Podiatry Billing Audit: Top 5 Pitfalls Defused
Why Every Podiatry Practice Needs an Audit-Proof Strategy
Podiatry billing audit failures are costing practices millions, and the stakes have never been higher. Recent government oversight reports reveal that nearly half of sampled podiatry claims failed to meet Medicare requirements, with an estimated $39.6 million in improper payments during just one audit period.
If you’re searching for ways to prevent a podiatry billing audit or prepare for one, here’s what matters most:
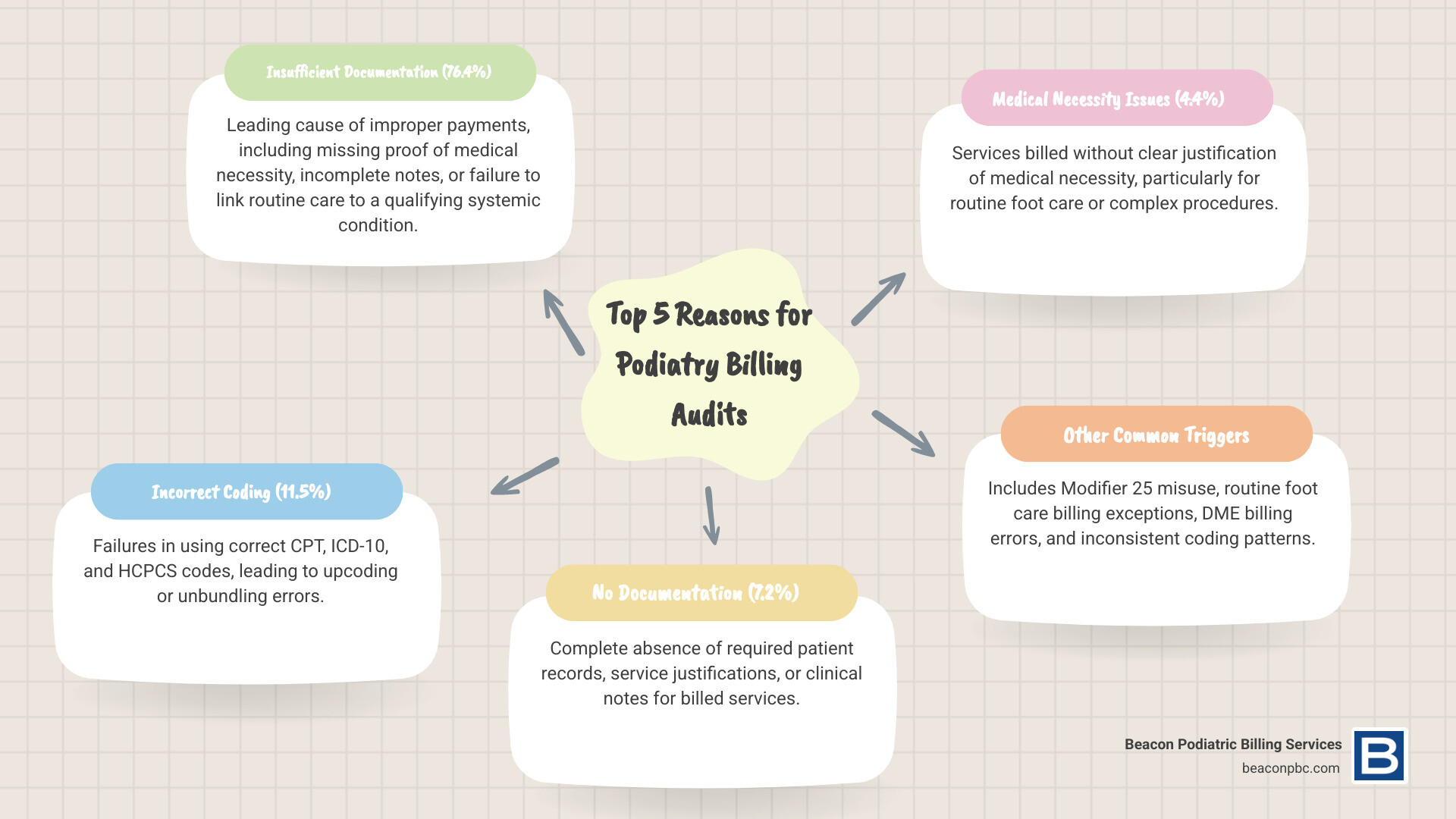
- Insufficient documentation causes 76.4% of improper payments
- Modifier 25 misuse with E/M services is a top audit trigger
- Routine foot care billing requires proof of systemic conditions like diabetes or peripheral vascular disease
- Incorrect coding and medical necessity failures lead to denials and recoupment
- Internal audits conducted quarterly can catch errors before external auditors do
The Office of Inspector General (OIG) found that 44 out of 100 sampled claims didn’t comply with Medicare requirements. That’s not just a compliance problem—it’s a direct threat to your practice’s financial stability.
