Stepping Up Your Earnings: Understanding Podiatry Reimbursement
Why Understanding Podiatry Reimbursement Rates Matters for Your Practice
Podiatry reimbursement rates are the amounts insurance payers—including Medicare, Medicaid, and private insurers—pay your practice for specific procedures and services. These rates vary significantly based on the payer, your geographic location, the type of service provided, and whether it’s performed in a facility or office setting.
Quick Answer: Key Factors Affecting Your Reimbursement (Updated for 2026)
- Medicare Physician Fee Schedule (PFS): Uses Relative Value Units (RVUs) multiplied by a Conversion Factor (the CF is updated every calendar year and directly impacts your 2026 payments) and adjusted by Geographic Practice Cost Indices (GPCIs)
- Routine vs. Surgical Services: Routine foot care is often excluded unless specific systemic conditions exist; surgical procedures have different coverage rules and post-operative periods
- Documentation Requirements: Insufficient documentation causes the vast majority of improper payments in podiatry
- Payer Variations: State Medicaid programs and private insurers set their own fee schedules, which may differ significantly from Medicare rates
For busy podiatrists, understanding these rates is crucial for your practice’s financial health. Recent Medicare data continue to show a double‑digit improper payment rate for podiatry, representing hundreds of millions of dollars in preventable revenue loss each year. Most errors come from avoidable documentation and coding mistakes.
The challenge is that reimbursement structures are complex and always changing. For example, Medicare’s Conversion Factor is revised annually through rulemaking and legislation, directly impacting your bottom line. Furthermore, RVU values and geographic adjustments mean payments differ by procedure and location.
This guide breaks down how podiatry reimbursement works today, from Medicare’s fee schedule to state Medicaid and private payer rules. You’ll learn to prove medical necessity, avoid billing pitfalls, and maximize your rates with proper coding and documentation.
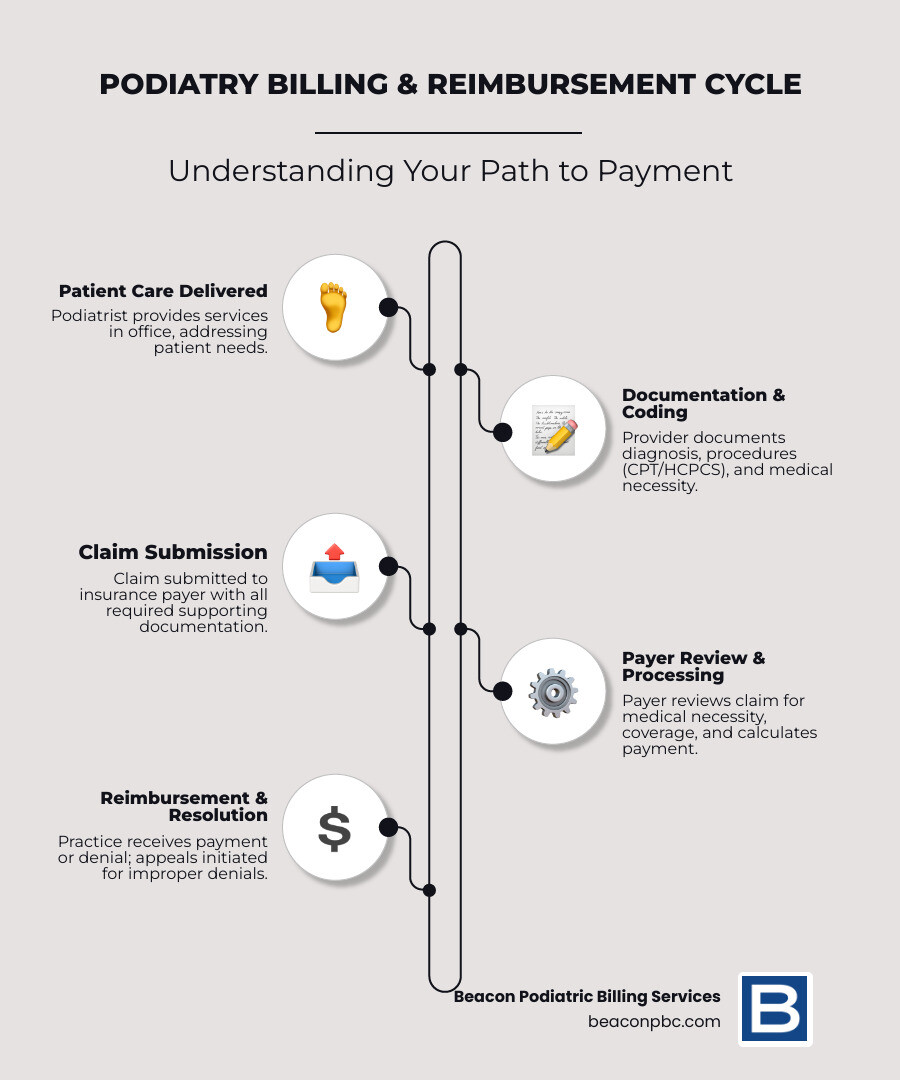
The Core Components of the Physician Fee Schedule (PFS)
The Medicare Physician Fee Schedule (PFS) dictates how physicians are paid and is crucial for optimizing your podiatry reimbursement rates. The PFS calculates payment based on the relative resources used to furnish a service, broken down into three categories of Relative Value Units (RVUs):
- Work RVUs: Reflect the provider’s effort, time, and skill for a service.
