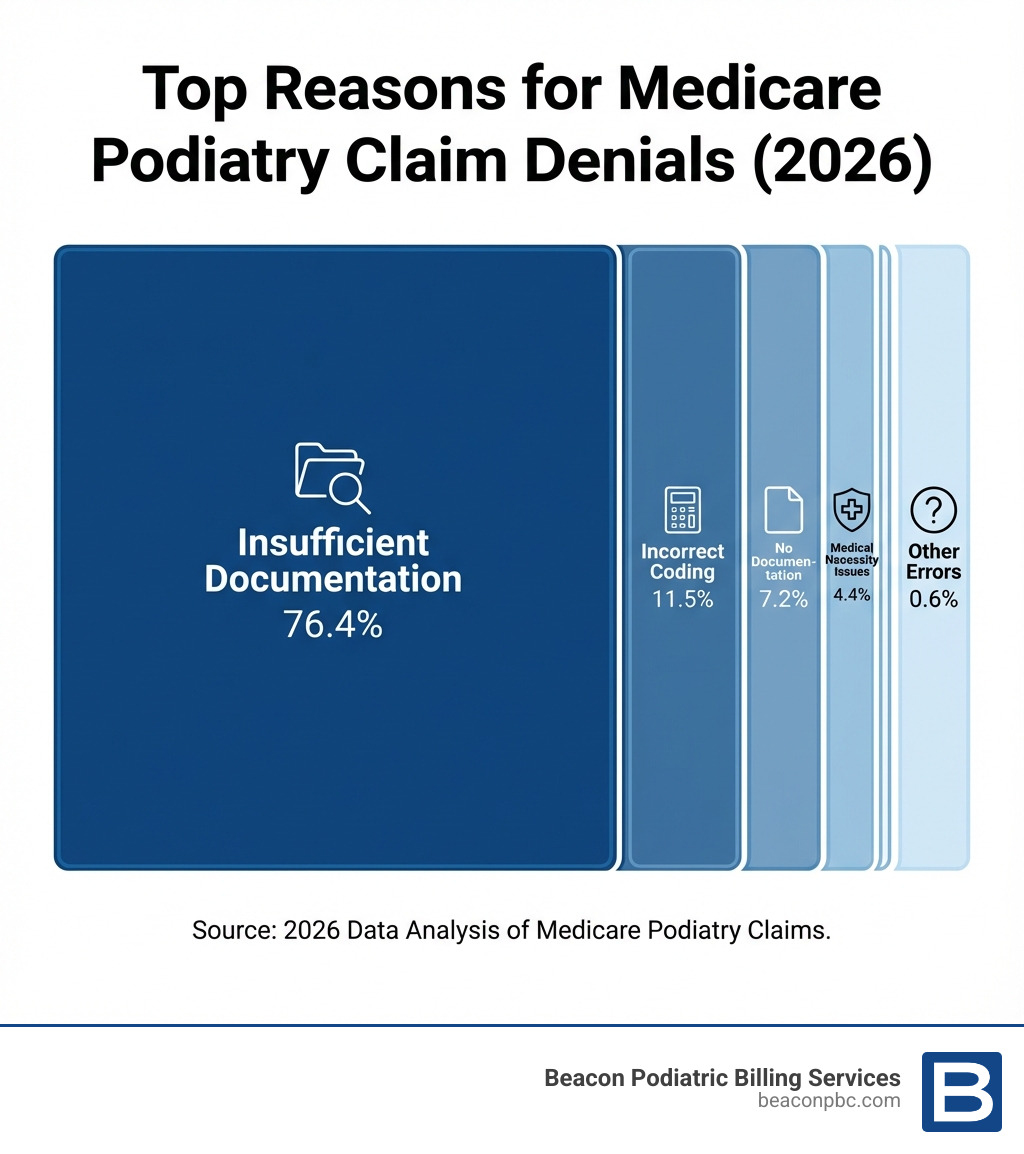
Medicare podiatry billing guidelines are complex rules that determine which foot care services Medicare will cover and pay for. If you’re a podiatrist struggling with denied claims, delayed payments, or spending too much time on billing, you’re not alone. The improper payment rate for podiatry care under Medicare Part B was 11.2% in 2024, totaling $216.9 million in projected improper payments. Even more concerning: 76.4% of these denials were due to insufficient documentation.