The good news? Most audit triggers are preventable with the right documentation practices, staff training, and billing expertise.
Medicare Administrative Contractors (MACs) are increasing oversight, and the improper payment rate for podiatry care sits at 11.2%, with a projected $216.9 million in improper payments nationwide. From missing signatures to upcoding lesion counts to billing CAM walkers without proper justification, the margin for error is shrinking.
This guide walks you through the exact strategies to avoid common pitfalls, strengthen your documentation, and build an audit-proof billing process that protects your revenue and keeps you compliant.
Understanding the Podiatry Audit Landscape: Who, Why, and How Much
No podiatry practice wants the hassle and stress of an audit. Yet, the reality is that audits are a growing part of the healthcare landscape, and podiatry practices are increasingly under the microscope. Understanding why audits happen, who conducts them, and their potential financial impact is the first step toward building a resilient, audit-proof practice.
Audits can be triggered by a variety of factors. Sometimes, it’s as simple as random selection. Other times, it’s more targeted: unusual billing patterns, high-cost claims, or inconsistent coding compared to your peers can raise red flags. Even patient or employee complaints can initiate an investigation. Performing services two standard deviations above the mean for your specialty can put you on an auditor’s radar.
The Office of Inspector General (OIG) is a key player in this landscape. The OIG, an official government oversight body, conducts audits and investigations to protect the integrity of Medicare and Medicaid programs. Their reports often highlight areas of concern, and podiatry has been a recurring focus. For instance, a 2010 OIG report found significant Medicare overpayments for Evaluation and Management (E/M) claims due to incorrect coding or documentation. More recently, an audit period found that 44 out of 100 sampled podiatrists’ claims for E/M services did not comply with Medicare requirements. This led to an estimated $39.6 million in improper payments out of $222.5 million paid by Medicare during that audit period.
These findings are not isolated incidents. The overall improper payment rate for podiatry care is a concerning 11.2%, with a projected improper payment amount of $216.9 million. This means a significant portion of Medicare dollars paid for podiatry services are not compliant with regulations.
The consequences of non-compliant podiatry billing can be severe. Beyond recoupment of overpayments, practices can face significant financial penalties, legal action under the False Claims Act, and even exclusion from federal healthcare programs like Medicare and Medicaid. Such actions can cripple a practice’s financial health and damage its reputation, making proactive compliance not just advisable, but essential.
For more insights into managing your practice’s financial health, explore our resources on Practice Management Growth.
The Role of MACs and Local Coverage Determinations (LCDs)
Medicare Administrative Contractors (MACs) are the frontline carriers for Medicare. They process claims, enroll providers, and, crucially for our discussion, are responsible for ensuring program integrity. MACs play a vital role in overseeing Medicare payments and identifying noncompliance. They are tasked with preventing improper payments through education, claim reviews, and referrals for further investigation when necessary.
A critical tool MACs use are Local Coverage Determinations (LCDs). These are detailed, payer-specific rules that outline medical necessity criteria for various services within their specific geographic jurisdiction. For podiatrists in New Jersey, Nevada, Nebraska, North Carolina, or Kentucky, this means understanding the specific LCDs issued by your regional MAC is paramount. These documents clarify what services are considered medically necessary, the conditions that must be met for coverage, and the required documentation.