- Practice Expense RVUs: Cover overhead costs like rent, staff salaries, and supplies.
- Malpractice RVUs: Account for the cost of professional liability insurance.
These RVUs are converted into a dollar amount using a fixed-dollar Conversion Factor (CF). This dollar amount acts as a multiplier to convert RVUs into a final payment. The CF is updated annually (for example, it changed between 2024 and 2025 and will be updated again for 2026), directly affecting revenue.
Finally, Geographic Practice Cost Indices (GPCIs) adjust payments to account for regional cost differences in labor, rent, and malpractice. A service in Jersey City, NJ, will reimburse differently than one in Omaha, NE.
It’s also important to note the distinction between facility vs. non-facility fees. Services in a private office (non-facility) have higher practice expense RVUs than those in a hospital or ASC (facility), as the facility bears the overhead costs.
For a deeper dive into how this all works, you can find More info about the Physician Fee Schedule.
How RVUs and Conversion Factors Determine Your Payment
The calculation for your Medicare payment looks like this:
(Work RVU * Work GPCI) + (Practice Expense RVU * Practice Expense GPCI) + (Malpractice RVU * Malpractice GPCI) = Total Adjusted RVUs
Total Adjusted RVUs * Conversion Factor = Medicare Payment
CMS issues annual PFS updates, which include revised RVUs, a new Conversion Factor, and budget neutrality adjustments. Budget neutrality requires that payment increases for some services are offset by decreases elsewhere, causing fluctuations in podiatry reimbursement rates from year to year.
The impact of legislative changes remains significant, as Congress can step in to modify the Conversion Factor or other elements of the PFS, which can materially alter podiatry reimbursement rates in 2026 and beyond. Staying informed about these changes is vital.
Understanding these mechanics is about safeguarding your practice’s financial health. If you find yourself overwhelmed by the intricacies of RVU calculations, conversion factors, and annual updates, specialized billing partners like us can help. Find More info about our Billing Services.
Understanding Geographic Adjustments (GPCIs)
GPCIs are a critical factor in podiatry reimbursement rates, reflecting cost-of-practice differences across the U.S. and causing payment for the same service to vary by location.
CMS uses a Zipcode to Carrier Locality File to map ZIP codes to payment localities, creating different urban vs. rural rates. This system of locality-based payment means a practice in a high-cost urban area like Jersey City, New Jersey, will have different GPCIs than one in rural Kentucky.
The impact on practice location decisions is significant. Understanding the GPCIs for potential locations is an important part of financial planning, as higher GPCIs might help offset higher rent in a metropolitan area. It’s a complex interplay that directly influences your potential podiatry reimbursement rates in 2026 and future years.
Mastering Medicare: A Podiatrist’s Guide to Coverage and Compliance
Navigating Medicare Part B rules is essential for proper podiatry reimbursement rates and compliance.
Recent Medicare data show an ongoing, liftd improper payment rate for podiatry, representing hundreds of millions of dollars in at-risk revenue—much of which practices can prevent with better processes. The top reasons for these improper payments are:
- Insufficient documentation: This accounts for the majority of improper payments and means the medical record lacked evidence to support the claim.
- Incorrect coding: This includes using the wrong CPT code or modifier.
- No documentation: Some improper payments occur because no documentation was submitted at all.
- Medical necessity: These denials mean Medicare determined the service wasn’t reasonable and necessary.
These statistics prove that meticulous documentation and accurate coding are direct drivers of your practice’s financial health in 2026 and beyond. We can help you steer these complexities and ensure you’re compliant. For detailed guidelines, refer to our Medicare Podiatry Billing Guidelines.
The “Routine Foot Care” Exclusion and Its Critical Exceptions
A common point of confusion is Medicare’s “routine foot care” exclusion. Generally, Medicare does not cover services like trimming nails or removing corns and calluses, as they are considered non-medical or preventive.
