Medical billing for podiatrists: Master 2026
Why Medical Billing for Podiatrists Demands Specialized Attention
Medical billing for podiatrists is fundamentally different from general medical billing, and getting it wrong costs practices thousands of dollars every month in lost revenue.
Quick Answer: What Makes Podiatry Billing Unique?
Medical billing for podiatrists requires specialized knowledge because:
- Routine care is typically non-covered unless linked to systemic conditions like diabetes or peripheral vascular disease
- Medicare patients make up a large portion of most podiatry practices, requiring precise compliance with complex rules
- Class findings must be documented to justify coverage for services like nail debridement
- Specialized modifiers (Q7, Q8, Q9, TA-T9) are essential for accurate reimbursement
- Mixed medical and surgical services often happen in the same visit, demanding careful coding
- High denial rates occur when diagnosis codes don’t properly support procedures
If you’re a podiatrist, you already know this reality. You perform a routine nail debridement for a diabetic patient with neuropathy. You document everything carefully. You submit the claim. Then it gets denied because you missed a required Q modifier or didn’t code the systemic condition correctly.
The problem isn’t just one denied claim. It’s the pattern. Missing a required diagnosis code triggers a denial. Misapplying a modifier triggers an audit. Billing routine care without documenting class findings triggers a compliance review.
This guide cuts through the complexity. You’ll learn exactly which codes and modifiers to use, how to document medical necessity properly, and how to build a workflow that prevents denials before they happen.
The stakes are high. Podiatry practices face unique billing complexities that directly affect revenue and operational efficiency. But with the right knowledge and systems, you can turn your billing operation from a constant headache into a reliable revenue engine.
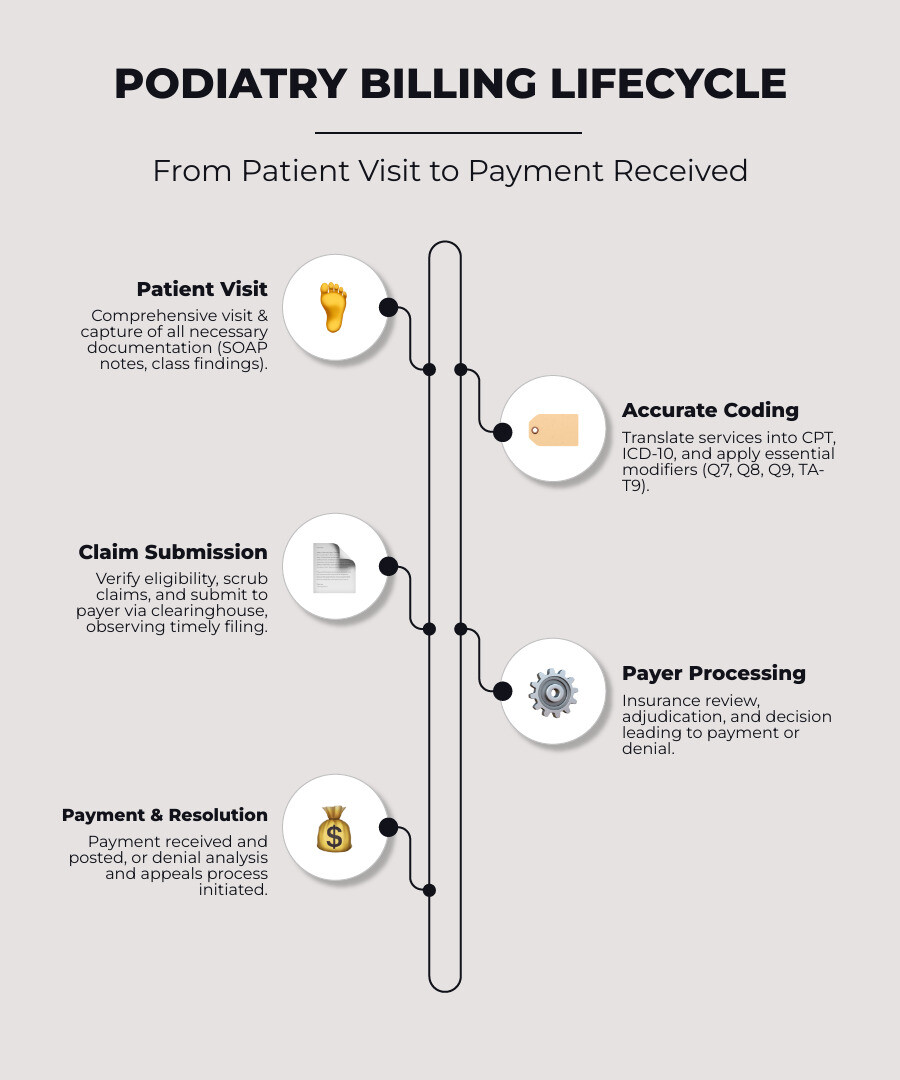
Why Podiatry Billing is a Unique Challenge
Medical billing for podiatrists is unlike other specialties. It involves a unique blend of routine care, chronic conditions, and complex surgical interventions, all governed by payers with very specific rules.
