Podiatry Billing Compliance: Boost 2026 Revenue
Why Podiatry Billing Compliance Matters for Your Practice
Podiatry billing compliance isn’t just paperwork—it’s the backbone of your practice’s financial health and your license to operate. Get it wrong, and you face denied claims, costly audits, and potential exclusion from federal programs.
Quick Answer: Key Elements of Podiatry Billing Compliance
- Accurate Documentation – Prove medical necessity for every service, especially routine foot care
- Correct Coding – Use proper CPT, ICD-10, and modifier combinations for all procedures
- Medicare Rules – Understand systemic condition requirements and Class Findings for routine care
- Payer Policies – Verify coverage and obtain prior authorizations before treatment
- Regular Audits – Review your claims proactively to catch errors before payers do
The numbers tell a sobering story. Medicare’s improper payment rate for podiatry care sits at 11.2%, representing $216.9 million in questionable payments. Even more concerning: 76.4% of these errors stem from insufficient documentation alone.
A recent OIG audit found that 49 out of 100 sampled podiatry claims didn’t meet Medicare requirements. The estimated impact? $4.4 million in non-compliant payments from just that sample. For busy podiatrists, these compliance gaps create significant financial risk.
The complexity is immense, involving routine foot care exclusions, systemic condition requirements, class findings, and rules that shift between payers. Miss one detail—like failing to document a patient’s diabetes severity or using the wrong Q modifier—and your claim gets denied.
This guide breaks down everything you need to know about podiatry billing compliance. We’ll walk through the foundation of revenue cycle management, decode Medicare’s routine foot care maze, explain audit triggers and fraud prevention, and show you practical strategies to protect your practice while maximizing legitimate reimbursement.
The Foundation: Core Components and Unique Challenges in Podiatry Billing
At its heart, podiatry billing compliance is about managing the financial journey of every patient visit, from scheduling to final payment. This process, known as Revenue Cycle Management (RCM), has unique twists for podiatry.
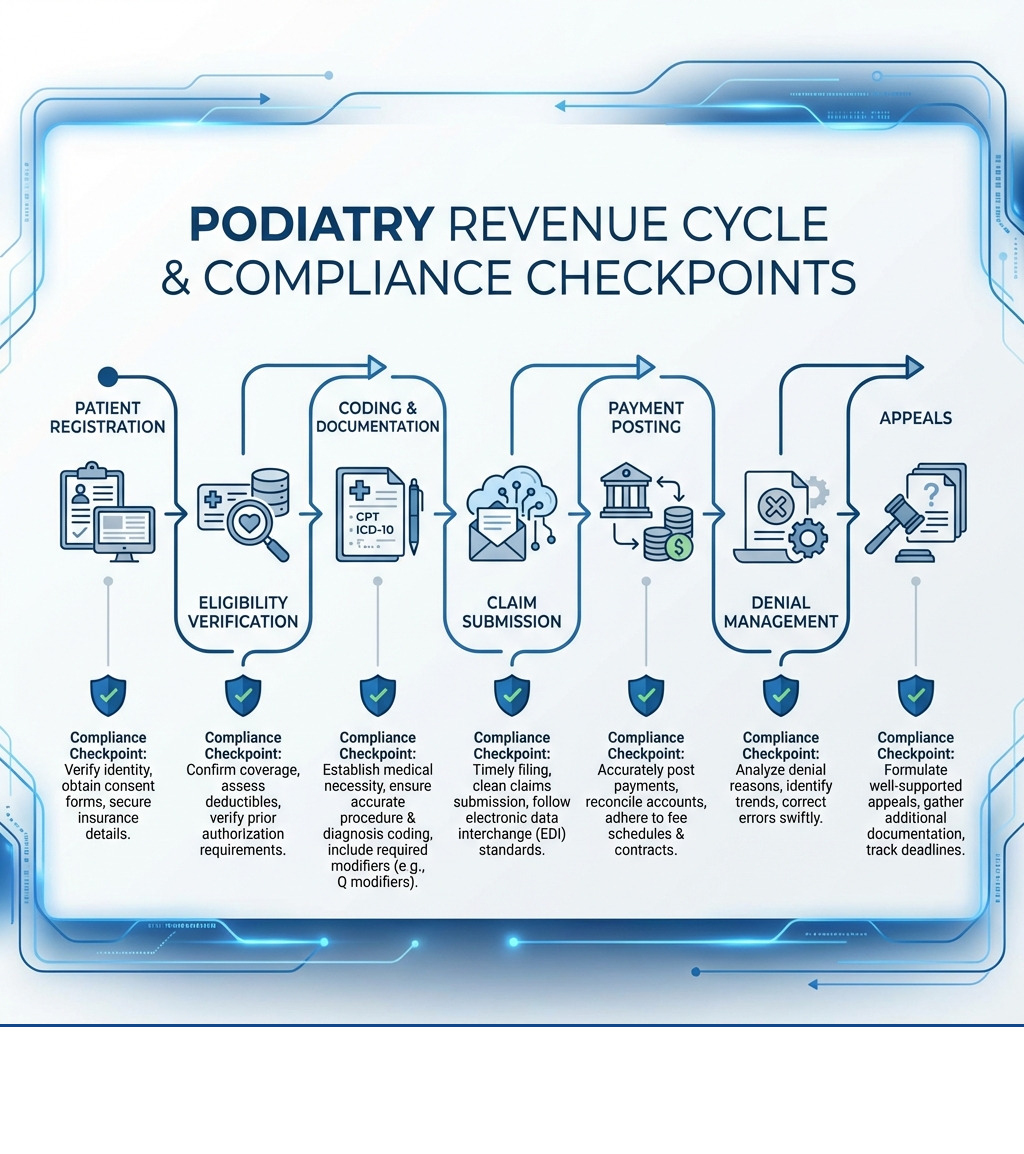
The fundamental components of podiatry billing and RCM include:
- Patient Registration and Eligibility Verification: Accurately capturing patient information and confirming insurance eligibility before services are rendered. This step is crucial for preventing future denials due to inactive coverage or incorrect patient data.
- Coding and Documentation: Translating the services provided and diagnoses made into standardized codes (CPT for procedures, ICD-10 for diagnoses). This requires meticulous documentation to support the medical necessity of every service.
- Claim Submission: Electronically sending claims to insurance companies, Medicare, or Medicaid, adhering to specific submission deadlines and payer-specific requirements.
