Podiatry claims processing: Optimize 2026 Success
Why Podiatry Claims Processing Determines Your Practice’s Financial Health
Podiatry claims processing is the specialized workflow that transforms your clinical services into revenue—covering everything from coding and documentation to claim submission, denial management, and final payment. According to Medicare data, the improper payment rate for podiatry care stands at 11.2%, with insufficient documentation accounting for 76.4% of denials. That translates to $216.9 million in projected improper payments annually.
Here’s what makes podiatry claims processing different:
- Routine foot care is typically excluded unless linked to systemic conditions like diabetes or peripheral vascular disease
- Class findings (A, B, C) and Q-modifiers (Q7, Q8, Q9) must be documented to justify medical necessity
- Payer policies vary dramatically between Medicare and commercial insurers for identical services
- High denial rates (often 18% or higher) result from coding errors, missing modifiers, and inadequate documentation
- Prior authorizations are frequently required for orthotics, DME, and surgical procedures
If you’re a busy podiatrist, these complexities likely mean delayed payments, reduced collections, and less time for patient care. The average practice spends up to 28 days in claim cycles—time that could be spent growing your practice instead of fighting denials.
The good news? Understanding the claims process from service to settlement can dramatically improve your revenue cycle. Practices using specialized billing services report clean claim rates of 98% and payments up to 3x faster.
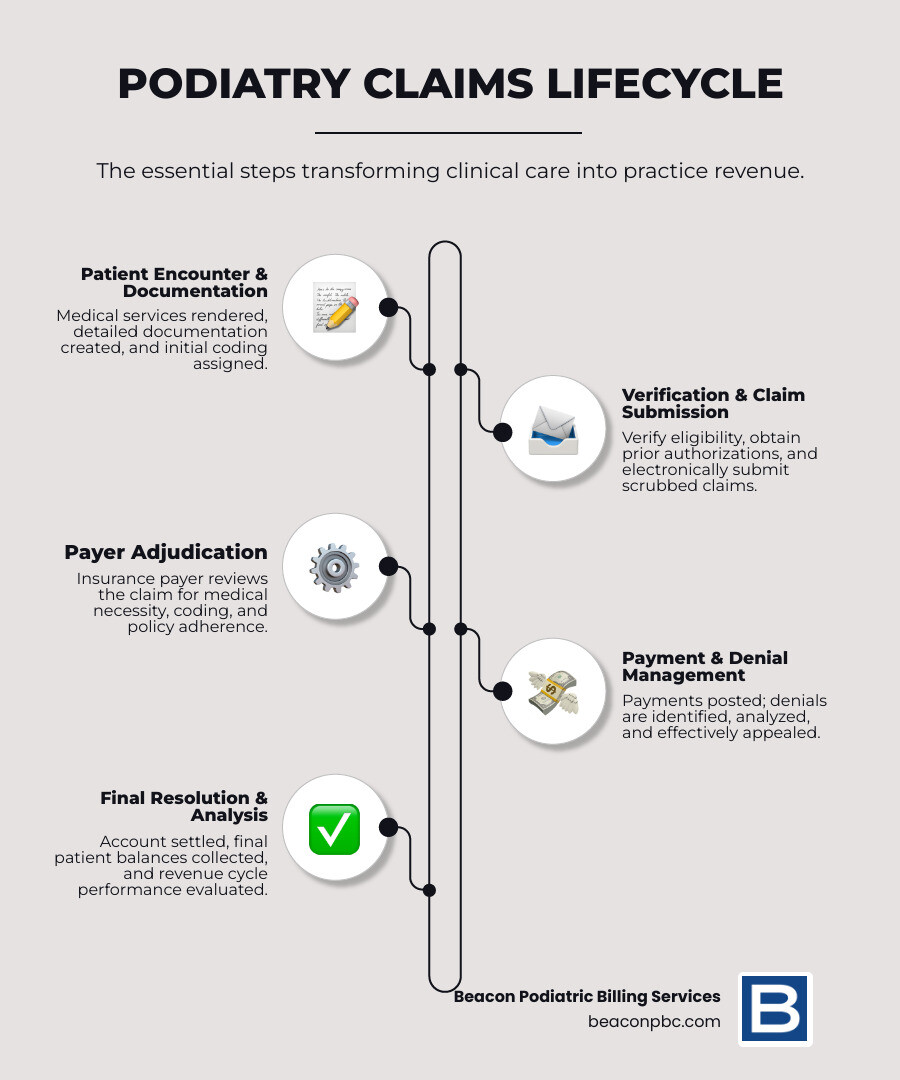
Why Podiatry Billing is Uniquely Complex
Podiatry isn’t just about feet; it’s a highly specialized medical field focused on the diagnosis and treatment of disorders of the foot, ankle, and lower extremity. This specialization brings with it a unique set of challenges in billing and claims processing that can significantly impact a practice’s revenue cycle management and financial stability. As our research shows, the podiatry billing process encounters certain challenges that set it apart from other medical specialties.