A primary distinction is the high percentage of Medicare beneficiaries in podiatry practices. Older patients often have systemic conditions like diabetes, peripheral vascular disease, and neuropathy that affect foot health. This makes navigating Medicare’s intricate rules for routine foot care essential for a practice’s financial health, as minor missteps often lead to denials.
Furthermore, podiatrists frequently provide a mix of medical and surgical services in a single visit, such as a check-up and an ingrown toenail removal. Accurately billing for these distinct services requires specialized CPT and ICD-10 codes, plus crucial modifiers to signify separate procedures. Without this precision, claims are often denied.
The need for pre-authorization is another hurdle. Services like custom orthotics or certain surgeries often require prior approval from insurers. Missing this step results in denials, regardless of medical necessity, adding another layer of administrative complexity.
These challenges contribute to high denial rates for podiatry practices. Missing a diagnosis code, misapplying a modifier, or failing to document “class findings” can trigger denials, impacting revenue. This underscores why specialized knowledge in medical billing for podiatrists is critical.
For a deeper dive into Medicare’s specific rules, you can refer to our guide on Demystifying Medicare Podiatry: What’s Covered, When, and How to Calculate Costs.
The Routine Foot Care Dilemma
Perhaps the most significant challenge in medical billing for podiatrists is “routine foot care.” Unlike in other specialties, services like nail trimming or callus paring are generally considered non-covered by Medicare and many commercial payers unless a specific, underlying systemic condition is present and properly documented.
Crucial exceptions exist. If a patient has a systemic condition that increases their risk of foot complications, routine foot care can become medically necessary and covered. The key systemic conditions include:
- Diabetes: Patients with diabetes are highly susceptible to neuropathy, poor circulation, and infections.
- Peripheral Vascular Disease (PVD): This condition restricts blood flow, leading to slow healing and increased infection risk.
- Neuropathy: Nerve damage can lead to loss of sensation, making patients unaware of injuries.
For these conditions, Medicare requires documented “class findings”—physical signs indicating the severity and risk. Without clear documentation of these findings, even for a diabetic patient, a routine foot care claim will likely be denied. This meticulous documentation requirement is a major reason medical billing for podiatrists requires specialized expertise.
Navigating Payer-Specific Nuances
While Medicare sets a high bar, practices must also contend with various commercial insurance policies, each with its own rules and reimbursement rates. This variability adds complexity to medical billing for podiatrists.
Medicare’s rules are stringent, especially for routine foot care. They dictate frequency limits (e.g., once every 60 days), require specific modifiers, and mandate class findings. The Medicare Physician Fee Schedule (PFS) also adjusts payments annually, so practices must stay current.
Commercial payer policies can differ significantly. Some plans may be less restrictive for routine care, while others are stricter than Medicare. Prior authorizations for procedures and durable medical equipment (DME) like orthotics are often more common with commercial insurers.
Workers’ Compensation cases have their own unique billing forms, narrative reports, and submission processes. Managing these inconsistent policies across all payers demands vigilance and adaptability from your billing team.
Mastering Podiatry Codes, Modifiers, and Documentation
Accuracy in coding and thorough documentation are the pillars of successful medical billing for podiatrists. Without them, even medically necessary services can go unpaid. You must use the correct CPT, ICD-10, and modifier codes to paint a clear picture for payers.
Essential CPT Codes for Medical Billing for Podiatrists
CPT codes describe the procedures and services performed. For podiatrists, understanding the nuances of these common codes is vital for accurate reimbursement.
Here are some of the most common CPT codes in podiatry:
- Nail Debridement:
11720: Debridement of nail(s) by any method(s); 1 to 5 nails11721: Debridement of nail(s) by any method(s); 6 or more nails- These codes are sensitive to medical necessity documentation and often require Q modifiers for Medicare.
- Callus Removal:
11055: Paring or cutting of benign hyperkeratotic lesion (e.g., corn or callus); single lesion11056: Paring or cutting of benign hyperkeratotic lesion (e.g., corn or callus); two to four lesions11057: Paring or cutting of benign hyperkeratotic lesion (e.g., corn or callus); more than four lesions- Medical necessity for these codes hinges on systemic conditions.
