Revenue cycle management podiatry: Top 5 KPIs for Success
Why Your Podiatry Practice’s Financial Health Depends on RCM
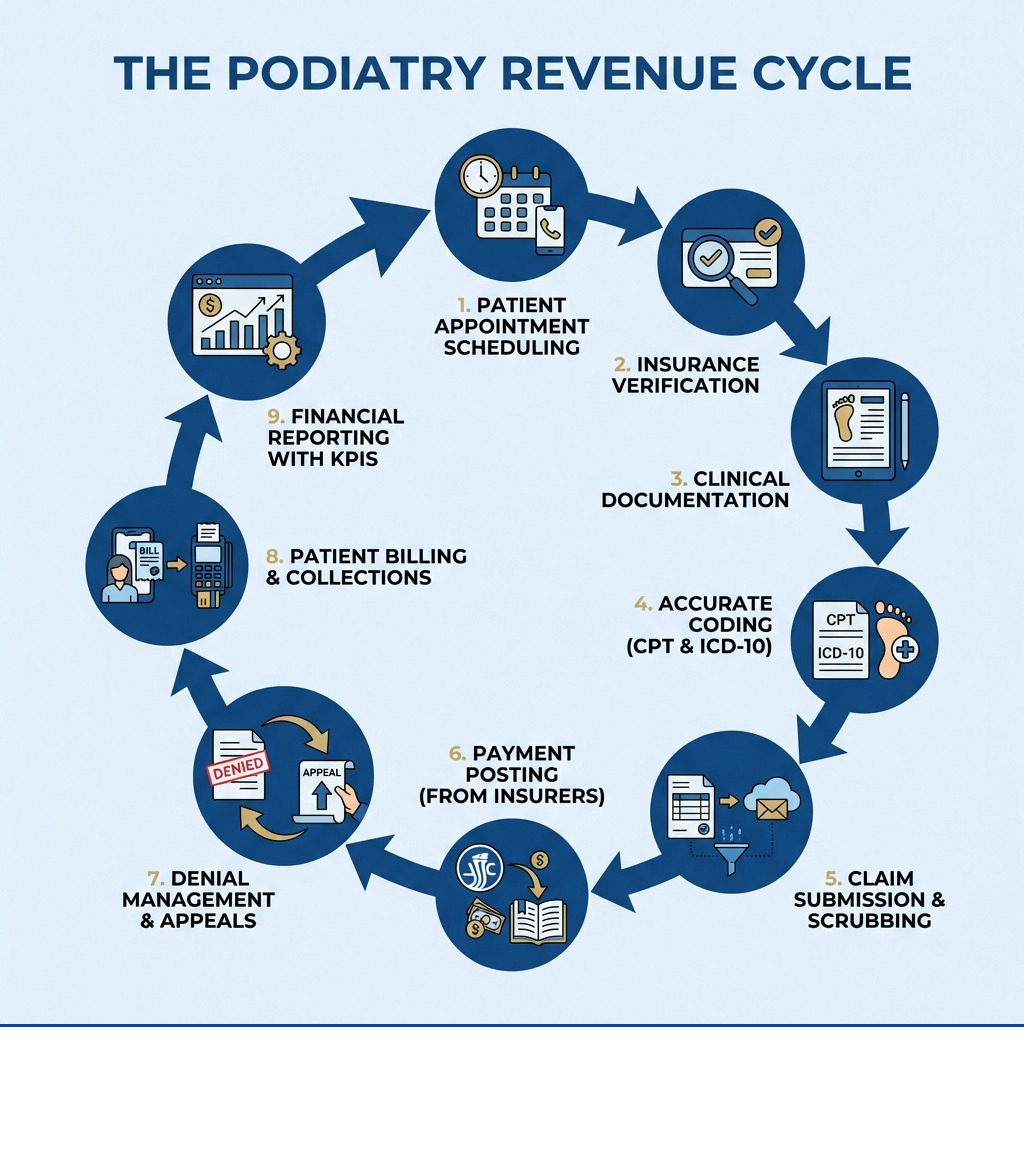
Revenue cycle management podiatry is the complete process of tracking patient care from initial appointment to final payment, including registration, insurance verification, coding, claim submission, payment posting, and denial management.