One of the biggest problems is distinguishing between routine foot care and medically necessary services. What seems routine to a patient might be a critical intervention for someone with a systemic condition. The variability in insurance coverage, the need for precise documentation to justify medical necessity, and the frequent policy updates from Medicare and private insurers all contribute to a complex landscape. For us, navigating these intricacies is a daily task, ensuring that your practice in New Jersey, Nevada, Nebraska, North Carolina, or Kentucky or any state that you might practice in, gets the reimbursement it deserves.
The Critical Role of Systemic Conditions
Here’s where podiatry billing gets particularly nuanced, and frankly, a bit tricky. Many podiatric services, especially what might be considered “routine” care like nail trimming or callus removal, are only covered by Medicare and many commercial payers if the patient has an underlying systemic condition. Think of conditions like:
- Diabetes: A chronic condition that can lead to severe foot complications, including neuropathy (nerve damage) and peripheral vascular disease (PVD).
- Peripheral Vascular Disease (PVD): Affects blood circulation, increasing the risk of infection and slow-healing wounds in the feet.
- Neuropathy: Nerve damage, often a complication of diabetes, leading to reduced sensation and an inability to detect foot injuries.
For these at-risk patients, routine foot care isn’t just about comfort; it’s preventative medicine that can avert serious issues like infections, ulcerations, or even amputations. To justify coverage for such services, meticulous documentation is paramount. This is where “Class Findings” come into play:
- Class A: Indicates a non-traumatic amputation of the foot or part of the foot, or other significant physical findings.
- Class B: Involves two of the following findings: absent posterior tibial pulse, absent dorsalis pedis pulse, edema, skin changes (e.g., thinning, shiny, hair loss), or temperature abnormalities.
- Class C: Involves one of the following findings: claudication, pain at rest, or trophic changes (e.g., thickened nails, fungal infections).
These findings, along with specific Q-Modifiers (Q7, Q8, Q9), are essential for linking the routine service to the systemic condition and proving medical necessity. For instance, Q7 is used for one Class A finding, Q8 for two Class B findings, and Q9 for one Class B and two Class C findings. Without these, even the most medically necessary routine foot care claim can be denied.
Common Denial Reasons and How to Fight Them
The reality is, claim denials are a significant drain on revenue. The average denial rate for podiatry claims can be as high as 18%, leading to substantial financial loss. Our research indicates that insufficient documentation alone accounts for a staggering 76.4% of improper payments for podiatric providers. This means that often, the care was provided, but the story wasn’t told clearly enough to the payer.
Common reasons for denials in podiatry claims processing include:
- Insufficient Documentation: As mentioned, this is the big one. If the medical record doesn’t clearly support the service rendered, especially the medical necessity linked to systemic conditions or the severity of a condition, your claim is likely to be rejected.
- Incorrect Coding: Using the wrong CPT, ICD-10, or HCPCS codes, or failing to update to the latest code sets annually, can lead to denials. Precision is key!
- Lack of Medical Necessity: The payer doesn’t believe the service was necessary for the patient’s condition, often due to inadequate documentation.
- Bundling Errors: Billing for services separately when they should be included in a more comprehensive code.