- Injections:
20550: Injection(s); tendon sheath, or ligament, aponeurosis (e.g., plantar “fascia”)20610: Arthrocentesis, aspiration and/or injection; major joint or bursa- Often used for pain management, such as for plantar fasciitis.
- Hammertoe Correction:
28285: Correction, hammertoe (e.g., interphalangeal fusion, partial or total phalangectomy)- This surgical code often requires pre-authorization.
- Orthotics:
L3020: Foot orthosis, insert, removable, molded to patient model, custom fabricated, heel cup- Orthotics are billed using HCPCS L-codes and frequently require prior authorization and detailed documentation.
The “no diagnosis, no dollars” principle applies. Every CPT code must be supported by an appropriate ICD-10 diagnosis code that justifies medical necessity.
The Role of ICD-10 Codes in Proving Medical Necessity
While CPT codes say what was done, ICD-10 codes explain why. These diagnosis codes are paramount for proving medical necessity, especially when distinguishing between routine and covered care.
Always use the highest level of specificity and laterality. For example, use M79.671 for “Pain in left foot” instead of a generic “foot pain” code. This detail helps payers understand the condition. When billing for services that could be considered routine, link them to appropriate systemic condition codes, like E11.621 (Type 2 diabetes mellitus with diabetic foot ulcer).
Common ICD-10 diagnoses in podiatry include:
M77.31: Plantar fasciitis, right footM77.32: Plantar fasciitis, left footL60.0: Ingrowing nailL84: Corns and callositiesM79.671: Pain in left footM79.672: Pain in right footE11.621: Type 2 diabetes mellitus with diabetic foot ulcerI70.201: Unspecified atherosclerosis of native arteries of right leg, with intermittent claudication (for PVD)G62.9: Polyneuropathy, unspecified (for neuropathy)
The precise linkage between diagnosis and procedure codes justifies reimbursement.
Crucial Modifiers for Accurate Reimbursement
Modifiers are two-character codes added to CPT codes to provide more information. In podiatry, they can make or break a claim.
- Q Modifiers (Q7, Q8, Q9): These are critical for Medicare routine foot care, indicating the presence of “class findings” that justify medical necessity:
Q7: One Class A finding (Non-traumatic amputation of foot or integral skeletal portion)Q8: Two Class B findings (e.g., absence of pulses, advanced trophic changes)Q9: One Class B and two Class C findings (e.g., claudication, edema, paresthesia)- These must be used correctly with CPT codes like 11721-Q8 for Medicare reimbursement.
- Toe Modifiers (TA-T9): Specify which toe was treated (e.g.,
TAfor left great toe). Essential for procedures on specific digits. Note: not typically used for codes like11720and11721. - -25 Modifier (Significant, Separately Identifiable E/M Service): Used on an E/M code when a significant, separate E/M service is performed on the same day as a minor procedure.
- -59 Modifier (Distinct Procedural Service): Indicates two or more procedures on the same day were distinct (e.g., different locations), like removing a callus (11055) and a wart (17110) in the same visit.
- LT/RT Modifiers: Indicate laterality (left or right) for bilateral procedures.
Proper modifier application is a nuanced art, and misuse is a frequent cause of denials.
Documentation: Your First Line of Defense
If coding is the language of billing, documentation is its grammar. Thorough and compliant documentation is your best defense against denials and audits in medical billing for podiatrists.
The SOAP format (Subjective, Objective, Assessment, Plan) remains the gold standard. Every note should detail:
- Subjective: Patient’s chief complaint.
- Objective: Physical exam findings, including specific class findings.
- Assessment: Your diagnosis.
- Plan: Treatment provided, patient education, and follow-up.
For routine foot care under Medicare, documenting class findings is paramount to prove medical necessity. For example, when performing nail debridement for a diabetic patient, notes must describe the specific signs of neuropathy or PVD. For these patients, documentation should also show that a managing physician has seen them for the systemic condition within the last six months. This supports medical necessity and demonstrates coordinated care.
Comprehensive documentation supports your codes and protects you in an audit. Learn more about optimizing your practice management through our resources on More on practice management.
Best Practices for Flawless Medical Billing for Podiatrists
Flawless medical billing for podiatrists requires robust best practices. This means a proactive approach to claim submission, diligent denial management, and staying informed about evolving regulations.

A Step-by-Step Claim Submission Workflow
A defined claim submission workflow is critical to minimize errors and maximize your first-pass resolution rate.
- Insurance Eligibility Verification: Before the appointment, verify active coverage, benefits, and prior authorization needs. Automated checks prevent denials from inactive coverage and save time.