However, there are crucial exceptions where these services are covered. Understanding these is key to ensuring appropriate podiatry reimbursement rates.
Medicare will cover routine foot care services when they are:
- A necessary and integral part of otherwise covered services: For example, nail trimming required to treat a covered ulcer.
- For the treatment of warts: This is covered on the foot just as it is elsewhere on the body.
- For mycotic nails: Treatment of fungal nails may be covered if there is clinical evidence of infection causing pain or limiting ambulation. Detailed documentation is paramount.
- Due to systemic conditions: This is the most significant exception. Routine care may be covered if a patient’s systemic condition causes severe circulatory issues or reduced sensation in the legs or feet.
This means a nail trim for a healthy patient isn’t covered, but the same service for a diabetic patient with severe neuropathy could be. The difference is the medical necessity driven by the systemic condition.
Proving Medical Necessity: Systemic Conditions and Coverage Presumption
Proving medical necessity is paramount for securing podiatry reimbursement rates, especially for services that fall under the routine foot care exclusion. Systemic conditions are key to justifying this coverage.
Medicare recognizes several systemic conditions that can justify routine foot care, including:
- Diabetes mellitus
- Arteriosclerosis obliterans
- Buerger’s disease
- Chronic thrombophlebitis
- Peripheral neuropathies with evidence of neuropathy
For coverage, the medical record must clearly show the systemic condition has resulted in severe circulatory discomfort or reduced sensation. Medicare establishes a coverage presumption based on specific clinical findings of severe peripheral involvement, categorized as:
- Class A Finding: Nontraumatic amputation of the foot or part of the foot.
- Class B Findings: Absent posterior tibial pulse, advanced trophic changes (e.g., hair loss, skin changes), or other signs of vascular insufficiency.
- Class C Findings: Claudication, temperature changes, edema, paresthesia, or burning.
Coverage is presumed with one Class A finding, two Class B findings, or one Class B and two Class C findings. The patient must also be under the active care of an MD or DO for the systemic condition.
Documentation best practices are non-negotiable in the current Medicare environment:
- Clearly link the systemic condition to the need for foot care.
- Document the specific Class A, B, or C findings.
- Note the date of the last visit with the patient’s primary care physician.
- Describe the services provided and why they were medically necessary.
For more detailed guidance on these critical aspects, refer to More info about Medicare Podiatry Care.
Differentiating Reimbursement for Routine vs. Surgical Podiatry Services
Podiatry reimbursement rates differ significantly between routine care and surgical procedures. Coverage for podiatric surgery is generally more straightforward if medically necessary.
Surgical CPT codes have higher RVUs but often include bundled services. A key concept is the post-operative follow-up period (for example, 90 days for some procedures), during which routine follow-up visits are part of the initial surgical payment and cannot be billed separately. Bundled services can also include local anesthesia.
Pre-operative assessments may be included in the surgical fee. A non-referred pre-operative assessment might only be billable if the case proceeds to surgery. Understanding these nuances remains crucial for maximizing your podiatry reimbursement rates under current Medicare rules. This is where robust practice management becomes invaluable. Learn more about More info about Practice Management & Growth.
Navigating Varying Podiatry Reimbursement Rates Across Payers
While Medicare sets a benchmark, it’s just one piece of the podiatry reimbursement rates puzzle. State Medicaid programs and private insurers have unique rules and fee schedules, causing payment for the same service to vary dramatically.
Our goal is to help you understand these variations to optimize your practice’s financial health.