- Payment Posting: Accurately recording payments received from payers and patients to their respective accounts.
- Denial Management: Investigating rejected claims, understanding the reasons for denial, appealing when necessary, and implementing corrective measures to prevent similar denials in the future.
While these steps are universal in healthcare, podiatry faces distinct challenges that often make this footwork (pun intended!) more complex. These include:
- Routine Care Exclusions: Medicare and many commercial payers generally do not cover “routine foot care” unless specific medical criteria are met, often related to systemic conditions. This requires careful navigation and precise documentation.
- Complex CPT Codes: Podiatry involves a wide array of procedures, from nail debridement to complex surgeries and orthotic fittings, each with specific coding guidelines and potential modifiers.
- ICD-10 Specificity: Diagnoses related to the foot and ankle often require highly specific ICD-10 codes, including laterality, to accurately reflect the patient’s condition.
- Orthotics Billing: Billing for durable medical equipment (DME) like orthotics comes with its own set of rules, including medical necessity, documentation, and prior authorization requirements.
- Surgical Procedure Coding: Surgical procedures, especially those involving the foot and ankle, demand expert coding to capture the full scope of the service while avoiding unbundling or upcoding.
Why Accurate Podiatry Billing is Non-Negotiable
Accurate podiatry billing is a multi-faceted imperative for your practice’s long-term success.
- Financial Health: Accurate billing ensures timely reimbursement for your services, protecting cash flow and your practice’s financial viability. Efficient revenue cycle management is the engine that powers a thriving practice.
- Regulatory Adherence: Adhering to the myriad rules from CMS, state Medicaid programs, and commercial payers is paramount. Incorrect billing can lead to severe penalties, fines, and exclusion from federal programs. Our practices in New Jersey, Nevada, Nebraska, North Carolina, and Kentucky must operate within all applicable guidelines.
- Patient Trust: Clear communication about charges and coverage builds trust. When patients understand their bills and feel they are charged fairly, satisfaction and loyalty grow.
- Efficient Claims Processing: Accurate claims are processed quickly, reducing administrative overhead and the rework caused by denials.
- Data-Driven Decisions: Data from accurate billing provides invaluable insights into your practice’s performance. This allows for informed decision-making to identify areas for improvement and track financial health. For more insights into tracking your practice’s financial pulse, consider exploring our resources on Financial Health KPIs.
Common Coding and Documentation Problems
Even with the best intentions, podiatry practices frequently encounter specific coding and documentation pitfalls that can lead to denials and audits.