- Missing Modifiers: Forgetting to apply a crucial modifier (like RT/LT, T1-T9, or the Q-modifiers) that clarifies the procedure or circumstance.
So, how do we fight them? Effective denial management isn’t just about appealing; it’s about prevention.
- Proactive Prevention: This starts with meticulous documentation and accurate coding at the point of service. Investing in specialized training for your staff or partnering with experts can drastically reduce initial denial rates.
- Tracking and Analysis: We identify common denial patterns specific to your practice and payers. What are the recurring issues? Which codes or modifiers frequently lead to rejections?
- Appeals Process: When a denial occurs, we act swiftly. This involves understanding the specific reason for denial, gathering additional documentation, and submitting a well-structured appeal with all necessary supporting information. This can feel like wrestling a greased pig sometimes, but we’re tenacious!
By systematically addressing these issues, we can turn denied claims into paid claims, significantly improving your practice’s financial health.
The Core of Podiatry Claims Processing: Coding and Documentation
At the heart of successful podiatry claims processing lies the intricate world of coding and documentation. These aren’t just administrative tasks; they are the language through which your clinical expertise is communicated to insurance payers. Accuracy here directly translates to timely reimbursements and reduced denials. For more insights on the latest updates, you can always check our Billing & Coding Updates.

Every service you provide, every diagnosis you make, and every supply you use must be translated into standardized codes that payers understand. This requires a deep understanding of CPT (Current Procedural Terminology) codes for services, ICD-10 (International Classification of Diseases, 10th Revision) codes for diagnoses, and HCPCS (Healthcare Common Procedure Coding System) codes for supplies and certain services not covered by CPT. On top of that, modifiers add critical details to these codes, clarifying the specifics of the procedure.
Essential CPT and ICD-10 Codes
Let’s explore some of the most frequently used codes in podiatry. While codes are subject to annual updates, understanding the categories is fundamental:
Common CPT Codes for Podiatry:
- 11055-11057: Paring or cutting of benign hyperkeratotic lesions (e.g., corns, calluses).
- 11720-11721: Debridement of nails (e.g., trimming, cutting, grinding of dystrophic nails). This is a prime example where medical necessity and systemic conditions often come into play.
- 11730: Avulsion of nail plate, partial or complete, simple; single. (Often seen with modifiers AG and UA, as per our research on specific billing examples).
- 11750: Excision of nail and nail matrix, partial or complete (e.g., for ingrown toenail).
- 28292-28299: Bunionectomy procedures.
- 29540: Strapping; ankle.
- 99202-99215: Evaluation and Management (E/M) codes for office visits, new and established patients. These require careful documentation of history, exam, and medical decision-making.
- G0127: Trimming of dystrophic nails, for Medicare patients, when certain criteria are met.
Common ICD-10 Codes for Podiatry:
- E11.621: Type 2 diabetes mellitus with diabetic foot ulcer. (This highlights the systemic condition link).
- L60.2: Onychogryphosis (thickened, curved nails).
- M79.67- (M79.671, M79.672, M79.673): Pain in foot (right, left, bilateral). Always remember laterality!
- L84: Corns and callosities.
- B35.1: Tinea unguium (fungal infection of nails).
- I70.20-: Unspecified atherosclerosis of native arteries of extremities. (Another systemic link).
The key is to accurately link the ICD-10 diagnosis code to the CPT procedure code. For example, billing for 11721 (nail debridement) without a supporting diagnosis like L60.2 (onychogryphosis) and a systemic condition like E11.621 (diabetes) will likely result in a denial, especially from Medicare.
Decoding Podiatry-Specific Modifiers
Modifiers are two-character codes appended to CPT or HCPCS codes that provide additional information about the service rendered, clarifying that the service was altered in some way without changing its basic definition. In podiatry, they are absolutely crucial. We’ve even created a Podiatry Billing Made Easy: Your Ultimate Cheat Sheet for CPT Modifiers and Diagnosis Codes to help our clients.