| Feature | Medicare (Federal) | Nebraska Medicaid (State Example) | New Jersey Medicaid (State Example) | Nevada Medicaid (State Example) | North Carolina Medicaid (State Example) | Typical Private/Commercial Plan (General) |
|---|---|---|---|---|---|---|
| Fee Schedule | Physician Fee Schedule (PFS) – RVUs, CF, GPCIs | Practitioner Fee Schedule for Podiatry Services | Fee Schedules – NJ.gov | Nevada Medicaid Fee Schedules | Podiatry Services Fee Schedule | Contracted rates, “reasonable and customary” fees, UCR (Usual, Customary, and Reasonable) |
| Reimbursement Basis | RVU-based calculation (lower of charge or max allowable) | Lower of usual/customary or max allowable; Invoice cost (IC) for some supplies | State-specific fee schedules | State-specific fee schedules | State-specific fee schedules | Negotiated rates, sometimes based on a percentage of Medicare rates or UCR |
| Copayments | Patient responsibility (deductible, coinsurance) | Varies by plan/service | Varies by plan/service | Varies by plan/service | Varies by plan/service | Varies greatly by plan, deductible, coinsurance, copayments |
| Prior Authorization | Required for some services/devices | Required for certain podiatry services (Form 471-000-206) | Required for some services/devices | Required for some services/devices | Required for some services/devices | Common for high-cost procedures, imaging, or specific therapies |
| Routine Foot Care | Excluded, with specific medical necessity exceptions | Varies, often with medical necessity and systemic condition requirements | Varies, often with medical necessity and systemic condition requirements | Varies, often with medical necessity and systemic condition requirements | Varies, often with medical necessity and systemic condition requirements | Varies by plan, often excluded unless medically necessary for systemic conditions |
| Billing for Supplies | Incident-to supplies (e.g., skin substitutes) | Office use only; no take-home supplies can be billed | Varies by plan | Varies by plan | Varies by plan | Varies by plan, often bundled or reimbursed separately |
| Network Advantages | N/A (federal program) | N/A (state program) | N/A (state program) | N/A (state program) | N/A (state program) | In-network providers typically receive higher reimbursement and direct payment |
This table shows how different payers approach podiatry reimbursement rates. It’s clear that payer-specific rules are paramount. For private plans, being an in-network provider often offers significant advantages in reimbursement and payment processing.
State Medicaid Variations: A Snapshot
Each state’s Medicaid program sets its own policies and podiatry reimbursement rates. A provider in New Jersey will face different rules than one in Nebraska, Nevada, or North Carolina.
Here are some examples that remain relevant for 2026 planning:
-
Nebraska Medicaid: Uses a specific podiatry fee schedule, reimbursing the lower of the charge or their max allowable. It has unique rules for prior authorization, billing for supplies (office use only), and limits on orthopedic devices.
-
New Jersey Medicaid: The New Jersey Department of Banking and Insurance (NJDOBI) publishes fee schedules that providers must follow. It’s crucial for NJ practices to consult official NJDOBI resources for the most current rates and guidelines.
-
Nevada Medicaid: Maintains its own “Nevada Medicaid Fee Schedules.” Providers in Nevada must consult these schedules to find the maximum allowable fees and coverage policies in the current year.
-
North Carolina Medicaid: Provides a “Podiatry Services Fee Schedule Archive,” which is updated regularly. Providers must access the latest schedule for accurate billing.
These examples show you cannot assume uniformity across state Medicaid programs. Each has unique state-specific fee schedules, copayments, prior authorization requirements, and rules for billing for supplies. It is imperative for practices in states like New Jersey, Nevada, Nebraska, North Carolina, and Kentucky to be familiar with their state’s current Medicaid policies when planning for 2026 revenue.
Private and Student Health Plan Considerations
Private and student health plans also have varied approaches to podiatry reimbursement rates, making it crucial to understand each plan’s policies. Many private plans use a system of “reasonable and customary fees” or “usual, customary, and reasonable (UCR)” charges, often based on their internal data or a percentage of Medicare rates.
The principle of coordinating benefits is also common. If a patient has multiple insurance plans, the primary plan’s benefits must be used before the secondary plan covers costs. This is a critical step in the claims process.
For private plans, being an in-network provider is advantageous. Network providers agree to contracted podiatry reimbursement rates, which are generally higher and more predictable than out-of-network payments.
Benefit limitations, such as annual maximums or visit limits, are also common. Always in 2026 and going forward:
- Verify patient eligibility and benefits before the appointment.
- Understand the plan’s fee schedule or UCR policies.
- Be aware of prior authorization requirements.
- Inform patients about their financial responsibility.
Common Billing Challenges and How to Boost Your Financial Health
Even with a solid grasp of podiatry reimbursement rates, practices face common billing challenges like claim denials, incorrect coding, and policy changes that hinder cash flow. As noted, Medicare’s improper payment rate for podiatry remains driven largely by preventable documentation and coding errors.
Payer audits are another significant challenge that can lead to recoupments and penalties if documentation is lacking. The solution is robust revenue cycle management (RCM)—an end-to-end process from patient registration to denial management. A well-managed RCM system is proactive, identifying issues before they become denials and ensuring every earned dollar is collected.
We understand these challenges. Our specialized billing services are designed to streamline your operations and maximize your podiatry reimbursement rates in the current regulatory environment. Stay ahead of the curve with our More info about Billing & Coding Updates.
Why Documentation is the Key to Maximizing Podiatry Reimbursement Rates
The golden rule of billing—”if it wasn’t documented, it wasn’t done”—is especially true for podiatry reimbursement rates. Insufficient documentation accounts for the majority of Medicare’s improper podiatry payments.