Quick Guide to Medicare Podiatry Billing Guidelines:
- Medically necessary services for foot injuries or diseases (bunions, hammertoes, heel spurs) are generally covered
- Routine foot care (nail trimming, corn removal) is typically not covered
- Exceptions apply when patients have systemic conditions like diabetes or peripheral neuropathy
- Proper documentation of medical necessity is essential for every claim
- Specific modifiers (Q7, Q8, Q9) are required to justify routine care exceptions
- Frequency limits apply – typically once every 60-61 days for routine services
Understanding these guidelines isn’t just about compliance. It’s about protecting your practice’s financial health and maximizing your reimbursement for legitimate services.
The good news? Once you understand the foundation of what Medicare covers, the exceptions that allow routine care coverage, and the documentation requirements that prove medical necessity, you can significantly reduce denials and streamline your billing process.
The Foundation: Covered vs. Non-Covered Podiatry Services
Navigating Medicare podiatry billing can feel like tiptoeing through a minefield. The first step to a smooth journey is understanding the fundamental distinction between what Medicare Part B generally covers and what it typically excludes.
Medicare Part B is designed to cover medically necessary services, which means care needed to diagnose or treat a medical condition. For podiatry, this translates to services for injuries, diseases, or other medical conditions affecting the foot, ankle, or lower leg. These services must be delivered by a physician (M.D.) or a Medicare-certified podiatrist (DPM). You can dive deeper into these specifics by checking out the Official CMS guidelines for podiatry.
What Medicare Part B Generally Covers
When we talk about medically necessary care, we’re referring to treatments for diagnosed conditions that require professional intervention. This includes:
- Injury Treatment: Services related to acute injuries of the foot or ankle.
- Disease Management: Treatment for specific diseases affecting the lower extremities. This includes conditions like hammer toe, bunion deformities, and heel spurs, where the podiatrist is addressing a diagnosed medical issue rather than just cosmetic concerns or routine maintenance.
- Wound Care: Treatment for ulcers, infections, and other wounds on the feet, especially common in patients with systemic conditions.
- Diagnostic Services: Initial evaluations and tests to diagnose a covered condition.
If a service is deemed medically necessary for the treatment of injury, disease, or other medical conditions affecting the foot, ankle, or lower leg, and is provided by a qualified professional, Medicare Part B generally has your back.
What is Considered Non-Covered Routine Foot Care?
Here’s where many practices can get tripped up. Medicare generally does not cover routine foot care. Think of it as your everyday foot maintenance – the kind of care most individuals can perform themselves or that doesn’t stem from a specific, complex medical condition that puts the patient at significant risk.
Examples of routine foot care that are typically non-covered include:
- Nail Trimming/Clipping/Debridement: Unless specific medical criteria are met, simply cutting or trimming nails is considered routine.
- Corn and Callus Removal: The cutting or removal of corns and calluses for general comfort or cosmetic reasons.
- Hygienic Maintenance: Services like cleaning or soaking feet, or other preventive care without localized illness, injury, or symptoms.
- Supportive Devices for Flat Feet: While some orthotics may be covered under specific circumstances (like therapeutic shoes for diabetics), general supportive devices for flat feet are typically excluded.
- Services for Cosmetic Purposes: Any procedure performed solely for aesthetic improvement without an underlying medical necessity.
It’s crucial to remember that the exclusion of foot care is determined by the nature of the service, not by who provides it. So, even if a highly skilled podiatrist performs these services, they are generally non-covered unless specific exceptions apply. And that brings us to the exciting part: the exceptions!
The Exception Rule: When Routine Foot Care IS Covered
While routine foot care often falls outside Medicare’s coverage umbrella, there’s a significant “but” – and it’s a big one for podiatry practices. Medicare will cover routine foot care services if they are medically necessary due to certain systemic conditions that put the patient at high risk of complications if the care isn’t performed by a professional. This is where the medicare podiatry billing guidelines get interesting and require careful attention.