Here are some essential modifiers:
- RT/LT: These indicate laterality (right or left) and are used for services performed on a specific side of the body. For example, if you treat a right foot issue, you’d use RT.
- TA-T9 Toe Modifiers: These are HCPCS modifiers specifically for toes. TA indicates the left foot, first digit; T1 for the left foot, second digit; and so on, up to T9 for the right foot, fifth digit. These are vital for precise billing of toe-specific procedures.
- Modifier 59 (Distinct Procedural Service): Used to identify a procedure or service that was distinct or independent from other services performed on the same day. It’s often used to unbundle services that might otherwise be considered part of a larger procedure.
- Modifier 25 (Significant, Separately Identifiable Evaluation and Management Service by the Same Physician or Other Qualified Health Care Professional on the Same Day of the Procedure or Other Service): This is used when an E/M service (like an office visit) is performed on the same day as a minor procedure, and the E/M service goes above and beyond the typical pre- or post-procedure care.
- Q Modifiers (Q7, Q8, Q9): As discussed, these are critical for routine foot care when systemic conditions are present, indicating the class findings that justify medical necessity.
Using the correct modifiers is non-negotiable. A missing or incorrect modifier is a fast track to a claim denial, leading to unnecessary delays and administrative headaches.
Documentation: Your First Line of Defense
If coding is the language, documentation is the narrative. It’s the detailed story of the patient’s visit, your findings, your medical decision-making, and the services you provided. Without thorough and accurate documentation, even perfectly chosen codes can lead to denials. 76.4% of improper payments are due to insufficient documentation!
Key elements of robust podiatry documentation include:
- SOAP Notes (Subjective, Objective, Assessment, Plan): A structured way to record patient encounters, ensuring all necessary information is captured.
- Proving Medical Necessity: Your documentation must clearly demonstrate why the service was medically necessary. This includes the patient’s symptoms, the severity of their condition, the impact on their daily life, and the expected outcome of the treatment.
- Documenting Systemic Conditions: For routine foot care, clearly state the systemic condition (e.g., diabetes, PVD, neuropathy), its severity, and how it directly impacts the patient’s foot health, increasing their risk.
- Class Findings Documentation: For services tied to systemic conditions, carefully record the specific Class A, B, or C findings you observed during the physical exam. This is the concrete evidence payers look for.
- Surgical Reports: For surgical procedures, a detailed operative report is essential, outlining the procedure performed, findings, anesthesia, complications, and post-operative instructions.
- Prior Authorization Records: Keep clear records of all prior authorizations obtained, including the authorization number and the services it covers.
Medicare, in particular, has stringent documentation requirements for podiatric services. Their Medicare Podiatry Care guidelines emphasize that medical records must clearly support the medical necessity of all services billed. If it’s not documented, it didn’t happen, at least in the eyes of the payer.
Navigating Payer Policies: Medicare vs. Commercial Insurance
One of the biggest headaches in podiatry claims processing is the sheer diversity of payer policies. What Medicare covers, and how, often differs significantly from commercial insurance plans. This means that a billing strategy that works perfectly for one payer might fail miserably for another. We see this supporting practices in diverse states like New Jersey, Nevada, Nebraska, North Carolina, and Kentucky, where regional variations and specific payer contracts add further layers of complexity.
Understanding Medicare Guidelines
Medicare sets the baseline for many podiatry billing rules, and understanding their policies is non-negotiable. Our internal guide on Medicare Podiatry Billing Guidelines is a testament to its importance.
The fundamental rule for Medicare is the routine foot care exclusion. Generally, Medicare does not cover routine services like:
- Cutting or removal of corns and calluses.
- Trimming, cutting, or clipping of nails.
- Hygienic care (e.g., cleaning, soaking, moisturizing).
However, there are crucial exceptions, particularly for “at-risk” patients. Medicare will cover routine foot care if the patient has a systemic condition that significantly increases the risk of complications from minor foot trauma or infection. These are often patients with:
- Diabetes mellitus (E11.xxx)
- Arteriosclerosis obliterans (I70.2-)
- Chronic venous insufficiency (I87.2-)
- Peripheral neuropathies (G57.x-)
For these patients, the key is to document the systemic condition and the “Class Findings” (A, B, C) that justify the medical necessity, as discussed earlier, and apply the appropriate Q-modifiers (Q7, Q8, Q9).
