Podiatry revenue cycle management: Master 20% Growth
Why Your Practice’s Financial Health Starts with RCM
Podiatry revenue cycle management (RCM) is the complete process of managing your practice’s revenue from the moment a patient schedules an appointment to the final payment collection. It encompasses everything from insurance verification and accurate coding to claim submission, denial management, and patient billing.
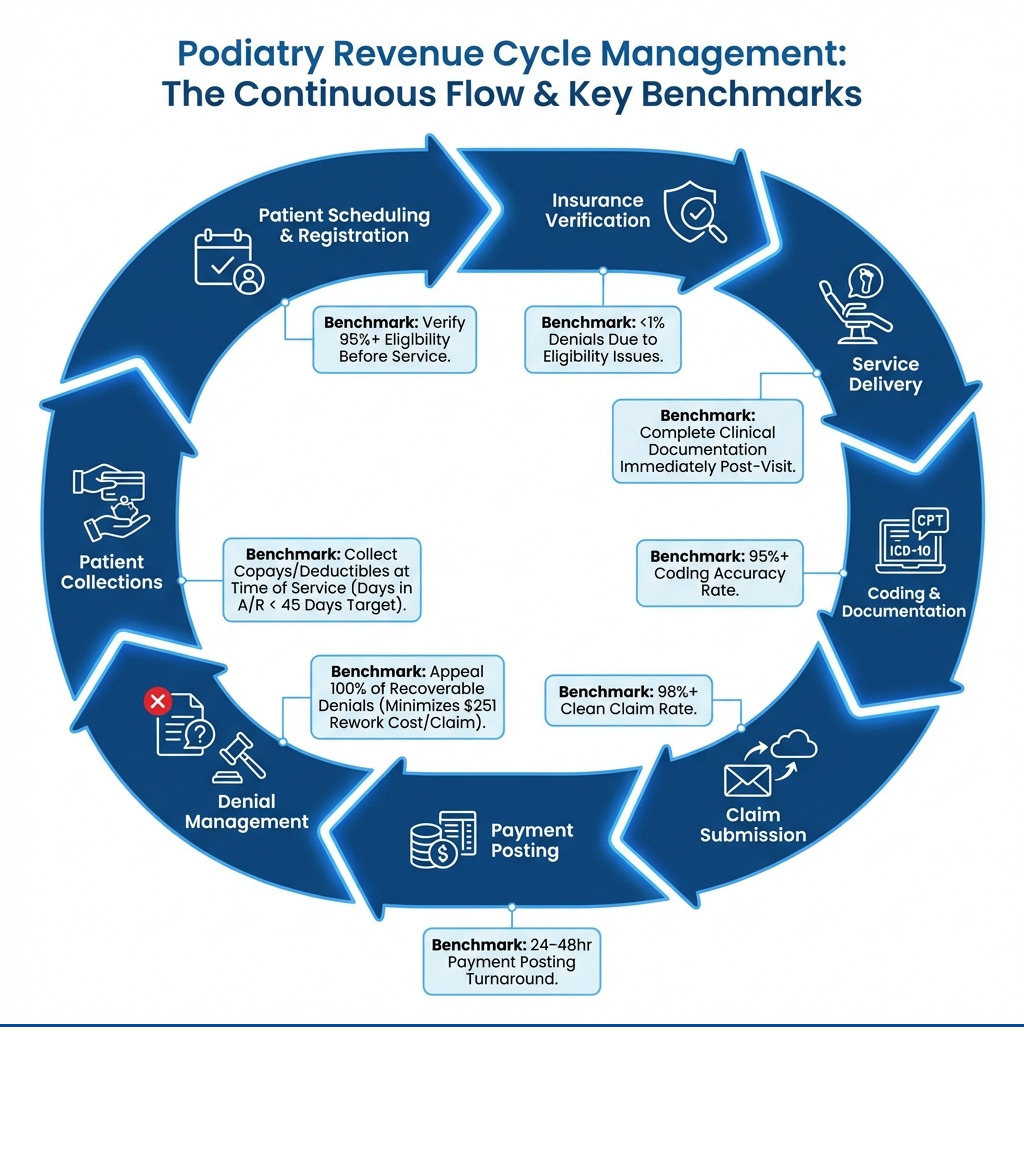
Here’s what effective podiatry RCM includes:
- Patient registration and insurance verification – Confirming coverage before services are rendered
- Documentation and coding – Using accurate CPT and ICD-10 codes specific to podiatry procedures
- Claim submission – Scrubbing and submitting clean claims electronically
- Payment posting – Recording all payments and reconciling EOBs
- Denial management – Identifying, appealing, and preventing claim denials
- Patient collections – Managing copays, deductibles, and outstanding balances
- Performance tracking – Monitoring KPIs like days in A/R and clean claim rates
If you’re a podiatrist, you already know that running a successful practice requires more than clinical expertise. You need to steer complex coding rules, understand payer-specific requirements, and ensure you actually get paid for the care you provide.