For example, LCDs are instrumental in defining the exceptions to Medicare’s routine foot care exclusion. They specify the systemic conditions that may justify coverage and the precise documentation needed to support those claims. Staying updated on these policies through MAC articles and communications is not just good practice; it’s a non-negotiable requirement for compliant billing. Ignoring them is a direct path to audit triggers and denials.
Financial Impact of Non-Compliance
The financial implications of non-compliant podiatry billing extend far beyond just repaying claims. As mentioned, the OIG estimated $39.6 million in improper payments for E/M services alone in one audit period, and the projected improper payment amount for podiatry care nationwide is a staggering $216.9 million. These figures represent direct financial losses to the Medicare program, which are ultimately recouped from providers.
However, the impact on individual practices is equally devastating. High denial rates, a direct result of non-compliance, can lead to significant annual revenue loss—estimates suggest denial rates above 10% can cause $80,000–$120,000 in annual revenue loss. Each denied claim means delayed or lost revenue, requiring additional staff time and resources for appeals. The cost of appealing claims can be substantial, with some estimates placing lost revenue from appeals at over $65,000.
Beyond denials, non-compliance can lead to:
- Recoupment: Having to repay Medicare for services already compensated.
- Fines and Penalties: Monetary penalties that can be hundreds of thousands of dollars, especially under the False Claims Act.
- Increased Scrutiny: Once audited, practices often face ongoing, heightened review.
- Exclusion from Federal Programs: The most severe consequence, preventing a practice from billing Medicare or Medicaid, effectively ending its ability to serve a large patient population.
- Reputational Damage: Losing trust within the patient community and among referring physicians.
Maintaining a healthy revenue cycle is crucial for any practice. Keeping a close eye on your financial health KPIs is vital to avoid these pitfalls. Learn more about how to do that on our Financial Health KPIs page.
Top 5 Audit Triggers and How to Defuse Them

Preventing a podiatry billing audit starts with understanding what catches an auditor’s eye. While random audits occur, many investigations are triggered by specific billing patterns or errors. Here are the top five audit triggers in podiatry and how to proactively address them.
1. Insufficient Documentation for Routine Foot Care & E/M Services
This is the undisputed champion of audit triggers, accounting for a whopping 76.4% of improper payments for podiatric providers. If your documentation doesn’t clearly support the services you’ve billed, it’s as good as not having provided the service at all in the eyes of an auditor.
Medicare generally considers routine foot care (RFC)—such as nail trimming, corn or callus removal—as non-covered services. However, there are crucial exceptions, primarily when a systemic condition makes such care medically necessary. These systemic conditions include:
- Diabetes mellitus: Often leading to neuropathy and poor circulation.
- Peripheral Vascular Disease (PVD): Affecting blood flow to the extremities.
- Neurologic conditions: Such as peripheral neuropathies.
For RFC to be covered, your documentation must clearly link the service to one of these qualifying systemic conditions and demonstrate its severity. This includes documenting specific vascular, neurologic, or metabolic findings. For example, simply stating “diabetic patient” is often insufficient. You need to detail how the diabetes impacts the patient’s feet (e.g., absent pulses, trophic changes, loss of protective sensation) and why non-professional care would be hazardous.
Medicare also has specific criteria for “coverage presumption” for RFC, based on what they call Class A, B, and C findings. These findings relate to specific symptoms and conditions (e.g., non-traumatic amputation of foot/leg, absent posterior tibial pulse, claudication). Documenting these objectively and explicitly is crucial.
For Evaluation and Management (E/M) services, documentation must support the chosen level of service. For initial visits, all three components—history, examination, and medical decision-making—must be documented at the same level. For subsequent visits, two out of three components at the same level are usually sufficient. Auditors will carefully review your notes to ensure they justify the E/M code billed.
To dive deeper into these complex requirements, check out our Medicare Podiatry Billing Guidelines. For a broader understanding of how program integrity is maintained, refer to the Medicare Program Integrity Manual.
2. Improper Use of Modifier 25
Modifier 25 is a common audit target, and its misuse can quickly trigger an investigation. This modifier indicates that an E/M service was “significant and separately identifiable” from another procedure performed on the same day by the same provider.