Mycotic nail coverage also has specific criteria. Treatment for mycotic nails (fungal infections) is covered if it’s medically necessary and supported by documentation of severe pain, infection, or the patient’s inability to care for their nails due to a physical or mental impairment.
Another important concept is the active care requirement. For routine foot care to be covered due to a systemic condition, the patient must be under the active care of an MD or DO for that complicating systemic disease. The podiatrist’s documentation should include a statement of physician concurrence, especially if the patient hasn’t seen their primary care physician within the last six months.
Finally, Medicare’s Local Coverage Determinations (LCDs) are vital. These are medical policies developed by Medicare Administrative Contractors (MACs) that specify when certain services are covered and what documentation is required. LCDs can vary by region, so knowing the specific requirements for your practice location is critical.
Mastering Prior Authorizations
Prior authorizations (PAs), also known as pre-certifications, are a common and often frustrating part of dealing with both Medicare Advantage plans and many commercial payers. A PA is essentially permission from the payer before a service is rendered, confirming that they deem it medically necessary and will cover it. Without it, you could be left with an unpaid claim and an unhappy patient.
Services frequently requiring pre-approval in podiatry include:
- Orthotics and Durable Medical Equipment (DME): Custom orthotics, diabetic shoes, braces, and other supportive devices often need pre-authorization.
- Surgical Procedures: Many elective and complex foot and ankle surgeries require extensive prior authorization.
- Advanced Imaging: MRI, CT scans, and sometimes even complex X-rays.
- Certain Medications: Especially high-cost specialty drugs.
The process for obtaining PAs can be time-consuming and varies significantly between payers. It typically involves submitting clinical notes, justification for medical necessity, and sometimes even peer-to-peer reviews.
Effective strategies for managing prior authorizations:
- Payer Portals: Most major payers have online portals specifically for submitting and tracking PAs. These can streamline the process compared to phone calls or faxes.
- Dedicated Staff or Outsourcing: Assigning a dedicated team member or partnering with a specialized billing service to handle PAs can significantly improve efficiency and success rates. Our team has extensive experience navigating these complex requirements.
- Effective Tracking Systems: Implement a system to track the status of all PAs, including submission dates, approval numbers, and expiration dates. This prevents delays and ensures services aren’t rendered without approval.
- Reducing Pre-Auth Denials: The best way to reduce PA denials is to ensure the initial clinical documentation is robust and clearly supports the medical necessity for the requested service. Over time, we learn the specific “hot buttons” for each payer that lead to faster approvals.
Optimizing Your Workflow: Best Practices for Podiatry Claims Processing
The goal of efficient podiatry claims processing isn’t just to get paid, but to get paid quickly and accurately, allowing your practice to thrive. This requires a streamlined workflow, leveraging the right tools, and continuously monitoring your performance.
When we talk about optimizing your workflow, we’re aiming for a high clean claim rate (claims paid on the first submission), a low denial rate, minimal days in A/R (accounts receivable), and an excellent first-pass resolution rate. All of this contributes to robust financial health and compliance.
Technology’s Role in Modern Podiatry Claims Processing
In today’s healthcare landscape, technology is a necessity. It can transform your podiatry claims processing from a manual, error-prone task into an efficient, automated system. For more on this, check out our insights on Technology in Podiatry.
- EHR Integration: A seamless EHR-to-billing platform integration reduces manual data entry and speeds up claim creation. Podiatry-specific EHR templates are crucial for capturing detailed information for complex conditions.
- Practice Management Systems (PMS): A robust PMS acts as the command center for administrative and financial operations, handling everything from scheduling and eligibility to claim submission and payment posting.
- Automated Eligibility Verification: Automated systems verify a patient’s coverage before their appointment, preventing denials from inactive coverage and allowing staff to collect payments upfront.