The reality is sobering. One-third of insurance denials are due to eligibility issues – a highly preventable problem. Even worse, 50-60% of all denials are never worked to adjudication, which means practices are essentially writing off revenue they’ve already earned. And every time you need to rework and resubmit a claim, it costs your practice an average of $251.
As one podiatrist put it: “I didn’t realize what we were missing out on” after switching to a specialized billing service that understood the unique challenges of podiatry RCM.
The good news? With the right processes, technology, and expertise, you can dramatically improve your collections, reduce administrative burden, and get back to what you do best – caring for patients.
Relevant articles related to Podiatry revenue cycle management:
The Core Components of Podiatry Revenue Cycle Management
Podiatry revenue cycle management is a complex, multi-stage process that begins long before a patient even steps into your office and continues long after they’ve left. To master your practice’s financial health, it’s crucial to understand each primary component and how they interact. Think of it as a carefully choreographed dance, where every step must be executed precisely for a flawless performance.

Step 1: Patient Pre-Registration and Insurance Verification
The journey of podiatry revenue cycle management often starts with patient pre-registration. This initial phase involves gathering essential patient demographics and, critically, performing thorough eligibility and benefits verification. Why is this so important? Because, as statistics show, one-third of insurance denials are due to eligibility issues. This is a highly preventable problem that can lead to significant lost revenue and administrative headaches down the line.
During pre-registration, our team ensures we capture accurate patient information, including their name, address, and date of birth. We then verify their insurance coverage, confirm their plan’s benefits, and determine if any prior authorizations are required for scheduled procedures. This proactive approach helps identify potential out-of-network alerts or coverage gaps before services are rendered, allowing us to communicate financial expectations with patients upfront. It’s much easier to discuss a patient’s responsibility before treatment than after! By laying this groundwork diligently, we prevent denials and ensure a smoother payment process. For more insights on optimizing your practice’s operations, explore our resources on practice management.
Step 2: Accurate Documentation, Coding, and Charge Capture
Once a patient is seen, the next critical step in podiatry revenue cycle management involves meticulous documentation, precise coding, and accurate charge capture. This is where clinical care translates into billable services. Podiatry billing is notoriously nuanced, requiring specialized expertise in CPT (Current Procedural Terminology) and ICD-10 (International Classification of Diseases, 10th Revision) codes.
For example, podiatry involves specific codes for routine foot care, wound care, diabetic exams, orthotics, and various minor surgical procedures. Furthermore, understanding the correct application of modifiers, such as -Q7, -Q8, and -Q9 for at-risk patients, is paramount. Incorrect or missing modifiers can lead to immediate claim rejections or denials.
The concept of “medical necessity” is also central here. While you, as a physician, evaluate the need for care, insurance companies have their own criteria. Therefore, your clinical notes must clearly and comprehensively demonstrate medical necessity to meet insurer requirements. Detailed and customized templates in your EHR can be invaluable for ensuring chart note accuracy and consistency. Our team stays updated on the latest coding standards and regulatory changes to ensure every service you provide is accurately represented and billed. For the latest updates, check out our coding updates.
Step 3: Claims Submission and Processing
After accurate documentation and coding, the charges are compiled, and claims are prepared for submission. This stage focuses on achieving a high “clean claim rate,” meaning claims are submitted correctly the first time, minimizing rejections and denials. Our process involves thorough “claim scrubbing” using advanced tools to identify and correct any errors—like missing information, incorrect codes, or modifier issues—before the claim even leaves your practice. This proactive step is crucial because simple demographic errors or missing diagnosis codes can cause immediate rejections by the clearinghouse.
We then electronically submit these scrubbed claims to the appropriate payers. Timely filing limits are a strict reality in medical billing; missing these deadlines means lost revenue, pure and simple. Our efficient systems ensure claims are submitted promptly, often within 24-48 hours of service, well within these critical windows. By focusing on precision from the outset, we significantly reduce the time elapsed between the patient encounter and claim submission, ensuring a smoother journey towards reimbursement. For reliable podiatry billing services that prioritize clean claim submission, consider partnering with us.