Quick Answer: Key Components of Podiatry RCM
- Patient Registration & Verification – Capture accurate demographics and verify insurance eligibility
- Documentation & Coding – Use correct CPT, ICD-10 codes and modifiers (Q7, Q8, Q9)
- Claim Submission – Submit clean claims that meet payer-specific requirements
- Payment Posting – Track and reconcile all payments from insurers and patients
- Denial Management – Appeal denied claims and prevent future rejections
- Patient Collections – Manage copays, deductibles, and outstanding balances
You focus on treating diabetic foot ulcers, performing nail debridements, and helping patients walk pain-free. But managing the billing process? That’s often where your revenue walks right out the door.
The numbers tell a sobering story. The average podiatry practice faces denial rates of 5-8% or higher due to complex coding requirements. Even worse, 50-60% of denied claims are never reworked, representing pure lost revenue. And each time you need to rework a claim, it costs your practice $251.
Many podiatrists underestimate just how complex medical billing has become. Between Medicare Local Coverage Determinations (LCDs), payer-specific rules for routine foot care, and the constant changes to coding requirements, it’s no wonder billing issues pull you away from patient care.
A reliable revenue cycle management system doesn’t just get you paid faster. It prevents the administrative burden from overwhelming your staff, reduces claim rejections from common mistakes, and ensures you’re capturing revenue for every service you provide.
The Unique Financial Problems in Podiatry Billing
As podiatrists, you deal with a unique blend of chronic conditions, injuries, and specialized procedures. This specificity, while making your work incredibly rewarding, also creates distinct challenges in the revenue cycle management podiatry landscape. The financial health of your practice depends on navigating these intricate obstacles.

We understand that you want to focus on keeping your patients moving, whether treating diabetic foot ulcers, chronic wounds, or addressing common podiatric conditions. However, managing your practice’s revenue cycle can often feel like a burden, pulling you away from what you do best. Our goal is to help you overcome these challenges and achieve financial stability.
The Intricacies of Podiatry Coding and Modifiers
The language of medical billing is complex, and for podiatry, it’s practically a dialect all its own. We’re talking about specific Current Procedural Terminology (CPT) codes, International Classification of Diseases (ICD-10) codes, and a host of modifiers that can make or break a claim.
For instance, common podiatry CPT codes might include:
- 58550 – Cryotherapy of Skin Lesion(s)
- 20550 – Injection tendon sheath/ligament
- 11740 – Total nail avulsion
- 11730 – Debridement of nail(s)
And ICD-10 codes can range from those related to diabetic foot ulcers (e.g., E11.621) and chronic foot ulcers (e.g., L97.519) to hammer toes (M20.41) and onychomycosis (B35.1).
But it’s not just about knowing the codes; it’s about understanding their nuances. Podiatry frequently uses special modifiers, like -Q7, -Q8, and -Q9, which indicate different levels of medical necessity for routine foot care, especially for at-risk patients. Misusing or omitting these can lead to immediate denials. The concept of “medical necessity” is crucial here, as insurance companies, not just physicians, often arbitrate what’s considered medically necessary for claim approval.
The challenge is further compounded by the need for clear documentation that supports these codes. Incorrect coding or insufficient documentation is a leading cause of claim rejections and delayed payments. Our team stays updated on these complex rules to ensure your claims are accurate and compliant. For a deeper dive into these specifics, check out The Foot-Friendly Guide to Podiatry Billing and Coding.
Navigating Payer Policies and Audit Risks
Beyond coding, podiatry practices face a labyrinth of payer-specific policies, particularly from Medicare and commercial insurers. We must be intimately familiar with Medicare Local Coverage Determinations (LCDs) published for regions like New Jersey, Nevada, Nebraska, North Carolina, and Kentucky. These LCDs contain vital information regarding required documentation, specific CPT codes, and linked ICD codes for various podiatric services.