The key here is “significant and separately identifiable.” It’s not enough to simply perform an E/M service and a procedure on the same day. The E/M must be distinct and go beyond the usual pre- and post-operative care inherent in the procedure itself.
Best practices for Modifier 25 use:
- Documentation is paramount: Your chart notes must clearly differentiate the E/M service from the procedure. Document a separate chief complaint, history, exam findings, and medical decision-making that addresses a different problem or a significant exacerbation of the same problem that required additional work beyond the procedure.
- Not for routine follow-ups: If a patient is scheduled for a procedure and the E/M is simply a quick check to ensure they’re ready, Modifier 25 is likely inappropriate.
- Avoid excessive use: If you frequently bill E/M with Modifier 25, especially compared to your peers, it can flag your practice for higher scrutiny.
For a comprehensive look at how to avoid common billing pitfalls, including the correct use of modifiers, read this guide: Billing Pitfalls: How To Avoid An Audit.
3. Incorrect Coding and Medical Necessity
Incorrect coding, including upcoding (billing for a more complex service than performed) and unbundling (billing separately for services that should be bundled), is a direct path to audit failure and potential fraud allegations. Similarly, billing for services that are not medically necessary is a major trigger.
- CPT, ICD-10, HCPCS Updates: The coding landscape is constantly evolving. Medicare’s 2024 revisions to wound debridement codes (11042–11047) caused mass rejections where practices failed to update their systems. Outdated coding practices are often cited as the #1 mistake clinics make. We must stay current with CPT, ICD-10, and HCPCS code changes.
- Justifying Services: Every service you bill must be medically necessary. This means it must be reasonable and appropriate for the diagnosis or treatment of an illness or injury, or to improve the functioning of a malformed body member. Vague terms like “rule out” are insufficient; symptoms should validate diagnostic testing.
- Nail Debridement (11720-11721) and Corn/Callus Removal (11055-11057): These are frequently audited codes. For nail debridement, documentation must specify the number and type of nails treated, the method, and clinical indications (e.g., pain, secondary infection, ambulation limitation). For corn/callus removal, ensure you accurately document the count and location of lesions. Upcoding lesion counts (e.g., billing for “more than four” when only three were documented) is a common error.
4. Durable Medical Equipment (DME) Billing Pitfalls
Billing for Durable Medical Equipment (DME) like splints, braces, or custom orthotics can also be an audit hotspot. Auditors often look for strict adherence to medical necessity and dispensing rules.
- CAM Walkers: These are a frequent target. CMS generally does not allow CAM walkers for ulcer management. There’s also a distinction between codes L4360 and L4361: L4360 requires significant modification by the provider, while L4361 does not. Ensure you’re billing the correct code based on the service provided.
- Medical Necessity Documentation: For any DME, your documentation must include a clear order, explicit medical necessity (why the patient needs it), and the duration of need.
- Dispensing Records: When you dispense DME, you must obtain a signed patient receipt. This receipt should clearly list the item dispensed, provide instructions for usage, and confirm that the item fits properly. Without this, you may struggle to prove the item was provided and properly fitted.
- Prior Authorization: Many DME items require prior authorization. Always secure this beforehand to avoid denials.
5. Key Documentation for Your Next Podiatry Billing Audit
When an auditor comes knocking, your documentation is your first, best, and often only line of defense. Having rock-solid, comprehensive records is non-negotiable. Here’s a list of essential documents and best practices:
- Legible Signatures and Dated Notes: Every entry in the patient’s chart must be signed and dated. Illegible signatures can lead to claims being questioned. Consider maintaining a signature log for all providers and staff.
- Detailed Procedure Reports: For any procedure, your notes must clearly describe what was done, why it was done, and where it was done. Anatomic specificity (e.g., “right great toe nail,” “left 4th metatarsal head”) is crucial.
- Proof of Medical Necessity: This is the overarching theme. For every service, the chart must clearly demonstrate why it was reasonable and necessary. This includes linking routine foot care to qualifying systemic conditions and documenting their severity.