Step 4: Payment Posting, Denial Management, and Appeals
Once claims are submitted, we move into the crucial phase of payment posting, denial management, and, when necessary, appeals. Payment posting involves accurately recording payments received from payers and patients, then reconciling these against the original charges and Explanation of Benefits (EOBs). This ensures your accounts receivable (A/R) are always current and accurate.
However, not all claims sail through smoothly. Denials are an unfortunate reality, and this is where robust denial management becomes your practice’s financial superhero. Our dedicated team reviews each denied claim to identify the exact reason for the denial. Was it a coding error? Lack of medical necessity? Eligibility issue? Once identified, we correct any errors and resubmit the claim. If necessary, we carefully handle the appeals process, fighting for every dollar your practice is owed. It’s a battle worth fighting, especially when you consider that 50-60% of all denials are never worked to adjudication, effectively becoming lost revenue. Moreover, each time you need to re-work and redo a claim, it costs your practice an average of $251. We work tirelessly to prevent underpayments and ensure your practice receives the maximum reimbursement it deserves.
Navigating the Top Challenges in Podiatry Billing
Even with a solid understanding of the RCM components, podiatry practices face unique and persistent challenges that can significantly impact their financial health. It’s like navigating a maze with constantly shifting walls – tricky, to say the least!

The Challenge of Complex Coding and Payer-Specific Rules
Podiatry is a specialty with its own intricate coding landscape. Nuanced procedures, from routine foot care to complex surgical interventions, each require precise CPT and ICD-10 codes. The frequent use of modifiers, such as the -Q7, -Q8, and -Q9 modifiers for at-risk patients, adds another layer of complexity. Incorrect application of these can lead to immediate claim rejections or denials.
Beyond this, we must contend with “bundling and unbundling” of services, where certain procedures performed together may or may not be separately reimbursable, leading to potential underpayments or compliance risks. A major hurdle is understanding and adhering to payer-specific rules and Local Coverage Determinations (LCDs), especially from Medicare. These policies, which can vary by region (such as in New Jersey, Nevada, Nebraska, North Carolina, or Kentucky), outline specific documentation requirements and medical necessity criteria for covered services. Staying current with these changing payer policies is a full-time job in itself. For comprehensive guidance on Medicare billing, refer to our Medicare Podiatry Billing Guidelines. To ensure your practice remains compliant and avoids audits, we also recommend our guide on audit-proofing your practice.
The Challenge of Denial Management and A/R Follow-Up
Denial management is arguably one of the most significant pain points in podiatry revenue cycle management. High denial rates cripple cash flow and create a mountain of administrative work. As we’ve seen, denial rates in general should be below 8%, but many practices struggle to meet this benchmark. The challenge isn’t just about appealing a denial; it’s about conducting a thorough root cause analysis to understand why claims are being denied and implementing strategies to prevent future occurrences.
Unfortunately, a common issue is the lack of consistent follow-up on denied claims. With 50-60% of all denials never worked to adjudication, practices are leaving substantial revenue on the table. This neglect directly contributes to aging accounts receivable (A/R), where payments become harder to collect the older they get. The longer a claim remains unpaid, the less likely it is to be fully recovered. Our proactive approach to denial management ensures that every denied claim is addressed promptly, diligently, and with an eye toward maximizing your practice’s reimbursement. Our specialized services are designed to tackle these challenges head-on; learn more about our denial management solutions.
The Challenge of Patient Collections and Financial Transparency
While insurance companies are a major payer, patient collections form another vital, yet often challenging, part of podiatry revenue cycle management. With the rise of high-deductible health plans, patients are shouldering a greater portion of their healthcare costs. This makes transparent communication about patient responsibility-including copays, deductibles, and co-insurance-absolutely essential from the very first interaction.
Many practices struggle to effectively communicate financial expectations, leading to an increase in outstanding patient balances. Our strategy involves clearly conveying payment policies and providing patient-friendly billing statements. We also leverage modern solutions like online payment options and interactive balance-due reminder texting to make it easier for patients to pay. Some practices even implement solutions like “Flexpay,” allowing patients to pay over time while the provider collects immediately. By being upfront and offering convenient payment methods, we help reduce outstanding balances and improve patient satisfaction, ensuring they understand their financial obligations without feeling overwhelmed.