- Nail Debridement Codes (11720-11721): These are frequently scrutinized. Insufficient documentation of medical necessity, especially for routine nail care, or incorrect application of modifiers can trigger denials. The OIG identified incorrect coding as 11.5% of improper payments for podiatric providers.
- E/M Services (e.g., 99203-99205): Billing for an Evaluation and Management (E/M) service on the same day as a procedure is a common audit trigger. The E/M service must be “significant and separately identifiable” from the procedure and require modifier 25. Documentation must clearly support this separate service, going beyond the typical pre- and post-work inherent to the procedure.
- Modifiers (25, 59): Modifier 25, as mentioned, indicates a separate E/M service. Modifier 59 signifies a distinct procedural service. Misuse or overuse of these modifiers, without clear supporting documentation, is a red flag for auditors.
- Laterality: Many podiatric conditions and procedures are specific to the left or right foot. Failing to use appropriate laterality modifiers (e.g., -LT, -RT) or indicating it clearly in documentation can lead to coding errors.
- Medical Necessity Proof: This is the big one. As the statistics show (76.4% of improper payments due to insufficient documentation), claims often lack the detailed clinical evidence needed to prove that a service was “reasonable and necessary.” This is particularly true for routine foot care, where the burden of proof is high.
Proper documentation is our shield against these issues. It’s not just about what we do, but how carefully we record why we do it.
Navigating Medicare’s Maze: Routine Foot Care and Systemic Conditions
Medicare policies for podiatric services, especially routine foot care (RFC), can feel like a labyrinth. Medicare generally excludes RFC services—like cutting corns, calluses, or trimming nails—assuming patients or caregivers can perform them.
However, there are critical exceptions, and understanding these is key to podiatry billing compliance. Routine foot care can be covered if it is medically necessary and integral to the treatment of a systemic condition that makes the patient “at risk.” This means that due to their underlying health issues, performing self-care could be dangerous, leading to infection or injury.
Common systemic conditions that may justify coverage for routine foot care include:
- Diabetes Mellitus: This is perhaps the most well-known. Diabetic patients often have compromised circulation and nerve function, making even minor foot injuries dangerous.
- Peripheral Vascular Disease (PVD): Conditions affecting blood flow to the extremities can severely impair healing and increase infection risk.
- Neuropathies: Conditions like peripheral neuropathy (often associated with diabetes or alcoholism) can lead to loss of sensation, making it difficult for patients to detect injury.
- Arteriosclerosis Obliterans: A severe form of hardening of the arteries.
- Chronic Kidney Disease: Can also impact circulation and nerve health.
For coverage, Medicare requires an “active care” component. The patient must be under a physician’s care for the systemic disease within a reasonable timeframe (typically 6 months) before the RFC service. The condition must be actively managed and documented.
The Key to Coverage: Class Findings and Q Modifiers
When billing Medicare for routine foot care due to a systemic condition, we enter the field of “Class Findings” and “Q modifiers.” These are specific criteria that help justify the medical necessity of the service.
Medicare defines three classes of findings, indicating the severity of the systemic condition’s impact on the patient’s feet:
- Class A Findings: These are severe and represent signs of non-traumatic amputation of the foot or integral part thereof. One Class A finding is sufficient for presumptive coverage.
- Class B Findings: These indicate a significant circulatory or neurological impairment, such as absent posterior tibial pulse, advanced trophic changes (e.g., hair loss, shiny skin), or edema. Two Class B findings are typically required for presumptive coverage.
- Class C Findings: These represent less severe signs of impairment, including claudication, temperature changes, or paresthesia. One Class B finding combined with two Class C findings can also lead to presumptive coverage.
To communicate these findings to Medicare, we use specific Q modifiers:
- Q7 Modifier: Used when there is one Class A finding.
- Q8 Modifier: Used when there are two Class B findings.
- Q9 Modifier: Used when there is one Class B finding and two Class C findings.
Linking these findings directly to the appropriate Q modifier in our billing is absolutely critical. Without the correct Q modifier, even with impeccable documentation of systemic conditions, the claim will likely be denied. This level of detail is a cornerstone of Medicare Podiatry Billing Guidelines.
Best Practices for Medicare Documentation
Given the scrutiny surrounding routine foot care and systemic conditions, our documentation must be impeccable. Here are some best practices:
- Document the Systemic Condition: Clearly state the qualifying systemic condition (e.g., diabetes mellitus with peripheral neuropathy).