- Claims Scrubbing Software: Before submission, this software reviews claims for common errors (missing modifiers, incorrect codes) that cause denials, significantly increasing your clean claim rate.
- AI in Coding: AI can suggest CPT and ICD-10 codes based on EHR documentation, reducing coder time per encounter and improving accuracy, which frees up staff for complex tasks.
Key Performance Indicators (KPIs) to Track
To truly understand and improve your practice’s financial health, you need to measure it. Key Performance Indicators (KPIs) are vital metrics that provide a clear picture of your revenue cycle’s efficiency. We believe in living and dying by these metrics, which is why we’ve put together a guide on Live and Die by KPIs: The Podiatrist’s Guide to Practice Growth and Profitability.
Here are some essential KPIs for podiatry practices:
- Net Collection Ratio: The percentage of collectible revenue your practice actually collects. A high ratio indicates efficiency.
- Aged A/R Analysis: Breaks down outstanding A/R by age. The longer a claim is unpaid, the harder it is to collect. Aim for low percentages in the 90+ day category.
- Days in A/R: The average number of days it takes to get paid after a service. Lower is better.
- Clean Claim Rate: The percentage of claims paid on the first submission. Aim for 95% or higher.
- Denial Rate: The percentage of claims denied. This should be as low as possible, ideally under 5%.
- First-Pass Resolution Rate: Measures claims paid on first submission without intervention.
- Cost Per Encounter: The administrative cost per patient visit, used to identify efficiency opportunities.
Regularly tracking these KPIs allows us to identify trends, pinpoint bottlenecks in your podiatry claims processing, and make informed strategic decisions to improve profitability.
Leveraging Specialized Podiatry Billing Services
Given the unique complexities of podiatry claims processing, many practices find immense value in partnering with specialized billing services. Our experience, supporting practices in places like Jersey City, Las Vegas, Omaha, Charlotte, and Ashland, shows that this isn’t just about offloading work; it’s about optimizing your entire revenue cycle.
Benefits of working with a podiatry billing partner like us:
- Specialized Expertise: Our team is intimately familiar with podiatry-specific codes, modifiers, medical necessity rules, and payer policy shifts.
- Reduced Administrative Burden: Outsourcing frees up your in-house team from paperwork and insurance calls to focus on patient care and practice operations.
- Focus on Patient Care: With billing handled by experts, podiatrists can dedicate more time to treating patients, improving their experience and satisfaction.
- Revenue Improvement: A tangible benefit. Practices can see revenue increase up to 20% in 90 days, with a 98% clean claim rate and payments up to 3x faster.
- Scalability: A billing partner scales services to meet your practice’s needs as it grows or experiences seasonal fluctuations, without you hiring more staff.
- Compliance Assurance: Our experts ensure your billing practices are always compliant with regulations like HIPAA and CMS, minimizing audit risks.
By entrusting your podiatry claims processing to specialists, you’re not just hiring a vendor; you’re gaining a partner dedicated to your practice’s financial success and operational efficiency.
Conclusion
Navigating the intricate world of podiatry claims processing is undeniably challenging. From the unique demands of documenting systemic conditions and applying precise modifiers to the ever-changing landscape of Medicare and commercial payer policies, it’s a journey fraught with potential pitfalls. Insufficient documentation, incorrect coding, and a lack of understanding of payer-specific rules can lead to frustrating denials, delayed reimbursements, and a significant drain on your practice’s financial health.
However, with a clear understanding of these complexities, a commitment to meticulous documentation, and the strategic adoption of technology, you can transform your revenue cycle. Tracking key performance indicators provides invaluable insights, while leveraging specialized expertise can lift your practice’s billing efficiency to new heights.
We at Beacon Podiatric Billing Services understand these challenges intimately. Our specialized, 100% US-based team is dedicated to maximizing your collections and streamlining your operations, allowing you to focus on delivering outstanding patient care in New Jersey, Nevada, Nebraska, North Carolina, and Kentucky or any state that you might practice in. Let us be your trusted partner in navigating the complexities of podiatry billing.
Ready to optimize your billing, reduce denials, and improve your financial health? Partner with us to optimize your billing services today!