- Patient-Signed Receipts for DME: As mentioned, for any DME dispensed, a signed receipt confirming the item, instructions, and fit is vital.
- Consent Forms: Documenting informed consent for procedures.
- Referral Notes: If a patient was referred, include the referral notes.
- Diagnostic Test Results: All relevant lab, imaging, or diagnostic test results that support your diagnosis and treatment plan.
- Correction Policy: Clearly document any corrections to charts, ensuring they are dated and initialed, never obscuring original entries.
If it’s not documented, it didn’t happen!
Proactive Strategies for a Successful Podiatry Billing Audit

While the idea of a podiatry billing audit can be daunting, a proactive approach can transform it from a threat into an opportunity for growth and compliance. By implementing robust internal strategies, we can identify and correct errors before external auditors do, safeguarding our practice’s financial future.
This means developing comprehensive compliance programs that align with OIG guidelines. These programs should include clear policies and procedures for billing, coding, and documentation. Crucially, they must also incorporate ongoing staff training and continuous education. The OIG has recommended that CMS work with MACs to ensure sufficient oversight and prevent improper payments, and CMS has responded by emphasizing provider education and medical review. This signals a clear need for practices to be vigilant and well-informed.
Conducting an Internal Podiatry Billing Review
One of the most powerful tools in our audit-prevention arsenal is the internal billing review, or self-audit. This process involves periodically checking our own policies, protocols, and chart accuracy, effectively auditing ourselves before an external agency does. The OIG recommends conducting internal audits at least annually. However, many experts, including those in the revenue cycle management field, suggest quarterly reviews. This more frequent cadence allows us to catch and correct errors quickly, especially when new staff are hired or major coding changes occur.
Steps for an effective internal review:
- Define Scope and Responsibility: Determine who will lead the audit (e.g., a designated staff member, an external consultant).
- Sample Selection: Review a random sample of claims. This could be 5-10 claims per provider, focusing on high-risk areas like E/M services with Modifier 25, routine foot care, or DME.
- Claim Analysis Checklist: Use a detailed checklist to evaluate each claim for:
- Documentation completeness and accuracy.
- Medical necessity substantiation.
- Correct CPT, ICD-10, and HCPCS codes.
- Appropriate modifier usage.
- Legible signatures and dates.
- Alignment of services billed with services documented.
- Identify Error Patterns: Don’t just correct individual errors. Analyze the patterns. Are there specific providers consistently miscoding? Are certain services routinely lacking documentation? These insights are crucial for targeted training.
- Implement Corrective Actions: Based on findings, update policies, provide focused staff education, and make necessary adjustments to billing processes. If overpayments are identified, follow MAC guidelines for voluntary refunds.
Conducting regular internal audits not only helps us proactively identify issues but also demonstrates a commitment to compliance, which can be viewed favorably by external auditors. For more on the fundamentals of medical auditing, refer to What Is Medical Auditing? – AAPC.
Keeping Your Coding and Billing Practices Current
The medical billing landscape is a dynamic one, with constant updates from CMS, the American Medical Association (AMA), and various payers. Staying informed about these changes is not just a best practice; it’s a necessity to avoid denials and audit triggers.
- CMS Revisions: CMS frequently revises coding guidelines, coverage policies, and payment rules. For example, the 2024 revisions to wound debridement codes (11042–11047) caused significant issues for practices that failed to implement the updates. We must diligently monitor CMS announcements and implement changes immediately.
- AMA Announcements: The AMA is responsible for CPT codes, and updates to these codes are released annually and sometimes quarterly. These changes can impact how we bill for common podiatric procedures.
- Payer Policy Changes: Each MAC and private payer may have specific policies that differ slightly. Regularly reviewing their local coverage determinations (LCDs) and billing articles ensures we are always compliant with their specific requirements.
To help you stay on top of these crucial updates, we regularly publish insights and guidance on our Billing and Coding Updates page.