- Accurate Data Entry: Ensure all patient demographics and insurance information are entered correctly.
- Claim Scrubbing: Before submission, use software or clearinghouse tools to scrub claims for common coding errors, missing modifiers, or incompatible code pairings.
- Clearinghouse Submission: Submit claims electronically through a clearinghouse for streamlined processing and tracking.
- Timely Filing Deadlines: Be aware of each payer’s timely filing limits (from 30 to 365 days) to avoid forfeiting reimbursement.
Effective Denial Management and Appeals
Denials are inevitable, but effective management is key to your practice’s financial health. Common podiatry denial reasons include lack of medical necessity, missing documentation of class findings, incorrect modifiers, and missing prior authorizations.
A systematic approach to denial management is crucial:
- Analyze Denial Reasons: Log each denial and its reason to identify patterns and address root causes.
- Timely Action: Act on denied claims within a day, adjusting and resubmitting promptly.
- The Appeals Process: For claims requiring an appeal, submit medical records and a letter of appeal within the payer’s deadline (often 30-90 days). Check Correct Coding Initiative (CCI) edits for bundling issues.
- Track Financial KPIs: Regularly track KPIs like your clean claim rate and denial rate to gauge billing effectiveness. Our guide, Live and Die by KPIs: The Podiatrist’s Guide to Practice Growth and Profitability, offers further insights.
Staying Current with Billing and Coding Updates
The healthcare landscape is always changing. For medical billing for podiatrists, staying current with updates is non-negotiable for maintaining compliance and optimizing revenue.
- Annual CPT and ICD-10 Changes: Integrate annual code set revisions into your workflows promptly.
- Payer Policy Updates: Routinely check payer websites and subscribe to newsletters for updates to local and national coverage determinations (LCDs and NCDs).
- Staff Training: Continuous training for billing staff is paramount to ensure accuracy. Our resources under Category: Billing & Coding Updates can help.
- CMS Billing Examples: Refer to resources like the CMS billing examples for guidance on filling out the CMS-1500 form.
Optimizing Your Revenue Cycle: Choosing the Right Billing Solution
In the complex world of medical billing for podiatrists, choosing the right billing solution is paramount to optimizing your revenue cycle and fostering practice growth. The challenges are too significant, and the stakes too high, to settle for anything less than specialized expertise and efficient workflows.
| Feature / Approach | Expertise & Compliance | Efficiency & Workflow | Cost-Effectiveness |
|---|---|---|---|
| Specialized Podiatry Billing Services | High (dedicated experts) | High (streamlined processes, advanced tech) | High (reduced denials, maximized collections) |
| General Billing Services | Moderate (may lack podiatry specifics) | Moderate (generic processes) | Moderate (potential for more denials) |
| In-House Billing | Varies (requires continuous training) | Moderate (depends on staff and tech) | Moderate (high overhead for training, tech) |
The Benefits of Specialized Medical Billing for Podiatrists
The unique complexities of podiatry billing mean that a one-size-fits-all approach simply won’t cut it. That’s why specialized medical billing for podiatrists offers distinct advantages:
- Expertise and Compliance: Specialized services possess in-depth knowledge of podiatry-specific CPT and ICD-10 codes, modifiers (like the crucial Q modifiers and toe modifiers), and documentation requirements. This expertise ensures claims are submitted correctly, minimizing denials and maintaining compliance with ever-changing payer regulations.
- Maximized Reimbursements: With a deep understanding of payer policies, including Medicare’s stringent rules and varied commercial insurer guidelines, specialized billers can identify opportunities for legitimate reimbursement that might otherwise be missed. This translates directly into higher collection rates and improved cash flow.
- Reduced Administrative Burden: By entrusting billing to dedicated experts, our practice staff can focus more on patient care and clinical operations, rather than getting bogged down in complex coding, claim submissions, and denial appeals. This improves practice efficiency and reduces burnout.
- Cost-Effectiveness: While there’s an investment, the benefits often outweigh the costs. Specialized services typically lead to fewer denials, faster payment cycles, and a higher net collection rate, ultimately improving your practice’s profitability. They also eliminate the need for significant in-house investment in billing software, training, and staff salaries.
Finding the right partner is crucial. You can explore 5 Proven Ways to Find a Podiatry Billing Company to guide your search.
Leveraging Technology for a Streamlined Workflow
Technology plays a pivotal role in modern medical billing for podiatrists, changing workflows and boosting efficiency.
- EHR Integration: Seamless integration between your Electronic Health Record (EHR) system and billing software is fundamental. This ensures that clinical documentation flows directly to billing, reducing manual data entry errors and streamlining the coding process.