In-House vs. Specialized RCM Services: Making the Right Choice
When it comes to managing your practice’s podiatry revenue cycle management, you essentially have two main paths: handling it in-house or partnering with a specialized RCM service. Both have their merits, and the best choice often depends on your practice’s size, resources, and specific needs. It’s a bit like deciding whether to cook a gourmet meal yourself or hire a professional chef – both can get the job done, but the experience and outcome might differ!
| Feature | In-House Billing | Outsourced RCM Services |
|---|---|---|
| Cost | Salaries, benefits, training, software, infrastructure | Percentage of collections, predictable fee structure |
| Expertise | Dependent on staff knowledge, ongoing training required | Access to certified specialists, up-to-date knowledge |
| Efficiency | Can be high with well-trained staff, but prone to errors | Streamlined processes, advanced technology, high accuracy |
| Control | Direct oversight of all processes | Less direct daily control, but strong reporting & communication |
| Scalability | Challenging to scale with practice growth | Easily scalable, adapts to practice volume fluctuations |
If you’re weighing your options, our guide on 5 Proven Ways to Find a Podiatry Billing Company can offer further insights.
Benefits of In-House Podiatry Revenue Cycle Management
Maintaining an in-house billing department offers several advantages, particularly for larger, well-established practices with dedicated resources. One of the primary benefits is direct control over every aspect of your podiatry revenue cycle management. You have immediate access to your billing staff, can oversee their daily activities, and directly manage specific cases or patient inquiries.
An integrated staff can foster strong internal communication between clinical and administrative teams, potentially leading to faster resolution of documentation issues. For some practices, the direct cost of an in-house team might appear lower on paper, especially if they have existing infrastructure and a stable, experienced billing team. It also allows for immediate access to billing information and reports, which can be beneficial for real-time decision-making.
Benefits of Outsourcing Your Podiatry Revenue Cycle Management
For many podiatry practices, especially those aiming to maximize collections and streamline operations without the heavy administrative burden, outsourcing podiatry revenue cycle management to a specialized service is a game-changer.
The most significant benefit is accessing specialized expertise. Our team comprises 100% US-based, AAPC-certified billers who possess deep knowledge of podiatry-specific coding, modifiers, and payer rules. This specialized focus often translates to improved collections and a higher clean claim rate.
Outsourcing also significantly reduces your administrative burden. You no longer need to worry about hiring, training, and retaining billing staff, managing software licenses, or keeping up with ever-changing regulations. This frees up your in-house team to focus on patient care and other critical practice operations. The cost savings can be substantial, as you eliminate salaries, benefits, and the overhead associated with an in-house department, often replacing it with a predictable fee structure based on collections.
Furthermore, outsourced RCM services offer scalability, adapting seamlessly to your practice’s growth or fluctuations in patient volume. We bring advanced technology, detailed claims scrubbing, and automated denial management processes that might be cost-prohibitive for individual practices. By partnering with us, you gain a dedicated team focused solely on optimizing your revenue cycle, ensuring you get paid accurately and on time, allowing you to practice with confidence. Find how our outsourced RCM services can transform your practice’s financial health.
Measuring Success: The KPIs That Define a Healthy Revenue Cycle
In podiatry revenue cycle management, what gets measured gets managed. Without tracking key performance indicators (KPIs), you’re essentially flying blind, unable to identify bottlenecks, inefficiencies, or areas for improvement. Regular financial benchmarking and performance tracking are crucial for making data-driven decisions that ensure the long-term health and profitability of your practice. It’s like a doctor monitoring a patient’s vital signs – you need to know what’s healthy and what needs attention!
For a deeper dive into the importance of tracking these metrics, check out our guide, Live and Die by KPIs: The Podiatrist’s Guide to Practice Growth and Profitability.
Key Performance Indicators for Podiatrists
To effectively monitor your podiatry revenue cycle management, we recommend focusing on these essential KPIs:
- Days in A/R (Accounts Receivable): This measures the average number of days it takes for your practice to get paid after a service is rendered. A lower number indicates a more efficient billing process. Most practices should fall below 50 days to get a claim paid. If your days in A/R are consistently higher, it signals a potential bottleneck in your RCM.
- Clean Claim Rate: This KPI represents the percentage of claims that are paid on their first submission, without requiring any corrections or resubmissions. A high clean claim rate is a hallmark of an efficient RCM process. Claim rejection rates should normally be lower than 4%.
- Denial Rate: This tracks the percentage of claims that are denied by payers. A high denial rate directly impacts your cash flow and increases administrative costs. Denial rates in general should be below 8%. 50-60% of all denials are never worked to adjudication, representing significant lost revenue.
- Net Collection Rate: This is the ultimate measure of your billing department’s effectiveness, showing the percentage of collectible revenue your practice actually collects. It reflects how well your RCM process turns billed services into actual cash.
- A/R Over 120 Days: This metric focuses on the portion of your accounts receivable that is more than 120 days old. The older a claim gets, the harder it is to collect. National benchmarks for A/R aging suggest that less than 18% of your A/R should be over 120 days old. A high percentage here indicates serious issues with follow-up and denial management.
