The Best Personalized Podiatry Revenue Management Strategies for 2026
Why Personalized Podiatry Revenue Management Is the Key to Practice Profitability in 2026
Personalized podiatry revenue management is a tailored approach to optimizing every step of your practice’s billing cycle — from patient intake to final payment — based on your specific payer mix, sub-specialties, and patient demographics.
Here’s a quick look at what it involves and why it matters:
- Customized billing workflows built around your practice type (solo, group, or multi-location)
- Sub-specialty coding expertise for diabetic foot care, DME/orthotics, wound care, and podiatric surgery
- Proactive denial management to recover lost revenue and prevent future leakage
- Data-driven analytics to spot missed billable services and payer-specific patterns
- Transparent patient financial services to improve collections and satisfaction
Nearly 25% of podiatry practices struggle to maintain financial stability due to inefficient revenue management. And it’s no mystery why — podiatry billing sits at a complicated crossroads of office-based care, minor surgery, and durable medical equipment (DME) rules. Miss one modifier, skip a systemic diagnosis, or misbill an orthotics code, and you’re looking at denied claims, delayed payments, or even audit risk.
The problem runs deep. Industry data shows podiatry practices can lose 25–40% of potential revenue to insurance adjustments and denials. Solo practitioners are hit hardest — median net income dropped to just $106,750 in 2020, while group practices earned nearly $35,000 more on average.
The good news? Practices that shift to a personalized, specialized RCM approach consistently see dramatic improvements — often a 20–30% increase in monthly revenue — simply by tightening up documentation, coding accuracy, and denial workflows.
This guide walks you through exactly how to do that in 2026.
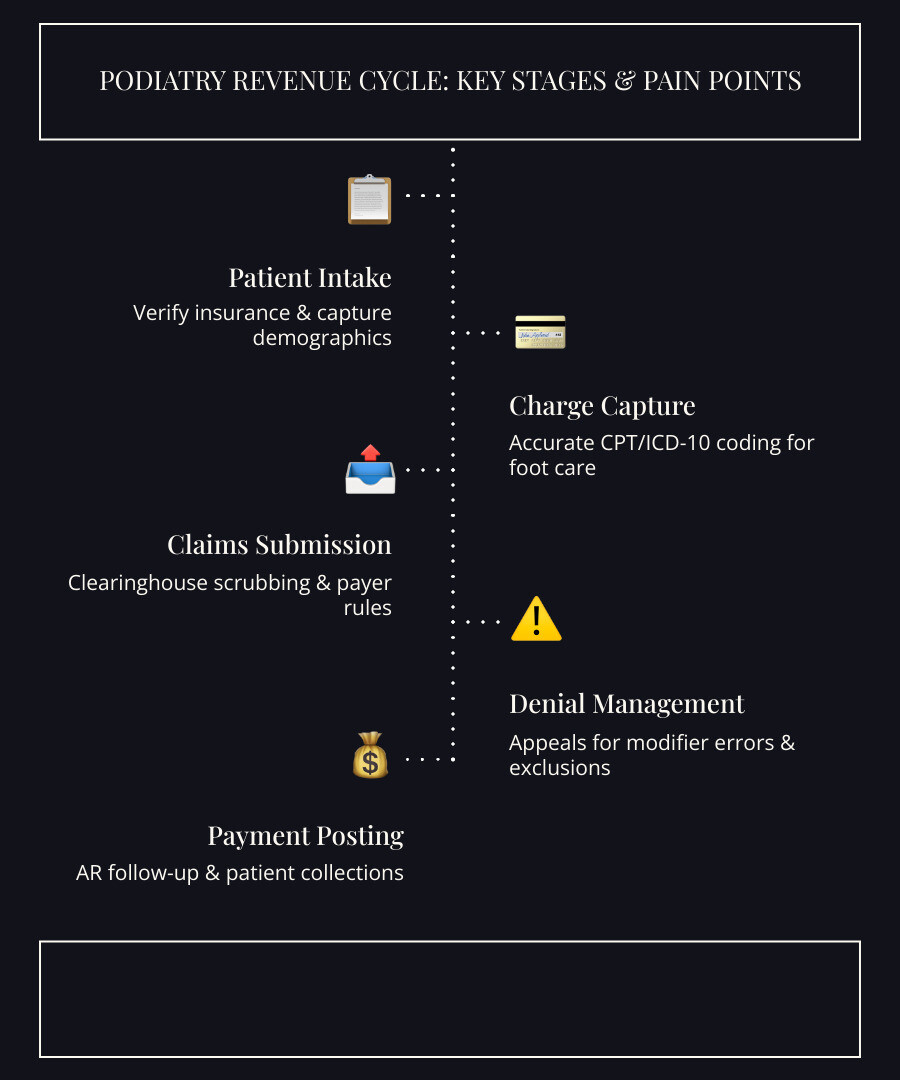
Defining Personalized Podiatry Revenue Management in 2026
In the past, medical billing was often treated as a “one-size-fits-all” administrative task. You saw a patient, picked a code, and hoped for the best. In 2026, that approach is a recipe for financial disaster. Personalized podiatry revenue management represents a shift toward precision. It acknowledges that a sports medicine clinic in Charlotte has different billing needs than a geriatric-focused practice in Jersey City.