The key here is medical necessity, specifically linked to an increased risk of complications. If a patient has a systemic condition that makes professional foot care essential to prevent serious issues like infection, ulceration, or even amputation, then Medicare may step in.
Qualifying systemic conditions that can justify coverage for routine foot care include:
- Diabetes Mellitus: A primary driver of foot complications.
- Peripheral Vascular Disease (PVD): Conditions like Arteriosclerosis obliterans and Chronic thrombophlebitis that affect circulation.
- Peripheral Neuropathies: Conditions that cause diminished sensation in the feet, making self-care dangerous.
- Malnutrition: Can impair healing and increase susceptibility to infection.
- Alcoholism: Often associated with neuropathy and poor self-care.
- Malabsorption: Leading to nutritional deficiencies that affect foot health.
- Pernicious Anemia: Can contribute to neurological issues.
- Uremia (chronic renal disease): Associated with various systemic complications affecting the feet.
- Traumatic Injury: Past injuries that leave the foot vulnerable.
- Leprosy or Neurosyphilis: Conditions that cause nerve damage.
- Hereditary Disorders: That impact foot health and sensation.
- Diabetic Sensory Neuropathy with Loss of Protective Sensation (LOPS): A specific and critical condition for diabetic foot care coverage.
For more insights into optimizing your practice’s operations and understanding how these nuances impact your overall business, explore our resources on Practice Management Growth.
The Role of Systemic Conditions in Medicare Podiatry Billing Guidelines
Systemic conditions don’t just affect one part of the body; they can have widespread impacts, and the feet are often ground zero for serious complications. For instance, diabetes can lead to poor circulation (peripheral arterial disease) and nerve damage (neuropathy), making a simple ingrown toenail a gateway to a severe infection or ulcer. This is why professional foot care becomes medically necessary for these patients.
Our job as providers and billers is to clearly link the patient’s systemic diagnosis to the need for the foot care service. It’s about demonstrating that without professional intervention, the patient faces a significant hazard. This justification is central to successful medicare podiatry billing guidelines.
The “Active Care” Requirement
Another critical piece of the puzzle for justifying routine foot care under Medicare is the “active care” requirement. For many of the systemic conditions that make routine foot care medically necessary, Medicare requires that the patient be under the active care of a managing physician (an M.D. or D.O.) for that underlying condition.
What does “active care” mean? It generally means the patient has been seen by their primary physician for the complicating systemic disease process within the six-month period prior to the podiatry service. This confirms that the systemic condition is being managed and that the podiatry service is an integral part of the patient’s comprehensive care plan.
When submitting claims for these services, we must include the name of the managing physician and the approximate date the beneficiary was last seen by that physician. Failing to provide this information can lead to claim denials, even if the medical necessity is otherwise perfectly clear. It’s Medicare’s way of ensuring a holistic approach to patient care and preventing isolated treatments.
Cracking the Code: Essential CPT Codes and Modifiers
Once you understand what Medicare covers and the circumstances under which routine foot care becomes reimbursable, the next step is translating that medical necessity into the language of billing: CPT codes and HCPCS modifiers. These codes are the backbone of medicare podiatry billing guidelines, telling the story of the service provided and why it was necessary. Accurate coding is paramount; a single misplaced digit or forgotten modifier can send your claim spiraling into denial purgatory.
To avoid coding errors, not only know the codes but also understand their coverage implications and how they link directly to your detailed documentation.
Here’s a quick reference for the crucial Class Findings and their corresponding Q Modifiers:
| Class Finding Description | Q Modifier | Example |
|---|---|---|
| Class A Finding: Nontraumatic amputation of a foot or part of a foot. | Q7 | Patient has a previous amputation of the left second toe. |
| Two Class B Findings: Patient has at least two findings from the Class B list, which includes absent pulses (posterior tibial, dorsalis pedis) and advanced trophic changes. | Q8 | Patient has an absent dorsalis pedis pulse and advanced trophic changes (e.g., thin, shiny skin). |
| One Class B and One Class C Finding: Patient has one finding from the Class B list (e.g., absent pulse) and one from the Class C list (sensory changes like burning, numbness, or claudication). | Q9 | Patient has an absent posterior tibial pulse (Class B) and reports burning pain in their feet (Class C). |