Commercial payers also have their own changing guidelines, often requiring pre-authorizations for certain procedures or dictating specific documentation standards. For example, HMO insurance often requires a referral from a Primary Care Provider (PCP) as the initial step for specialist visits. If this isn’t tracked and obtained, the claim will be denied.
The regulatory environment is constantly shifting, increasing the risk of audits. Inadequate documentation and coding can trigger an audit, leading to significant financial penalties. It’s a daunting prospect, but with a proactive approach to compliance, we can safeguard your practice. As we know, one-third of insurance denials are due to eligibility issues – a highly preventable problem. The cost of reworking a claim, on average, is $251. This is why it’s critical to get it right the first time. To learn how to protect your practice, explore Audit-Proof Your Practice: A Guide to Podiatry Billing Compliance.
A Step-by-Step Guide to the Podiatry RCM Process
Understanding the entire revenue cycle management podiatry process is like understanding the flow of blood through the body – every part is crucial for overall health. Let’s walk through the key stages that ensure your foot traffic translates into healthy cash flow.

Front-End Essentials: Patient Registration and Insurance Verification
This is where the journey begins, and arguably, where many potential problems can be prevented. Accurate patient registration is paramount. This means capturing correct demographic information – name, address, date of birth, and current insurance details. It sounds simple, but errors here are astonishingly common and lead to frustrating claim rejections.
Next comes insurance verification. This isn’t just a quick check; it’s a deep dive. We verify eligibility, understand the patient’s benefits, and determine copayments, deductibles, and co-insurance responsibilities. Why is this so vital? Because as much as one-third of all insurance denials are due to eligibility issues. That’s a highly preventable problem that costs practices thousands.
Instead of calling insurance companies on the phone (which is, let’s be honest, a colossal time sink), we leverage technology to perform quick, accurate eligibility checks. This proactive step allows us to communicate financial responsibilities to patients upfront, reducing surprises and improving collection rates. For insights into Medicare specifics, which are particularly relevant for many podiatry patients, see Demystifying Medicare Podiatry: What’s Covered, When, and How to Calculate Costs.
Mid-Cycle Mastery: Documentation, Coding, and Timely Claim Submission
Once the patient has been seen, the clinical details must be carefully translated into billing language. This is where clinical documentation improvement (CDI) becomes your best friend. Every procedure performed, every diagnosis made, must be thoroughly documented in the patient’s electronic health record (EHR) to support the codes chosen. Meticulous clinical notes are not just for patient care; they are your strongest defense against denials.
Then comes the coding. Using the correct CPT and ICD-10 codes, along with appropriate modifiers, is essential. We ensure the diagnosis codes accurately link to the procedures performed, justifying the medical necessity of the service. This attention to detail is critical for creating “clean claims” – claims that are free of errors and ready for submission.
Timely claim submission is another non-negotiable. Payers have strict filing deadlines, and missing them means lost revenue. Before submission, we use claim scrubbing tools to review claims for potential conflicts or missing information. This proactive step catches errors before they become rejections, ensuring a higher clean claim rate and faster reimbursement. Staying informed about the latest changes in coding is crucial, as discussed in Billing & Coding Updates.
Best Practices for Optimizing Revenue Cycle Management Podiatry
Optimizing your revenue cycle management podiatry isn’t a one-time fix; it’s an ongoing commitment to financial health. By implementing strategic best practices, we can transform your practice’s financial performance and operational efficiency.
Strategies to Maximize Reimbursements and Reduce Denials
Denials are the bane of every practice’s existence, but many are preventable. Here are some common reasons for podiatry claim denials and how we tackle them:
- Eligibility Issues: As mentioned, a huge culprit. Our robust verification process catches these upfront.
- Coding Errors: Incorrect CPT, ICD-10, or modifier usage. We employ certified coders with podiatry-specific expertise.
- Lack of Medical Necessity: Insufficient documentation to justify the procedure. We emphasize thorough clinical notes.
- Timely Filing Limits: Claims submitted past the payer’s deadline. Our streamlined process ensures prompt submission.
- Bundling/Unbundling Issues: Incorrectly billing for services that should be grouped or separated. We stay updated on payer rules.
- Missing or Incorrect Authorizations: Failing to obtain necessary pre-approvals. We manage this proactively.