- Physician Visit Within 6 Months: Confirm and document that the patient has been seen by an MD/DO for the complicating systemic disease within the last 6 months.
- Specific Physical Findings: Detail the exact Class A, B, or C findings observed during the examination. Vague descriptions won’t cut it. For example, instead of “poor circulation,” specify “absent dorsalis pedis pulse.”
- Number of Nails/Lesions Treated: For services like nail debridement or paring of corns/calluses, accurately document the number and location of the nails or lesions treated.
- Pain and Ambulation Limitations: If pain is a factor, objectively document how it impacts the patient’s ability to ambulate or perform self-care. Pain merely during the nail cutting procedure itself is generally not sufficient.
- Medical Necessity Narrative: Provide a clear narrative explaining why the routine foot care is medically necessary due to the systemic condition, emphasizing the risk of injury or infection if not professionally performed.
The goal is to paint a complete and undeniable picture for the payer. For more detailed guidance, we often refer to the CMS guidance on Podiatry Care.
The High Stakes of Non-Compliance: Audits, Fraud, and Penalties
Non-compliance brings significant legal and financial risks that can threaten your practice. The regulatory environment is complex, and the consequences of missteps are severe.
Audits are a reality in healthcare, and podiatry practices are no exception. What triggers an audit?
- Unusual Billing Patterns: Billing significantly more frequently or for higher-level services than peers in your specialty or geographic area (e.g., New Jersey, Nevada, Nebraska, North Carolina, Kentucky) can flag your practice.
- High-Cost Claims: Claims for expensive procedures or devices are often scrutinized.
- Inconsistent Coding: Frequent use of certain modifiers (like 25 or 59), or coding that doesn’t align with documentation.
- Patient Complaints: Dissatisfied patients can report billing irregularities.
- Disgruntled Employees: Former employees with knowledge of questionable practices can become whistleblowers.
- Random Selection: Sometimes, you’re just unlucky, as agencies like Medicare conduct random audits to assess error rates.
Various types of audits include:
- Medicare Audits: Conducted by Medicare Administrative Contractors (MACs) or specialized audit contractors.
- Medicaid Audits: Conducted by state Medicaid agencies (e.g., Nevada Medicaid, Nebraska Medicaid) or their contractors.
- Private Payer Audits: Commercial insurance companies conduct their own audits.
- Recovery Audit Contractor (RAC) Audits: Focus on identifying and recovering improper payments.
- Zone Program Integrity Contractor (ZPIC) Audits: More severe, investigating potential fraud and abuse.
- Comprehensive Error Rate Testing (CERT) Audits: Assess the accuracy of Medicare claims by reviewing a random sample.
Beyond innocent errors, practices must be vigilant about fraud. Common forms include:
- Upcoding: Billing for a more expensive service than what was actually performed (e.g., billing for a complex nail debridement when only routine trimming occurred).
- Unbundling: Billing separately for services that are typically considered part of a single procedure (e.g., billing for local anesthesia separately when it’s included in a surgical code).
- Billing for Services Not Rendered: Charging for procedures or visits that never happened.
- Misrepresentation of Services: Falsely describing the services provided to secure payment.
- Duplicate Billing: Submitting multiple claims for the same service.
- Kickbacks and Referrals: Engaging in unlawful financial arrangements to induce referrals.
Key Regulations Every Podiatrist Must Know
To steer this landscape, be familiar with key compliance regulations:
- HIPAA (Health Insurance Portability and Accountability Act): Protects patient privacy and security of health information. Compliance involves secure record-keeping, electronic data transmission, and patient consent for information sharing.
- CMS Guidelines: The Centers for Medicare & Medicaid Services sets standards for billing and coding for Medicare and Medicaid beneficiaries, influencing National Coverage Determinations (NCDs) and Local Coverage Determinations (LCDs).
- Anti-Kickback Statute (AKS): Prohibits knowingly and willfully soliciting or receiving, or offering or paying, any remuneration (e.g., money, gifts) to induce or reward referrals for items or services reimbursable by federal healthcare programs.
- Stark Law (Physician Self-Referral Law): Prohibits physicians from referring Medicare or Medicaid patients to entities for certain designated health services if the physician (or an immediate family member) has a financial relationship with that entity, unless an exception applies.
- False Claims Act (FCA): Imposes liability on persons and companies who defraud governmental programs. This is where allegations of upcoding, unbundling, or billing for services not rendered can lead to severe penalties.