Effective documentation is your best defense against denials and audits. It must:
-
Link diagnosis to procedure: The diagnosis code (ICD-10) must logically support the procedure code (CPT/HCPCS).
-
Prove medical necessity: Your notes should detail the patient’s complaint, exam findings, assessment, and treatment plan. For routine foot care exceptions, you must document the systemic condition and the Class A, B, or C findings.
-
Support audit defense: Thorough notes should allow an auditor to easily follow the patient’s story and confirm that services were medically necessary.
-
Reduce denials: A complete narrative minimizes the chance of a payer questioning your claim, leading to faster payments.
An “adequate clinical record” contains enough information for another practitioner to understand the service provided. Mastering documentation is a direct path to improving your podiatry reimbursement rates in 2026 and beyond. For more insights into optimizing your practice’s financial health, explore our More info about Financial Health KPIs.
Staying Current with Changing Fee Schedules and Rules
Podiatry reimbursement rates and their governing rules are constantly changing. To avoid revenue loss and ensure compliance, practices must stay current.
Here is how to maintain vigilance in 2026:
-
Track effective dates: Every policy or fee schedule change has an effective date. Missing these can lead to denials or underpayments.
-
Monitor annual updates: Payers release major updates annually, but also quarterly or monthly. Stay on top of new codes, revised RVUs, and changing medical necessity criteria.
-
Read payer newsletters: Subscribe to alerts from MACs and state Medicaid programs to get timely information directly from the source.
-
Use professional associations (APMA): Organizations like the American Podiatric Medical Association (APMA) are invaluable. They analyze proposed rules, advocate for podiatrists, and disseminate critical information about changes affecting your podiatry reimbursement rates.
-
Review proposed rules (MPFS): Following proposed rules, like the Medicare Physician Fee Schedule (MPFS) proposal each year, offers a glimpse into future changes, allowing you to adjust your strategies accordingly.
Proactive management of these updates is a cornerstone of successful revenue cycle management. For more insights and resources, explore our More info about our Articles.
Frequently Asked Questions about Podiatry Reimbursement
We know that navigating the complexities of podiatry reimbursement rates can generate a lot of questions. Here are some of the most common inquiries we receive:
How often do podiatry reimbursement rates change?
Podiatry reimbursement rates change frequently. Medicare’s Physician Fee Schedule (PFS) is updated annually, as are many state Medicaid and private plan schedules. Legislative action can also cause changes at any time, making vigilance essential.
What is the difference between a facility and a non-facility reimbursement rate?
The difference is where the service is performed and who covers the overhead costs.
- Non-facility rates apply to services in a physician’s private office. These rates are higher because the practice expense RVU is larger to cover costs like rent, staff, and utilities.
- Facility rates apply to services in a hospital or ambulatory surgical center (ASC). These rates are lower because the facility bears the overhead costs, so the physician’s practice expense RVU is reduced.
Are services like orthotics or supportive devices covered?
Coverage for orthotics and supportive devices varies widely by payer and medical necessity.
- Medicare: Coverage is limited. It’s available for devices that are part of a leg brace or for therapeutic shoes for diabetic patients under strict criteria. Routine orthotics are generally not covered.
- State Medicaid: Coverage depends on each state’s specific policies. For example, Nebraska Medicaid has rules allowing for a maximum of two medically necessary orthopedic devices per visit, implying specific coverage criteria.
- Private Insurance: Coverage varies greatly. Many plans cover medically necessary orthotics but may require prior authorization, have vendor limitations, or cap the number of devices covered per year. Always verify benefits for each patient.
Conclusion
Navigating podiatry reimbursement rates is challenging but vital for your practice’s growth. We’ve covered the Medicare Physician Fee Schedule, routine foot care exceptions, and payer variations in states like New Jersey, Nebraska, Nevada, North Carolina, and Kentucky.
The key takeaways for 2026 are clear:
- Understand the Mechanics: Grasp how RVUs, Conversion Factors, and GPCIs work and how they are updated each year.
- Master Medical Necessity: Prove why every service is necessary, especially for routine care exceptions.
- Document Carefully: Your notes are your best defense against denials and audits.
- Know Payer Rules: Each payer is different; what works for one may not work for another.
- Stay Updated: Reimbursement rules are dynamic, so continuous learning is essential.
Proactive financial management optimizes your revenue cycle. This is where the importance of specialized billing is clear. At Guide Podiatric Billing Services, we are your dedicated partners, offering 100% US-based expertise custom to podiatry. Our goal is to maximize your collections and streamline operations, so you can focus on patient care.
Don’t let complex reimbursement rules undermine your practice’s financial health.
Contact us to optimize your billing services and step confidently towards a more profitable future in 2026 and beyond.