Traditional RCM focuses on high-volume processing, which often leads to “knowledge atrophy” where specific podiatry nuances are ignored. Personalized RCM, however, builds workflows around your specific sub-specialties. Whether you focus on limb salvage, pediatric podiatry, or elective forefoot surgery, your revenue cycle should reflect the specific documentation requirements and payer rules of those fields. By utilizing smart financial management, we can align your billing engine with your clinical strengths.
Assessing Current Revenue Cycle Pain Points
To fix your revenue, you first have to find where it’s leaking. Common pain points we see in podiatry include:
- Claim Denials: Often caused by missing “class findings” for routine foot care or incorrect modifier usage (like -59, -RT, or -LT).
- AR Delays: When claims sit in “pending” status for over 60 days because of simple front-desk errors or lack of prior authorization.
- Administrative Burden: Your front desk staff shouldn’t be “chasing” claims; they should be focused on the patient in front of them.
- Collection Rates: The average podiatrist collects only about 56% of their listed fees. In a personalized model, we aim for a 95%+ first-pass clean claim rate to close that gap.
The Shift from Volume to Value-Based Care
The healthcare landscape is moving away from just “seeing more feet” to providing better outcomes. This shift toward value-based care means podiatrists are now viewed as essential care coordinators, especially for diabetic patients. Proper revenue management ensures that your role in preventing hospitalizations and amputations is financially recognized through quality metrics and chronic disease management codes.
Overcoming Unique Podiatric Billing Challenges
Podiatry is unique because it blends primary care, surgery, and retail-like DME. This creates a “perfect storm” for billing errors. For example, a simple nail debridement can be considered “cosmetic” (non-covered) unless the patient has a documented systemic condition like peripheral vascular disease.
Recent podiatry billing analysis shows that the most frequent denials stem from failing to link the correct diagnosis to the procedure. If you aren’t using “class finding” modifiers correctly, you are essentially providing free care. Furthermore, surgical coding complexities—such as bundling rules for bunionectomies or hammertoe corrections—require a deep understanding of the Global Surgical Period to avoid “double-dipping” denials or missed post-op revenue.
Personalized Podiatry Revenue Management for DME and Orthotics
Durable Medical Equipment (DME) is a massive revenue opportunity that many practices leave on the table because of the paperwork. Coding for the L3000 series (custom orthotics) or A5513 (diabetic shoes) requires strict adherence to DMEPOS standards.
To maximize high-profit procedures, your documentation must prove medical necessity before the item is even dispensed. This includes detailed biomechanical exams and gait analyses. When managed correctly, DME reimbursements alone can often cover the entire cost of your RCM services.
Advanced Wound Care and Surgical Reimbursement
Wound care is a high-risk, high-reward area. With the rise of skin substitutes and biologic products, the audit risk has increased significantly. Implementing Clinical Documentation Improvement (CDI) ensures that every debridement and graft application is backed by specific measurements and progress notes. Using minimally invasive procedures and regenerative medicine requires a personalized strategy to ensure these cutting-edge treatments are actually reimbursed by payers who are often slow to update their policies.
Leveraging AI and Data Analytics for Practice Growth
By 2026, AI is no longer a futuristic concept; it is a fundamental tool for personalized podiatry revenue management. AI-driven software can “scrub” claims with a level of detail humans might miss, flagging high-risk code combinations before they ever reach the payer.
Predictive analytics allow us to look at “payer behavior.” If a specific insurance company in Nebraska suddenly starts denying all fungal nail claims, AI spots that pattern in real-time, allowing us to adjust your documentation templates immediately. Additionally, voice-to-text transcription tools are helping DPMs reduce their charting time by half, converting spoken clinical observations into structured, billable data. This AI integration ensures that no billable service is forgotten during a busy clinic day.
Tailoring Personalized Podiatry Revenue Management with Predictive AI
Predictive AI helps us manage your “financial health” by analyzing denial patterns. Instead of reactively fixing a rejected claim, we use data to proactively change the workflow. Tracking your KPIs—such as your net collection rate and days in AR—allows us to see exactly where the bottlenecks are. If your AR over 90 days is creeping up, the data tells us exactly which payer or which staff member’s documentation needs attention.