The Advantage of Specialized Podiatry Billing Expertise
While general medical billing firms handle a wide range of specialties, podiatry has unique billing complexities that often require specialized expertise. This is where a dedicated podiatry billing service like ours truly shines.
| Feature | Specialized Podiatry Billing | General Billing |
|---|---|---|
| Clean Claim Rate | 96%+ | 85% |
| Average AR Days | 30 | 50+ |
| Appeals Win Rate | 78% | 45% |
Source: Industry data and RevCycleIntelligence survey
Why does specialized expertise make such a difference?
- Podiatry-Specific Nuances: We understand the intricate details of LCD adherence for routine foot care, the correct application of Q-modifiers (specific to podiatry), and complex bundling edits that general firms often miss.
- Modifier Expertise: Our team possesses in-depth knowledge of modifiers like 25, 59, Q7, Q8, Q9, and their precise application in podiatry, which are frequent audit targets.
- Higher First-Pass Acceptance Rate: Clinics that invest in specialized podiatry billing services see a 20–25% higher first-pass claim acceptance rate. This translates directly to faster reimbursements and improved cash flow for practices in New Jersey, Nevada, Nebraska, North Carolina, and Kentucky.
- Reduced Overhead and Compliance Risk: Outsourcing to podiatry billing specialists can save clinics 20–30% annually compared to in-house teams, while significantly lowering compliance risk.
- Faster Reimbursements: Our outsourced teams ensure claims are submitted within 24–48 hours, leading to quicker payments.
We are 100% US-based, offering dedicated, podiatry-specific expertise and personalized service to maximize your collections and streamline your operations. Learn more about how technology supports efficient practice management on our Technology in Podiatry page.
Frequently Asked Questions about Podiatry Billing Audits
What is the #1 reason for podiatry claim denials and audit failures?
The leading cause of podiatry claim denials and audit failures is insufficient documentation, accounting for a staggering 76.4% of improper payments. This includes a range of issues such as missing proof of medical necessity, incomplete or illegible notes, or the failure to adequately link routine foot care to a qualifying systemic condition like diabetes or peripheral vascular disease. If the medical record doesn’t clearly support the billed service, it will likely be denied or flagged during an audit.
How often should a podiatry practice conduct internal reviews?
Best practice, as recommended by the OIG, is to conduct internal reviews at least annually. However, many compliance experts and revenue cycle management professionals suggest quarterly reviews to catch and correct errors more quickly. More frequent audits are particularly beneficial when new staff are hired, when there are significant changes to coding guidelines (like CMS revisions), or if your practice identifies a pattern of denials for specific services. Regular internal audits demonstrate a commitment to compliance and can significantly mitigate the risk of external audits.
What are the consequences of failing a Medicare audit?
The consequences of failing a Medicare audit can be severe and multifaceted. They range from recoupment of overpayments (having to pay back money already received) to significant financial penalties under the False Claims Act, which can include treble damages (three times the amount of the overpayment) plus substantial fines per claim. In cases deemed to involve fraud or abuse, a provider can face exclusion from federal healthcare programs like Medicare and Medicaid, effectively ending their ability to practice medicine for a large segment of the population. In the most severe instances, providers may even face criminal charges. Beyond the direct financial and legal repercussions, failing an audit can lead to increased scrutiny from payers, damage to the practice’s reputation, and a loss of trust from patients and referring physicians.
Secure Your Practice’s Financial Health
Navigating the complex world of podiatry billing audit requirements and compliance can feel like walking a tightrope. However, by understanding the common pitfalls and implementing proactive strategies, your practice can not only avoid costly audits but also optimize its revenue cycle.
The key takeaways are clear: meticulous documentation is your best defense, staying current with coding and payer policies is non-negotiable, and implementing regular internal audits is essential. Don’t underestimate the financial implications of non-compliance; improper payments and denials can severely impact your practice’s stability.
At Guide Podiatric Billing Services, we understand these challenges deeply. Our specialized, 100% US-based team offers the expertise your practice needs to maximize collections, streamline operations, and ensure unwavering compliance. We are dedicated to providing podiatry-specific knowledge and personalized service to practices across New Jersey, Nevada, Nebraska, North Carolina, and Kentucky.
Don’t wait for an audit to highlight your vulnerabilities. Take control of your practice’s financial health today.