- Practice Management Software: Robust practice management software helps organize patient information, schedule appointments, manage claims, and track financial performance, providing a comprehensive overview of your practice’s operations.
- Automated Eligibility Checks: Automated systems for verifying patient insurance eligibility before appointments save valuable time and prevent denials due to inactive coverage or benefit limitations.
- Reporting and Analytics: Advanced billing solutions provide detailed reporting and analytics. These insights help identify trends in denials, track reimbursement rates, and pinpoint areas for improvement, allowing for data-driven decision-making to optimize your revenue cycle.
For practices looking to upgrade their systems, finding an EHR that integrates seamlessly with billing is key. Consider our insights on Navigating Your Transition from TrakNet: Find Your Perfect EHR Match with Beacon.
Frequently Asked Questions about Podiatry Billing
What are the most common reasons for podiatry claim denials?
The most common reasons stem from the specialty’s complexities:
- Lack of medical necessity for routine care: Claims for services like nail trimming are often denied if not explicitly linked to a systemic condition (e.g., diabetes, PVD) and supported by documented class findings.
- Missing or incorrect modifiers: Forgetting a Q modifier for Medicare routine foot care, or misusing the -25 or -59 modifiers, can lead to immediate denials.
- Inadequate documentation of class findings: If the specific physical signs (class findings A, B, or C) are not clearly documented, Medicare will deny the claim for routine foot care, even if a systemic condition exists.
- Missing prior authorizations: Many advanced procedures, custom orthotics, and certain durable medical equipment require pre-approval. Submitting a claim without this authorization will result in a denial.
- Incorrect ICD-10 coding: Using a non-specific diagnosis code or one that doesn’t adequately support the CPT code is a common pitfall.
What are “Class Findings” for Medicare routine foot care?
“Class findings” are specific physical signs that prove a patient’s systemic condition (like diabetes or PVD) makes routine foot care medically necessary. Medicare requires these findings to be documented to cover services that would otherwise be considered routine. They are used with Q modifiers (Q7, Q8, Q9) and are categorized as follows:
- Class A Finding: Non-traumatic amputation of foot or integral skeletal portion.
- Class B Findings: Absence of posterior tibial pulse, absence of dorsalis pedis pulse, or advanced trophic changes (e.g., hair loss, nail thickening, skin atrophy).
- Class C Findings: Claudication, capillary filling time of greater than 5 seconds, edema, paresthesia, or deformity of the foot/toes.
For example, to use the Q8 modifier, you must document two Class B findings. To use the Q9 modifier, you must document one Class B and two Class C findings.
When should I use Modifier 25 versus Modifier 59?
These two modifiers are frequently confused but serve distinct purposes in medical billing for podiatrists:
-
Modifier -25 (Significant, Separately Identifiable E/M Service):
- When to use: Append to an Evaluation and Management (E/M) code (e.g., 99213) when a significant, separate E/M service is performed by the same physician on the same day as a minor procedure.
- Example: A patient receives an ingrown toenail removal. During the visit, they also discuss new neuropathy symptoms, leading to a separate exam and treatment plan. The E/M code for the neuropathy workup would get the -25 modifier.
-
Modifier -59 (Distinct Procedural Service):
- When to use: Append to a procedure code to show it was a distinct procedural service, separate from other procedures performed on the same day (e.g., different anatomical site, different session).
- Example: A callus is removed (CPT 11055) from the ball of the left foot and a wart is removed (CPT 17110) from the right heel during the same visit. You would append -59 to one of the procedure codes to indicate its distinctness. Avoid using -59 when a more specific modifier (like LT/RT or toe modifiers) would better describe the situation.
Conclusion
Navigating the intricacies of medical billing for podiatrists is undeniably challenging, with its unique blend of routine care considerations, the prevalence of Medicare patients, specialized coding, and rigorous documentation requirements. We’ve explored how seemingly minor details, like the correct application of a Q modifier or the precise documentation of class findings, can significantly impact your practice’s revenue and operational efficiency.
The good news is that you don’t have to tackle these complexities alone. By understanding the specific challenges, mastering the essential codes, modifiers, and documentation best practices, and leveraging the right solutions, you can transform your billing operations. Our specialized expertise in medical billing for podiatrists is designed to maximize your collections, streamline your workflows, and ensure compliance, allowing you to focus on what you do best: providing exceptional patient care.
Ready to turn your billing challenges into revenue opportunities? Get a free billing audit and see how our specialized Billing Services can boost your revenue. Let us help you write your next chapter of practice growth and financial success.