We conduct root cause analysis for every denial, identifying patterns and implementing preventive measures. This includes payer-specific compliance checks, ensuring correct modifier usage (like those tricky Q-modifiers for routine foot care), and ensuring that every billable service you provide is captured and reimbursed. It’s astonishing that 50-60% of all denials are never worked to adjudication – that’s pure lost revenue that we’re committed to recovering for you. We help you identify those high-profit procedures and ensure they’re billed correctly. Learn more about maximizing your earnings in High-Profit Procedures: Smart Strategies Your Guide to Podiatry Revenue Growth.
Enhancing the Patient Financial Experience
A smooth billing process isn’t just good for your bottom line; it significantly improves the patient experience. When patients understand their financial obligations and find the billing process transparent and easy, their satisfaction increases, fostering loyalty and positive reviews.
We advocate for transparent billing policies, clearly communicating expected costs, copays, and deductibles before services are rendered. This prevents surprises and reduces patient frustration. Patient-friendly statements that are clear, concise, and easy to understand also make a big difference. Offering convenient payment options, including online portals and payment plans, empowers patients to manage their bills effectively. We believe that clear communication and a patient-centric approach to billing contribute to a healthier overall practice, as highlighted by our testimonials.
Technology and Strategic Partnerships: Your Levers for RCM Excellence
In today’s healthcare environment, leveraging the right technology and forming strategic partnerships are not just options; they are necessities for achieving revenue cycle management podiatry excellence.
| Feature | In-House RCM | Partnering with Specialized Podiatry RCM Service |
|---|---|---|
| Cost | High overhead (staff salaries, benefits, training, software, infrastructure, office space) | Variable, typically percentage of collections (no fixed overhead) |
| Expertise | Requires continuous in-house training; limited exposure to diverse payer rules | Access to certified, podiatry-specific experts; up-to-date on all regulations |
| Efficiency | Can be slow due to staff limitations, manual processes, and learning curves | Streamlined workflows, advanced technology, faster claim processing, higher clean claim rates |
| Compliance | High risk of errors due to lack of specialized knowledge; difficult to stay updated | Proactive compliance management, reduced audit risk, adherence to LCDs and payer rules |
| Focus | Diverts practice focus from patient care to administrative tasks | Allows practice to fully concentrate on patient care and clinical excellence |
The Role of Technology in Modern Revenue Cycle Management Podiatry
Technology is a game-changer in RCM. Automated eligibility verification systems, for example, can instantly confirm patient insurance details, drastically reducing denials caused by eligibility issues. Smart coding suggestions within EHR systems can guide your team to select the most accurate CPT and ICD-10 codes, minimizing errors.
Advanced reporting tools provide deep insights into your practice’s financial performance, allowing us to identify trends, pinpoint bottlenecks, and make data-driven decisions. Patient payment portals offer convenience for patients and streamline your collection process. We are always exploring how innovations like AI can further improve efficiency, from natural language data capture for medical dictation to proactive alerts on claims likely to be denied. We also integrate seamlessly with popular EHRs used in podiatry to ensure a connected ecosystem. Find more about how technology can boost your practice in Technology in Podiatry.
In-House vs. Partnering with a Podiatry RCM Expert: Making the Right Choice
The decision to manage RCM in-house or outsource it is a critical one for any podiatry practice. While an in-house team offers direct control, it comes with significant challenges: the cost of recruiting, training, and retaining specialized billing staff; the constant need for education on evolving regulations; and the administrative burden that diverts focus from patient care.
Partnering with a specialized podiatry RCM expert, like us, offers compelling advantages:
- Cost Savings: By avoiding the expenses associated with in-house billing staff and infrastructure, practices often achieve significant cost savings.
- Access to Expertise: You gain access to a team of certified, 100% US-based podiatry coding and billing experts who live and breathe podiatry RCM. We have specialized experience with practices in New Jersey, Nevada, Nebraska, North Carolina, and Kentucky.
- Reduced Administrative Burden: We handle the complexities of billing, allowing your staff to focus on clinical tasks and patient care.