- OIG Compliance Guidance: The Office of Inspector General (OIG) provides guidelines for healthcare providers to develop effective compliance programs, helping prevent fraud, waste, and abuse.
Understanding the Consequences of Non-Compliance
The stakes are high, and non-compliance can lead to devastating consequences:
- Financial Penalties: These can be substantial, including fines per false claim, treble damages (three times the amount of the improper payment), and civil monetary penalties.
- Recoupments: Payers will demand repayment of any improper payments, often with interest. This can be a huge blow to a practice’s finances.
- Exclusion from Federal Programs: Practices or individual providers found in violation can be excluded from participating in Medicare, Medicaid, and other federal healthcare programs, effectively shutting down a significant portion of their business.
- Legal Action: This can range from civil lawsuits to criminal charges, potentially leading to jail time for egregious fraud.
- Reputational Damage: Allegations of non-compliance or fraud can severely damage a practice’s reputation, eroding patient trust and making it difficult to attract new patients.
- Increased Scrutiny: Once identified, a practice may face ongoing audits and heightened oversight, diverting valuable resources and time.
An OIG report on non-compliant podiatry claims found that nearly half of sampled claims for routine foot care services did not comply with Medicare requirements, leading to an estimated $4.4 million in improper payments. This highlights the very real and significant risks we face. You can review the full report at Podiatrists’ Claims for Routine Foot Care Services Did Not Comply With Medicare Requirements .
A Proactive Approach to Podiatry Billing Compliance
Given the complexities and risks, a proactive approach to podiatry billing compliance is essential. Build a fortress of best practices around your operations.
Key elements of a robust compliance strategy include:
- Internal Controls: Establishing clear policies and procedures for every step of the billing process, from patient intake to claims submission.
- Staff Training: Regularly educating our team on the latest coding updates, payer policies, and compliance regulations. The landscape is always shifting, so continuous learning is paramount.
- Payer Policy Review: Proactively reviewing and understanding the specific requirements of Medicare, Medicaid (in states like New Jersey, Nevada, Nebraska, North Carolina, and Kentucky), and all commercial payers we work with.
- Prior Authorization Management: Implementing a rigorous system to obtain prior authorizations for services that require them before they are rendered.
- Patient Payment Policies: Establishing clear, transparent payment policies and communicating them effectively to patients upfront, including options for multiple payment methods.
Mastering Documentation for Optimal Podiatry Billing Compliance
Documentation is your strongest defense. It’s the story of the patient’s visit, justifying the services provided and supporting your claims. Robust documentation directly contributes to successful billing and reduces claim denials.
Best practices for documentation include:
- Real-time Documentation: Documenting during or immediately after the patient encounter ensures accuracy and completeness, minimizing forgotten details.
- Standardized Templates: Utilizing consistent templates within our EHR system helps ensure all necessary information is captured for specific visit types or procedures.
- EHR Utilization: Leveraging Electronic Health Record (EHR) systems to streamline documentation, improve legibility, and integrate with billing systems for greater efficiency.
- Detailed Procedure Notes: For every procedure, our notes must be highly specific, detailing the procedure performed, the anatomical location, laterality, any complications, and the patient’s response.
- Clear Medical Necessity Justification: Articulate why each service was performed, linking it directly to the patient’s diagnosis and treatment plan.
Essential documentation elements:
- Patient identification (name, date of birth)
- Date of service
- Chief complaint
- History of present illness
- Review of systems
- Physical examination findings (especially Class Findings for RFC)
- Assessment/Diagnosis (with specific ICD-10 codes, including laterality)
- Treatment plan (including CPT codes for services rendered)
- Medical necessity statement (especially for routine foot care)
- Orders for tests, referrals, or DME
- Physician’s signature and credentials
Navigating Payer Policies and Prior Authorizations
Payer policies are not uniform. Medicare coverage can differ significantly from a commercial payer, and Medicaid rules vary by state.
- Medicare vs. Commercial Payers: Medicare sets a federal baseline, but private insurers can have stricter or looser documentation requirements, different coverage criteria, and varying frequency limits. We must always check individual commercial payer policies.
- Medicaid State Variations: Medicaid is a joint federal and state program, meaning eligibility, coverage, and billing requirements differ significantly from state to state. For our practices in New Jersey, Nevada, Nebraska, North Carolina, and Kentucky, we must be intimately familiar with each state’s specific Medicaid guidelines. For instance, Nevada Medicaid and Nebraska Medicaid have their own detailed provider billing guides that we must adhere to.