Enhancing Patient Financial Services
In an era of high-deductible plans, the patient is often your “second-largest payer.” Transparency is key. Personalized RCM includes:
- Clear Value Propositions: Explaining why a specific treatment is necessary, even if it’s a cash-pay service.
- Credit Card on File: Streamlining the collection of co-pays and balances.
- US-Based Call Centers: Ensuring that when your patients have a billing question, they speak to someone who understands their care and can provide a warm, professional experience. Effective patient communication reduces friction and increases the likelihood of full payment.
Strategic Revenue Maximization for Solo and Group Practices
The strategies for a solo practitioner in Ashland, Kentucky, differ greatly from a large group practice in Las Vegas. Solo practices often struggle with high overhead (sometimes as high as 32% of revenue) because they lack the “economy of scale.”
| Metric | Solo Practice (Average) | Group Practice (Average) |
|---|---|---|
| Median Net Income | $106,750 | $141,500 |
| Admin Overhead % | 30-35% | 20-25% |
| Collection Rate | 60-70% | 85-95% |
| Revenue Leakage | 25-40% | 10-15% |
For solo DPMs, the goal is often to reduce the administrative burden so they can focus on high-value patients. For group practices, the focus is on revenue maximization strategies across multiple providers, ensuring consistency in coding and centralized billing efficiency.
Uncovering Hidden Revenue Opportunities
Many practices are sitting on a goldmine of uncollected revenue. This includes:
- Lost Claim Recovery: Identifying claims that were “scrubbed” but never actually reached the payer.
- Missed Billable Services: Often, DPMs perform biomechanical exams or specific imaging that they forget to bill.
- Ancillary Services: Integrating pathology, vascular testing, or therapeutic shoes can keep revenue in-house that you would otherwise refer out. By conducting a profit potential audit, we can often find thousands of dollars in “hidden” revenue from the past six months alone.
Scaling Operations Through Specialized Outsourcing
Outsourcing to a general medical billing company is a mistake. They don’t know what a “bunionectomy with osteotomy” entails versus a “simple exostectomy.” Specialized outsourcing gives you access to certified podiatry coders who understand the anatomy of the foot. This leads to a higher first-pass claim rate and significantly reduced administrative costs, allowing your practice to scale without hiring more office staff.
Frequently Asked Questions about Podiatry RCM
What are the most important KPIs for podiatry practices?
You should live and die by your KPIs. The “Big Four” are:
- Net Collection Rate: (Target 95%+) This shows how much of the money you are legally owed you actually collected.
- Days in AR: (Target <35 days) This measures how long it takes for a dollar to hit your bank account after a patient is seen.
- Denial Rate: (Target <5%) High denial rates indicate a problem with either front-desk data entry or back-end coding.
- Average Revenue per Visit: This helps you identify if you are seeing too many low-value “routine care” patients and not enough high-value surgical or DME cases.
How does personalized RCM differ from standard medical billing?
Standard billing is reactive—it processes what you give it. Personalized RCM is proactive. It involves customized workflow training for your staff, payer-specific podiatry rule sets (like knowing which New Jersey payers require specific modifiers), and tailored reporting that gives you a “bird’s eye view” of your practice’s financial health.
Can a hybrid cash-pay model work for a solo practitioner?
Absolutely. In fact, it’s often the “escape hatch” for solo DPMs feeling trapped by low insurance reimbursements. By keeping only the best-paying insurance contracts and adding cash-pay services like laser therapy, regenerative medicine, or high-end custom orthotics, you can see 40% fewer patients while increasing your net revenue by 30-40%.
This model reduces administrative overhead from 32% down to as low as 8%, as you spend less time chasing $15 co-pays and more time delivering high-value care.
Conclusion
The “practice prison” of high-volume, low-reimbursement care is a choice, not a necessity. By implementing personalized podiatry revenue management, you can transform your practice from a source of stress into a thriving, profitable business.
At Beacon Podiatric Billing Services, we specialize in exactly this. Our 100% US-based team of experts understands the nuances of podiatric coding and the specific payer landscapes in New Jersey, Nevada, Nebraska, North Carolina, and Kentucky. Whether you are a solo practitioner looking to reclaim your time or a group practice aiming to scale, our personalized RCM strategies are proven to increase revenue by 10–30% within the first few months.
Don’t let your hard work walk out the door in the form of denied claims and unbilled services. Maximize your collections with Beacon Podiatric Billing Services and get back to what you do best: keeping your patients on their feet.