- Maximized Reimbursements: Our dedicated, podiatry-specific expertise ensures accurate claim submissions, aggressive denial management, and identification of all billable services, maximizing your collections.
- Scalability: Our services scale with your practice, whether you’re a solo practitioner, part of a group, or affiliated with a hospital.
We are not just another billing company; we are your strategic partner, committed to maximizing your collections and streamlining your operations. Many practices see at least a 10% increase in profitability within the first six months of partnering with us. To explore your options, read 5 Proven Ways to Find a Podiatry Billing Company.
Measuring What Matters: KPIs and Denial Management for Financial Health
You wouldn’t treat a patient without monitoring their vital signs, and the same principle applies to your practice’s financial health. Measuring key performance indicators (KPIs) and having a robust denial management strategy are crucial for effective revenue cycle management podiatry.
Critical KPIs for Effective Revenue Cycle Management Podiatry
KPIs are your practice’s financial pulse. By regularly tracking these metrics, we can identify strengths, pinpoint weaknesses, and make informed decisions to improve your revenue cycle.
Here are some critical KPIs we monitor:
- Days in A/R (Accounts Receivable): This measures the average number of days it takes to collect payments. Most practices should aim for under 50 days. If your days in A/R are consistently above this, it signals a bottleneck in your RCM process.
- Clean Claim Rate (CCR): The percentage of claims submitted that are paid on the first submission. A high CCR (aim for 95%+) indicates efficient front-end processes and accurate coding.
- Denial Rate: The percentage of claims denied by payers. Our goal is to keep this below 8%, and ideally, below 4% for rejections.
- Net Collection Rate: This shows how much of your collectible revenue you actually collect. A healthy rate is typically above 95%.
- Cost to Collect: The expense incurred to collect $1 of revenue. Lower is always better.
We provide regular reports on these and other metrics, offering clear insights into your financial performance. This data-driven approach allows us to benchmark your practice against national standards and continuously optimize your RCM processes. We help you understand these numbers and what they mean for your practice’s growth. For more on financial health, visit Financial Health KPIs and for a deeper dive into KPIs, check out Live and Die by KPIs: The Podiatrist’s Guide to Practice Growth and Profitability.
Building a Winning Denial Management Strategy
Even with the best preventive measures, denials happen. The key is how you respond. A winning denial management strategy isn’t just about appealing individual claims; it’s about identifying trends and implementing systemic changes to prevent future denials.
We conduct thorough root cause analysis to understand why claims are being denied. Is it a specific payer? A particular code? A documentation oversight? Once identified, we appeal wrongfully denied claims with robust supporting documentation. 50-60% of all denials are never worked to adjudication, meaning that revenue is permanently lost. Our dedicated team ensures claims are corrected and resubmitted promptly, often recovering revenue that would otherwise be abandoned. We also use this information to update your practice’s processes and provide ongoing staff training, turning denials into learning opportunities. Staying compliant with regulations is also key, as discussed in Compliance & Legal.
Conclusion: Take the Next Step Toward a Healthier Revenue Cycle
The journey from patient foot traffic to a healthy cash flow in your podiatry practice is paved with complexities, but it doesn’t have to be a painful one. Effective revenue cycle management podiatry is the backbone of a thriving practice, ensuring that your dedication to patient care is met with robust financial returns.
We’ve explored the unique challenges of podiatry coding, the intricacies of payer policies, and the critical steps involved in the RCM process. We’ve highlighted how implementing best practices, leveraging modern technology, and choosing the right strategic partner can transform your financial landscape. RCM is not a static process; it requires continuous monitoring, adaptation, and specialized expertise.
By partnering with us, Guide Podiatric Billing Services, you gain a dedicated, 100% US-based team of podiatry RCM experts. We are committed to maximizing your collections, streamlining your operations, and allowing you to focus on what you do best: providing exceptional foot and ankle care to your patients across New Jersey, Nevada, Nebraska, North Carolina, and Kentucky.
Don’t let revenue leakage, claim denials, or administrative burdens hinder your practice’s growth. Take the next step towards a healthier, more profitable future. Contact Beacon to optimize your podiatry billing services today.