- Verifying Coverage Upfront: A critical step in preventing denials is to verify patient coverage and eligibility before the service. This includes checking deductibles, co-pays, and coinsurance.
- Prior Authorization (PA): Many procedures, expensive diagnostic tests, and Durable Medical Equipment (DME) like orthotics require prior authorization. Failing to obtain PA can lead to a complete denial of payment, even if the service was medically necessary.
- Managing Authorization Denials: If a PA is denied, we need a clear process to appeal, providing additional clinical information to justify the request.
Leveraging Technology for Improved Podiatry Billing Compliance
In today’s healthcare environment, technology is an ally in achieving podiatry billing compliance.
- EHR Systems: Modern EHRs streamline documentation, integrate clinical and billing data, and can include coding assistance tools, reducing manual errors.
- Automated Claim Scrubbing: Billing software with claim scrubbing capabilities can identify coding errors, missing information, and potential compliance issues before claims are submitted, drastically reducing denial rates.
- Practice Management Software (PMS): A robust PMS helps manage patient scheduling, demographics, billing, and reporting, providing a centralized system for efficient RCM.
- Predictive Analytics: Some advanced systems use data analytics to identify trends, predict potential audit risks, and optimize billing strategies.
By embracing these technological solutions, we can improve accuracy, improve efficiency, and free up our team to focus on what matters most: patient care. To learn more about how technology can transform your practice, visit our Technology in Podiatry section.
Frequently Asked Questions about Podiatry Billing Compliance
What is the single biggest reason for podiatry claim denials?
Insufficient documentation is the leading cause, accounting for a staggering 76.4% of improper payments for podiatric providers during the 2024 reporting period. Claims are often denied when the medical record fails to adequately support the medical necessity of the service, especially for routine foot care linked to systemic conditions. This means even if the care was clinically appropriate, a lack of detailed, compliant notes will result in non-payment.
Can I bill for an E/M service on the same day as a procedure?
Yes, but with caution and precision. You can bill an Evaluation and Management (E/M) service on the same day as a procedure by using modifier 25, but only if the E/M service is “significant and separately identifiable” from the work typically included in the procedure. This means the E/M service must address a separate and distinct problem or require a level of evaluation beyond what would normally be performed as part of the procedure. Documentation must clearly justify the separate nature of the evaluation, including a distinct chief complaint, history, exam, and medical decision-making related to the E/M service. Auditors frequently scrutinize claims with modifier 25.
What are Q modifiers and when are they required?
Q modifiers (Q7, Q8, Q9) are required by Medicare for routine foot care claims to indicate that the service is medically necessary due to a systemic condition. They correspond to specific “Class Findings” (A, B, C) related to the patient’s vascular and neurological status, justifying why a non-professional cannot safely perform the care.
- Q7: Used when there is one Class A finding (e.g., non-traumatic amputation).
- Q8: Used when there are two Class B findings (e.g., absent pulses, advanced trophic changes).
- Q9: Used when there is one Class B finding and two Class C findings (e.g., claudication, edema, paresthesia).
These modifiers signal to Medicare that despite being “routine foot care,” the service is medically necessary due to the patient’s at-risk systemic condition, and therefore, should be covered. Without the correct Q modifier and supporting documentation, these claims will almost certainly be denied.
Conclusion
Mastering podiatry billing compliance is an ongoing journey, not a destination. It demands continuous education, meticulous documentation, and a proactive approach to changing regulations. We’ve seen how crucial it is to understand the nuances of revenue cycle management, steer Medicare’s specific requirements for routine foot care, and protect our practices from the high stakes of non-compliance.
By embracing best practices—from robust documentation and diligent prior authorization to leveraging technology and continuous staff training—we can not only avoid costly pitfalls but also optimize our practice’s financial health and ensure we continue providing exceptional patient care.
We understand that managing these complexities while also focusing on patient well-being can be a significant challenge. That’s why we specialize in providing 100% US-based billing and revenue cycle management services custom specifically for podiatry practices across New Jersey, Nevada, Nebraska, North Carolina, and Kentucky. Our dedicated, podiatry-specific expertise helps maximize collections and streamline operations, allowing you to focus on your patients’ feet, while we handle the footwork of finance.
Learn more about our specialized Billing Services and how we can support your practice’s journey to optimal compliance and financial success.