By regularly reviewing these KPIs, you gain clear insights into your practice’s financial performance, allowing you to identify weaknesses and implement targeted strategies for improvement. For more detailed insights into managing your practice’s financial health, explore our articles on Financial Health KPIs.
The Future of RCM: Technology and Evolving Regulations
The landscape of podiatry revenue cycle management is constantly evolving, driven by rapid advancements in technology and a steady stream of new healthcare regulations. Staying ahead of these changes isn’t just about compliance; it’s about leveraging new tools to improve efficiency, accuracy, and ultimately, your practice’s bottom line.
How Technology is Enhancing Podiatry RCM
Technology is revolutionizing how we approach podiatry revenue cycle management. Artificial intelligence (AI) and specialized software are no longer futuristic concepts; they are practical tools enhancing various RCM functions.
Here’s how technology is making a difference:
- AI-Powered Coding and Documentation: AI can assist with natural language data capture in EHRs, suggesting appropriate codes based on clinical notes and even identifying potential coding errors before submission. This reduces manual effort and improves accuracy.
- Automated Eligibility Checks: Advanced systems can perform eligibility verification multiple times, including proactive, pre-submission alerts for claims likely to be denied due to eligibility issues. Some even provide out-of-network alerts during scheduling.
- Advanced Analytics Software: Sophisticated dashboards and reporting tools offer real-time insights into KPIs, helping identify trends, bottlenecks, and areas for improvement.
- Patient Payment Portals and Mobile Options: Technology streamlines patient collections through online payment portals, balance-due texting, and the ability for patients to pay from any mobile device. This improves patient satisfaction and speeds up collections.
- EHR Integration: Seamless integration between your Electronic Health Record (EHR) system and RCM software is paramount. This ensures that clinical documentation directly supports billing, reducing errors and streamlining workflows. If you’re transitioning EHR systems, our team can help you steer this complex process; explore our resources on navigating your EHR transition.
These technological advancements automate tedious tasks, provide proactive alerts, and offer invaluable data, allowing your team to focus on more complex RCM challenges and patient care. For more information on leveraging technology in your practice, visit our Technology in Podiatry section.
Staying Ahead of Evolving Healthcare Regulations
The regulatory environment in healthcare is a dynamic beast, with new rules and updates frequently impacting podiatry revenue cycle management. Staying compliant is not optional; avoid penalties, audits, and legal complications.
Key regulatory considerations include:
- CMS Initiatives: The Centers for Medicare & Medicaid Services (CMS) frequently introduces new initiatives, such as those related to Value-Based Care and MIPS (Merit-based Incentive Payment System), which can significantly affect reimbursement models and reporting requirements.
- The Cures Act: This legislation promotes interoperability and patient access to their health information, impacting how EHRs connect with patients and other healthcare entities.
- No Surprises Act: This act protects patients from unexpected medical bills, particularly from out-of-network providers, and necessitates changes in how practices communicate costs and obtain consent.
- HIPAA Compliance: Adhering to the Health Insurance Portability and Accountability Act (HIPAA) remains critical for protecting patient data privacy and security.
- Payer Policy Updates: Beyond federal regulations, commercial payers regularly update their policies, coverage criteria, and coding guidelines, requiring constant vigilance.
Our team continuously monitors these evolving regulations and payer policies. We ensure that our processes and your practice remain compliant, helping you steer the complexities of healthcare law and avoid costly mistakes. For ongoing information on compliance and legal issues, refer to our Compliance & Legal resources.
Conclusion: Take Control of Your Practice’s Financial Future
Mastering podiatry revenue cycle management is not merely an administrative task; it’s a strategic imperative for the sustained success and growth of your practice. We’ve explored the intricate components, tackled the common challenges, weighed the benefits of specialized RCM services, and highlighted the crucial KPIs and technological advancements shaping the future.
The takeaway is clear: a proactive, informed, and expertly managed RCM strategy is the bedrock of a financially healthy podiatry practice. It allows you to transform “foot traffic” into consistent “cash flow,” ensuring that your dedication to patient care is appropriately reimbursed. By optimizing your RCM, you reduce administrative burden, minimize denials, accelerate payments, and ultimately, free up valuable time and resources to focus on what truly matters – your patients.
Don’t let the complexities of billing and collections overshadow your passion for podiatric medicine. Take control of your practice’s financial future today. Contact Beacon Podiatric Billing Services to guarantee an increase in your revenue by up to 20%. Let us be your trusted partner in navigating the ever-changing landscape of podiatry revenue cycle management, so you can practice with confidence.